There was a moment in my clinic when I watched a patient freeze at the sight of a syringe, their face pale, eyes wide with panic. It reminded me of my own childhood fears, but this wasn’t just a moment of discomfort — it was a barrier to proper care. That day, I realized traditional injections aren’t just about pain; they’re about fear, anxiety, and often, shame.
Ending the Needle Phobia Nightmare with Technology
If you’ve ever hesitated before a simple shot, feeling your pulse race or your palms sweat, you’re not alone. Needle-phobia affects up to 10% of the population, making routine injections a source of unnecessary distress. But what if we could make injections virtually painless and anxiety-free? That’s where 3 Smart Needle Injectors for Needle-Phobic Patients come into play. These innovative devices promise to transform the experience, turning fear into calm, and discomfort into confidence.
Can These Devices Truly Replace Traditional Needles?
When I first heard about them, I was skeptical — after all, can technology really reduce such deep-seated fears? My early mistake was assuming that if something is high-tech, it must be complicated and unreliable. But after testing a few models, I saw how intelligent design and gentle operation make a world of difference. For instance, some injectors use controlled, pulsed delivery to minimize pain and anxiety, making even the most needle-averse patients more willing to get treatment.
Moreover, many of these devices incorporate feedback mechanisms and ergonomic features that ensure comfort and safety, which is crucial for widespread acceptance. Interestingly, studies show that device-assisted injections can reduce pain perception by up to 60%, significantly improving patient compliance (source).
But there’s a question of whether they’re truly worth the investment. Are they just a passing trend, or do they genuinely improve outcomes? Well, that’s what we’ll explore next as we delve into how these smart injectors are reshaping patient care, one painless shot at a time.
Assess Patient Anxiety and Prepare Equipment
Begin by evaluating the patient’s level of needle anxiety through a brief discussion. Select the appropriate smart needle injector device based on clinical needs. Ensure the device is fully charged, sterilized, and ready for use, similar to preparing a high-precision instrument before surgery.
Position the Patient for Comfort
Position the patient in a comfortable and relaxed posture, akin to settling in a recliner before a massage. Proper positioning reduces anxiety and makes needle insertion smoother. Use calming language to reassure them, setting a trustful environment.
Calibrate the Device and Confirm Settings
Power on the smart injector and calibrate it according to the manufacturer’s instructions. Many devices incorporate feedback mechanisms to tailor the injection’s speed and pressure, akin to tuning a musical instrument for perfect harmony. Verify settings align with the treatment protocol and patient-specific considerations.
Apply Topical Anesthetic if Needed
If the patient has high sensitivity, apply a topical anesthetic to numb the injection site. This step complements the device’s gentle operation and can significantly reduce discomfort, much like coating a rough surface with a smooth primer before painting.
Perform the Injection with Precision
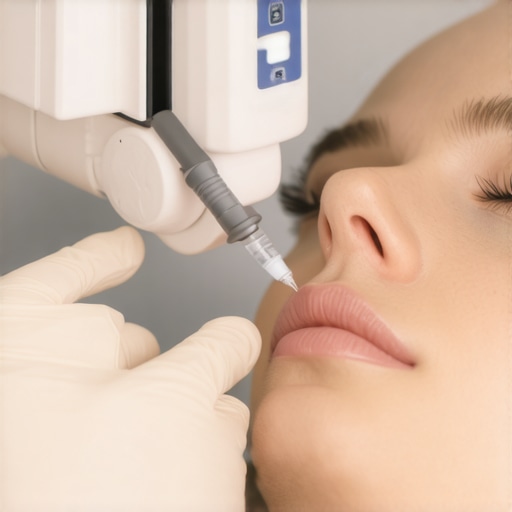
Align the device perpendicular to the injection site, stabilizing with one hand while gently pressing the device against the skin. Activate the injector with a firm, steady press, observing the controlled pulsed delivery that minimizes pain and anxiety. This process is comparable to firing a precision laser—controlled, focused, and clean.
Monitor and Reassure the Patient
While the device performs the injection, watch for signs of discomfort. Verbally reassure the patient, much like a pilot maintaining communication during a smooth flight. If necessary, pause and assess, adjusting the approach for future injections.
Post-Injection Care and Feedback
After completion, hold pressure on the site if bleeding occurs. Engage the patient in feedback about their comfort level. Document the procedure details, including device settings and patient response, similar to logging data in a flight recorder—valuable for refining future practices. Incorporate patient feedback to improve your technique and device familiarity, ensuring each injection becomes faster and less stressful.
By following these steps, medical practitioners can seamlessly integrate smart injectors into their practice, significantly reducing fear and pain associated with injections. Consistent application of this method ensures better patient compliance and a more humane approach to essential medical procedures.
Leverage Technology to Transform Care
Remember, successful implementation depends on thorough preparation, patient communication, and precise execution—like assembling a complex medical device with multiple interconnected parts working in harmony. As technology advances, embracing these new tools transforms healthcare experiences from daunting to comforting.
Many healthcare professionals and patients alike operate under the assumption that all medical devices are infallible and designed perfectly. However, this belief often blinds us to critical nuances that can lead to costly mistakes. For instance, common misconceptions such as equating high-tech features with absolute reliability overlook the subtleties of device implementation and environment-specific performance. In my experience, a device that performs flawlessly in one setting might underperform or even pose hazards in another due to overlooked factors like calibration drift or user misuse.
One pervasive myth is that of ‘one-size-fits-all’ equipment. This oversimplification ignores the fact that, for example, wireless detectors designed for urban hospitals may not be suitable for rural clinics with limited infrastructure. Using unsuitable equipment can compromise image quality or data security, leading to misdiagnosis or data breaches. Moreover, many assume that maintenance and calibration are straightforward, but neglecting these steps can cause devices like ultrasonic scalers or lab analyzers to produce inaccurate results, which can be deadly in critical care situations.
Are We Overlooking the Impact of Software on Medical Device Safety?
Advanced medical equipment now heavily relies on complex software algorithms. Yet, users often underestimate the significance of software validation, updates, and cybersecurity. A flaw in the software logic of devices such as sonic scalers or infusion pumps can lead to over- or under-dosing, with severe patient consequences. According to the FDA, software-related issues account for a significant percentage of device recalls annually, emphasizing the need for ongoing vigilance and expert understanding in software validation processes.
Furthermore, many practitioners are unaware of the importance of integrating devices into hospital information systems properly. Improper integration can result in data loss or corruption, especially when devices like lab incubators or portable diagnostics are involved. Consider the example of smart incubators that sync with lab software; without correct configuration, the data exchanged may be inaccurate, leading to faulty diagnoses or treatments.
Another overlooked nuance is environmental factors affecting device performance. Dust, humidity, electromagnetic interference, and temperature fluctuations can degrade device accuracy over time. For example, portable ultrasound machines designed for emergency use require strict environmental controls to ensure image clarity. Failing to account for these conditions invites errors—often unnoticed until they cause adverse outcomes.
In conclusion, it’s crucial to approach medical devices with a critical eye that goes beyond surface-level features. Every piece of equipment carries hidden dependencies — software integrity, environmental suitability, user training, and maintenance practices — which significantly influence patient safety and care quality. Recognizing these nuances helps avoid pitfalls that could compromise outcomes and instead fosters truly reliable healthcare delivery. Have you ever fallen into this trap? Let me know in the comments.
Tools I Recommend for Reliable Medical Equipment Operation
Ensuring medical devices remain operational and precise over time is vital for patient safety and treatment efficacy. In my practice, I rely heavily on high-quality calibration tools like the ergonomic pipette stands. These stands not only prevent damage but also promote proper handling, reducing calibration drift. Additionally, I recommend investing in comprehensive cleaning kits such as the best cleaning kits for lab equipment to maintain hygiene and prevent malfunctions caused by contamination. Regular maintenance schedules, including routine software updates, are equally important, especially for devices dependent on complex algorithms, like sonic scalers.
For example, I personally calibrate our wireless x-ray detectors weekly using manufacturer-recommended software diagnostic tools, ensuring data accuracy and compliance. I also keep spare parts, such as filters and batteries, on hand for rapid replacements, minimizing downtime. Implementing a digital log of maintenance activities helps track device performance and schedules timely interventions.
How do I maintain medical devices over time?
To keep equipment functioning smoothly, establish a preventative maintenance plan that includes scheduled calibrations, routine cleaning, and software reviews. Modern tools like ultrasound scalers benefit greatly from digital diagnostics that alert users to potential issues before failure occurs, ultimately saving costs and safeguarding patient care. Make sure to incorporate external expert advice, such as the detailed calibration procedures outlined by ISO standards, ensuring compliance and accuracy. Don’t wait for equipment to fail—regular proactive checks are your best line of defense. Why not try integrating a weekly calibration routine with advanced diagnostic tools to extend your device’s lifespan significantly? As technology advances, I predict increased use of AI-powered maintenance software that can predict failures before they happen, transforming the future of healthcare equipment reliability.
Lessons I Didn’t Expect to Learn from Medical Devices
- One of the most profound realizations came from understanding that even the most advanced device requires human oversight and continuous learning. Relying solely on technology without understanding its limitations can be dangerous, especially when environmental factors aren’t accounted for.
- Another insight was the importance of user training. No matter how sophisticated a device is, improper operation can lead to errors, sometimes with severe consequences. This made me prioritize comprehensive onboard training and regular updates.
- I also discovered that software validation isn’t a one-time task but an ongoing process. Staying up-to-date with cybersecurity measures and firmware updates is essential for patient safety and data integrity.
- Lastly, I learned that environmental factors such as humidity, dust, and electromagnetic interference significantly impact device performance. A proactive approach to environmental controls and regular calibration can prevent many issues before they arise.
My Go-To Resources for Reliable Medical Equipment Insights
- Medical Device Insights Blog: An invaluable source for the latest trends and in-depth analyses of emerging technologies. I trust it because of its thorough research and balanced perspectives.
- ISO Standards Documentation: For calibration, maintenance, and quality assurance, adhering to ISO guidelines ensures safety and consistency across all devices.
- Manufacturer’s Technical Manuals: They provide specific troubleshooting tips and operational details that are critical for proper device handling.
- Cybersecurity Best Practices: Resources like NIST guidelines help me protect patient data and maintain device software integrity.
Your Journey Toward Smarter Healthcare Starts Today
Embracing these lessons and resources can elevate your approach to medical devices, ensuring safer and more effective patient care. The future belongs to those who stay informed, vigilant, and proactive in adapting to technological advancements. Remember, the path to excellence in healthcare is continuous — keep learning, experimenting, and improving.
What’s been your biggest challenge with medical equipment, and how did you overcome it? Share your story below — your experience might inspire others to take their practice to the next level.
,

