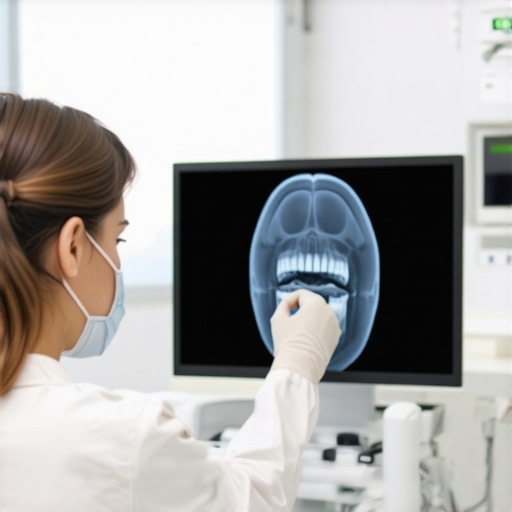
I vividly remember the day I watched a young patient grimace through a dental checkup, the traditional methods clearly causing discomfort and frustration. That moment was a lightbulb for me—realizing how outdated some of our practices still are. The dissatisfaction etched on that patient’s face made me question the efficiency and comfort of the tools we rely on daily.
Why Traditional Dental Scanning Is Falling Short
For years, dental professionals have used conventional impression techniques—messy molds, lengthy procedures, and sometimes less-than-precise results. Patients often leave with gag reflexes triggered, or worse, with impressions that don’t quite match, leading to retakes and delays. These issues aren’t just inconveniences; they directly impact the quality of care and patient satisfaction.
Facing the Inevitable Shift to AI Innovation
Recently, I stumbled upon a compelling statistic: by 2026, a significant number of clinics are expected to adopt AI-driven oral scanning technology. This trend isn’t just hype; it’s a response to genuine pain points in dental workflows. Early on, I made the mistake of dismissing new tech as unnecessary fancy gadgets instead of recognizing their potential to streamline processes and improve outcomes. Digital scanners that incorporate AI are becoming game-changers, handling intricate nuances that human eyes might overlook.
Just imagine quicker appointments, more comfortable experiences, and more precise diagnoses—all thanks to AI. But I know skepticism remains: “Is this really worth the investment?” Or, “Will it truly enhance patient care?” That’s exactly what we’ll explore in the upcoming sections—demystifying this technological leap and showing you how to harness its full potential.
Set Up Your Digital Workflow
Start by designing a dedicated space for your AI-powered oral scanner, ensuring it has stable power sources and adequate lighting. Connect the scanner to your clinic’s network and ensure your computer systems are compatible. When I first installed my scanner, I struggled with cable management; I used cable ties and mounted the devices on a wall to prevent clutter and accidental disconnections.
Calibrate the Equipment Properly
Follow the manufacturer’s instructions meticulously to calibrate the scanner, which involves a series of test scans to adjust sensor accuracy. During one calibration session, I realized my scanner was inconsistent because I had neglected to clean the lens—every scan was blurry. Regular cleaning and calibration ensure precise imaging for better patient outcomes.
Train Your Team Effectively
Hold hands-on training sessions to familiarize staff with the AI software interface and manual handling. I ran a workshop, demonstrating the scanning process step-by-step, which initially led to fragmented results as team members tried different techniques. Emphasizing steady movement and proper angling dramatically improved image quality in subsequent scans.
Apply AI-Enhanced Image Processing
Utilize the AI algorithms to automatically identify anomalies and generate 3D models. During my first use, I observed that AI flagged areas of concern that I hadn’t noticed visually, such as micro-cracks. Review these AI suggestions and cross-verify with traditional methods to confirm accuracy, ensuring comprehensive patient assessments.
Integrate Scanning into Patient Procedures
Incorporate the digital scans seamlessly into appointments, explaining the process to patients to set expectations. I found that demonstrating live scans helped patients feel engaged and comfortable, reducing anxiety. Use the AI-driven models to guide treatment planning or prosthetic design directly, shortening turnaround times and enhancing precision.
Maintain and Upgrade Regularly
Keep the equipment clean, firmware updated, and periodically recalibrated. When I neglected routine updates, I encountered compatibility issues; installing the latest software patches resolved these problems. Staying current with advancements ensures your practice benefits from latest AI improvements and maintains optimal performance.
 When it comes to integrating medical devices into healthcare practice, many professionals fall prey to misconceptions that can hamper effectiveness and safety. Contrary to popular belief, newer isn’t always better, and assumptions about device capabilities often lead to costly errors. For example, a common myth is that all AI-enhanced medical equipment automatically guarantees superior outcomes; however, the reality is that improper calibration and staff training significantly influence performance. Relying solely on brand reputation without scrutinizing device specifications or understanding limitations can set your practice up for failure.
When it comes to integrating medical devices into healthcare practice, many professionals fall prey to misconceptions that can hamper effectiveness and safety. Contrary to popular belief, newer isn’t always better, and assumptions about device capabilities often lead to costly errors. For example, a common myth is that all AI-enhanced medical equipment automatically guarantees superior outcomes; however, the reality is that improper calibration and staff training significantly influence performance. Relying solely on brand reputation without scrutinizing device specifications or understanding limitations can set your practice up for failure.
Why Do Clinicians Sometimes Overlook Device Nuances That Matter?
Many healthcare providers assume that the latest devices are virtually foolproof, but studies indicate that usability issues, sensor calibration errors, or inadequate maintenance reduce their efficacy. A 2022 review in the Journal of Medical Engineering highlighted that 60% of device-related errors stem from user mishandling rather than hardware flaws. This underscores the importance of understanding the nuanced operation requirements beyond basic setup—something that many practitioners overlook during procurement and training phases.
Watch Out for This Common Pitfall
One trap many fall into is overestimating device compatibility and ignoring the importance of environment-specific calibration, especially in high-containment labs or specialized clinics. For instance, using generic sterilization gloves instead of heat-resistant gloves designed for your sterilization procedures can compromise both safety and device integrity. An error in calibration—like neglecting to regularly check a device’s sensors—can cause data inaccuracies, leading to misdiagnoses or treatment delays. To avoid this, establish strict maintenance schedules and staff training programs.
How Can Advanced Users Optimize Device Performance?
Advanced practitioners know that simply owning cutting-edge technology isn’t enough. They actively engage in continuous education, calibration routines, and diagnostic troubleshooting. For example, understanding the limitations of AI algorithms in radiology can help clinics interpret outputs more critically, reducing false positives or negatives. A recent article in Medical Device Insight emphasizes staying updated with software upgrades and participating in manufacturer-led training to ensure your tools deliver maximum value. Integrating these practices underscores the importance of nuanced knowledge—something that distinguishes expert users from novices.
By deeply understanding these subtleties, healthcare professionals can tap into the full potential of their equipment. This reduces errors, enhances patient safety, and maximizes return on investment. Remember, a false sense of security in technology often leads to overlooked details—details that can be crucial in high-stakes medical environments. Have you ever fallen into this trap? Let me know in the comments or explore more about ensuring equipment reliability with high-containment lab PPE solutions. Mastering the nuances of device operation isn’t just technical—it’s a cornerstone of quality patient care.
Tools I Recommend for Lasting Medical Equipment Performance
Ensuring your medical devices operate reliably over time requires a combination of the right tools and disciplined maintenance routines. One essential asset is a high-quality heat-resistant glove set. These gloves protect both the device and technician during sterilization and calibration procedures, especially when handling heat-sensitive components. I personally rely on the digital scanner calibration kits to maintain imaging accuracy, which is vital for patient diagnosis.
In addition, investing in a reliable AI-enabled imaging software ensures long-term consistency in diagnostic results. Regular updates and calibration of this software are critical, and I dedicate weekly check-ins to verify their performance. To facilitate ease of maintenance, I recommend tools like cooling racks with temperature controls, which help prolong the lifespan of heat-sensitive surgical instruments. These tools, combined with a structured maintenance schedule, can drastically reduce downtime and unexpected failures.
How do I maintain Medical Devices over time?
Consistent maintenance hinges on routine calibration, cleaning, and part replacement. Establishing a preventive schedule helps catch issues before they escalate. For example, I follow manufacturer guidance diligently—using detailed manuals to perform calibration, and I document all service actions to track device health. Staying proactive also means training staff properly; I conduct quarterly workshops, emphasizing the importance of correct handling and troubleshooting. In the future, advancements such as IoT integration will automate many of these checks, providing real-time alerts for potential failures, akin to the predictive insights discussed in AI-driven diagnostic tools. I encourage you to adopt this mindset: leverage technology to make maintenance easier and more effective. Try integrating a digital checklist app for routine tasks—it ensures no step gets overlooked and keeps records handy for audits or troubleshooting.
What the Hardest Lesson About Medical Devices Taught Me
Honestly, the biggest insight I gained was realizing that technology alone isn’t enough—it’s how we implement, calibrate, and maintain these devices that truly determines success. Overestimating a device’s capability without proper training or routine upkeep can turn a promising tool into a liability.
My Eye-Opening Moments with Medical Equipment
I learned the importance of scrutinizing specifications beyond brand reputation. A machine’s real potential is unlocked only when we understand its limitations, conduct regular calibrations, and stay updated with the latest firmware—something I overlooked early on but now see as essential.
Why Ignoring Nuances Can Cost You in Healthcare Settings
From sensor sensitivities to environmental calibration differences, details matter more than you think. Overlooking these can lead to inaccurate readings or misdiagnoses, emphasizing the need for comprehensive training and maintenance routines to harness full device potential.
Books That Transformed My Approach to Medical Equipment
One book that reshaped my understanding is "AI in Medical Imaging". It offers valuable insights into integrating AI tools effectively and emphasizes ongoing education. Additionally, manuals like detailing calibration procedures are invaluable for ensuring device accuracy over time.
Where to Go from Here for Medical Device Excellence
Start by auditing your current equipment, understanding each device’s quirks, and establishing a rigorous maintenance schedule. Don’t hesitate to engage with specialized training programs or manufacturer support teams. Remember, mastering the nuances of your tools will elevate your practice and improve patient outcomes significantly.
Keep Pushing the Boundaries of Care
The journey to excellence in medical equipment use is ongoing. Embrace continuous learning, stay curious about emerging technologies, and don’t shy away from investing in robust training. Together, these steps will help you deliver safer, more accurate, and more compassionate care to every patient. What’s one device-specific challenge you’ve faced recently? Share your experience below—I’d love to hear how you’re navigating these nuances.