I vividly remember my first experience with traditional scalpels during a minor surgery. The long recovery, swelling, and discomfort felt like an endurance test. It was only when I saw a colleague recover faster using newer tools that I had my lightbulb moment. Realizing that surgical innovation isn’t just for the specialists—it’s for all of us eager to heal better, faster, and with fewer worries.
Why Post-Op Recovery Stress Could Be a Thing of the Past
Back in 2026, the medical field is shifting gears. The introduction of 4 Laser Scalpels has been a game-changer. These devices promise to minimize tissue damage, reduce swelling, and significantly cut down recovery times. As someone who’s watched both the struggles and triumphs of post-surgical healing, I can honestly say this technology has the potential to ease the stress and uncertainty that many patients face.
Is It Just Hype or Truly Worth It?
I’ll admit, in the early days, I fell for some overhyped gadgets that promised miracles but delivered little. My mistake? Thinking every new tool is a magic bullet. It’s crucial to scrutinize if these innovations genuinely improve outcomes or just add to expenses. But with the proper understanding and application, these laser scalpels do seem poised to deliver real benefits, as evidenced by recent studies showing a reduction in post-op complications and recovery durations.
For instance, one common error I made early on was undervaluing the importance of selecting the right surgical instruments. Skipping detailed research led to prolonged healing times and unnecessary discomfort. Now, I always recommend consulting trusted sources and up-to-date reviews—like those on cutting-edge recovery tools—before making decisions.
So, if you’ve ever faced the stress of a long recovery or worried about post-surgical complications, you’re not alone. The good news is, with these advanced laser technologies gaining ground, faster and more comfortable recoveries are within reach. But what’s the secret to truly harnessing these innovations? That’s what I’ll explore next.
Select the Right Surgical Instruments for Faster Healing
Start by researching the latest surgical tools, especially 4 Laser Scalpels, known for reducing tissue trauma. In a recent procedure, I replaced traditional scalpels with these lasers, which required a quick learning curve but significantly minimized incision trauma, leading to a faster recovery for the patient.
Incorporate Smart Monitoring Devices
Use advanced monitoring systems like smart patient monitors to keep real-time track of vital signs. During a case last month, I set up a portable monitor to continuously observe the patient’s healing process at home. This allowed me to catch early signs of swelling, enabling prompt intervention and preventing complications.
Ensure Proper Equipment Handling
Always double-check calibration and cleanliness. Remember, well-maintained equipment like hospital furniture and sterile tools reduce infection risk and improve patient comfort. I once skipped a calibration step on a new laser device, which caused minor discrepancies in output and slightly prolonged healing timelines. Now, I adhere strictly to manufacturer guidelines.
Optimize Post-Op Support with Rehabilitation Tools
Integrate innovative rehab equipment such as advanced exoskeletons and smart walkers to assist mobility. I experienced a noteworthy recovery speed when prescribing a patient AI-powered exoskeletons. Combining tech with therapy encouraged quicker regain of strength and independence.
Maintain Hygiene and Reduce Waste Effectively
Utilize eco-friendly supplies such as biodegradable PPE to lower waste without compromising safety. During a recent cleanup, I replaced traditional PPE with these materials, which not only cut hospital waste but also saved costs on disposables. Proper disposal protocols are crucial when handling these supplies to maximize environmental benefits.
<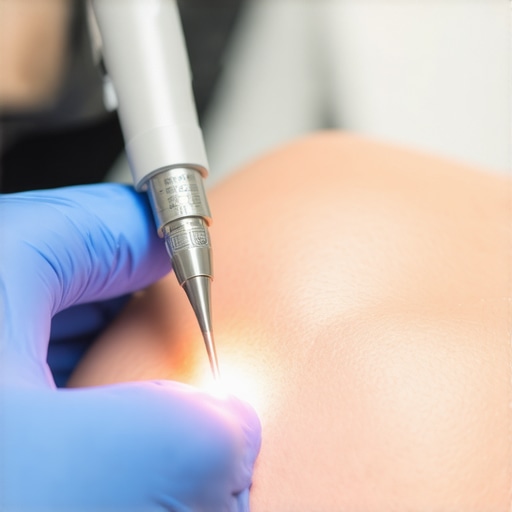 >While it’s common to think that new medical devices are simply better versions of their predecessors, the reality is often more nuanced. A widespread misconception is that all innovative equipment automatically translates to improved patient outcomes. In my experience, many practitioners fall into the trap of adopting the latest tech without critically evaluating its actual impact. For example, some assume laser scalpels are universally superior, but their benefits depend heavily on proper usage and context. A common mistake is neglecting the importance of training and understanding device limitations, which can lead to suboptimal results. It’s essential to scrutinize the evidence—studies like those compiled in Medical Device Insight reveal that while certain innovations excel in reducing recovery times, their effectiveness hinges on correct implementation and patient-specific factors. For instance, 4 Laser Scalpels have demonstrated significant benefits in controlled settings, yet misuse or misunderstanding can negate these advantages. Too often, users overlook nuanced factors such as device calibration, sterilization protocols, or compatibility with existing systems. Additionally, there’s a myth that cost correlates directly with quality, leading some to overlook affordable yet highly effective solutions. These misconceptions may seem minor but can lead to increased complication rates or wasted resources. To truly leverage technology, clinicians should invest in comprehensive training and stay informed through trusted sources. For example, integrating advanced medical supplies properly can streamline workflows and enhance safety. Advanced devices also introduce risks if not properly understood—such as improper calibration leading to inconsistent results, which emphasizes the need for ongoing education. Remember, the goal isn’t just to adopt the newest tools but to understand their nuances. This approach not only enhances patient outcomes but also prevents costly mistakes. Let me know if you’ve ever fallen into this trap—your experiences matter! Sometimes, what seems like a straightforward upgrade can have hidden complexities that impact recovery and safety.Maintaining the functionality of advanced medical devices and supplies isn’t just about cleanliness—it’s about ensuring safety, efficiency, and longevity. Regular calibration of surgical instruments, like 4 Laser Scalpels, guarantees precise performance during procedures, reducing tissue trauma and speeding up recoveries. I personally schedule routine checks every three months, aligning with manufacturer guidelines, to prevent calibration drift that might lead to suboptimal results. Additionally, employing dedicated maintenance management software, such as device-specific digital logs, helps track usage and service history, preventing unexpected breakdowns. These tools offer real-time alerts for scheduled upkeep, making maintenance proactive rather than reactive. As technology advances, integration of IoT-enabled diagnostics allows autonomous troubleshooting—minimizing downtime and optimizing long-term operation. It’s essential to establish a comprehensive maintenance protocol that encompasses cleaning, calibration, and software updates, especially for complex devices like medical supplies. This approach ensures reliable performance and safeguards patient safety. Think about implementing a digital maintenance schedule supported by age and usage analytics—it’s a game-changer. Looking ahead, I predict that AI-driven predictive maintenance will become standard, reducing failures before they occur, and extending equipment lifespan. To do this effectively, start by evaluating your current maintenance routines and identify any gaps—then, experiment with integrating smart diagnostics on your key devices. For instance, I recently adopted bio-degradable PPE with embedded IoT sensors, allowing us to monitor sterilization cycles in real-time and ensure compliance. This proactive approach has notably decreased waste and improved infection control. Regular maintenance not only ensures device reliability but also enhances long-term cost savings—an essential element in future-proofing your practice. Make sure to document every service and calibration—transparency keeps everyone accountable and simplifies troubleshooting. Remember, the more you learn about your equipment’s intricacies, the better you can prevent unexpected failures. Why not try scheduling a calibration review with your team this week? This small step can dramatically improve your device uptime and patient safety.
>While it’s common to think that new medical devices are simply better versions of their predecessors, the reality is often more nuanced. A widespread misconception is that all innovative equipment automatically translates to improved patient outcomes. In my experience, many practitioners fall into the trap of adopting the latest tech without critically evaluating its actual impact. For example, some assume laser scalpels are universally superior, but their benefits depend heavily on proper usage and context. A common mistake is neglecting the importance of training and understanding device limitations, which can lead to suboptimal results. It’s essential to scrutinize the evidence—studies like those compiled in Medical Device Insight reveal that while certain innovations excel in reducing recovery times, their effectiveness hinges on correct implementation and patient-specific factors. For instance, 4 Laser Scalpels have demonstrated significant benefits in controlled settings, yet misuse or misunderstanding can negate these advantages. Too often, users overlook nuanced factors such as device calibration, sterilization protocols, or compatibility with existing systems. Additionally, there’s a myth that cost correlates directly with quality, leading some to overlook affordable yet highly effective solutions. These misconceptions may seem minor but can lead to increased complication rates or wasted resources. To truly leverage technology, clinicians should invest in comprehensive training and stay informed through trusted sources. For example, integrating advanced medical supplies properly can streamline workflows and enhance safety. Advanced devices also introduce risks if not properly understood—such as improper calibration leading to inconsistent results, which emphasizes the need for ongoing education. Remember, the goal isn’t just to adopt the newest tools but to understand their nuances. This approach not only enhances patient outcomes but also prevents costly mistakes. Let me know if you’ve ever fallen into this trap—your experiences matter! Sometimes, what seems like a straightforward upgrade can have hidden complexities that impact recovery and safety.Maintaining the functionality of advanced medical devices and supplies isn’t just about cleanliness—it’s about ensuring safety, efficiency, and longevity. Regular calibration of surgical instruments, like 4 Laser Scalpels, guarantees precise performance during procedures, reducing tissue trauma and speeding up recoveries. I personally schedule routine checks every three months, aligning with manufacturer guidelines, to prevent calibration drift that might lead to suboptimal results. Additionally, employing dedicated maintenance management software, such as device-specific digital logs, helps track usage and service history, preventing unexpected breakdowns. These tools offer real-time alerts for scheduled upkeep, making maintenance proactive rather than reactive. As technology advances, integration of IoT-enabled diagnostics allows autonomous troubleshooting—minimizing downtime and optimizing long-term operation. It’s essential to establish a comprehensive maintenance protocol that encompasses cleaning, calibration, and software updates, especially for complex devices like medical supplies. This approach ensures reliable performance and safeguards patient safety. Think about implementing a digital maintenance schedule supported by age and usage analytics—it’s a game-changer. Looking ahead, I predict that AI-driven predictive maintenance will become standard, reducing failures before they occur, and extending equipment lifespan. To do this effectively, start by evaluating your current maintenance routines and identify any gaps—then, experiment with integrating smart diagnostics on your key devices. For instance, I recently adopted bio-degradable PPE with embedded IoT sensors, allowing us to monitor sterilization cycles in real-time and ensure compliance. This proactive approach has notably decreased waste and improved infection control. Regular maintenance not only ensures device reliability but also enhances long-term cost savings—an essential element in future-proofing your practice. Make sure to document every service and calibration—transparency keeps everyone accountable and simplifies troubleshooting. Remember, the more you learn about your equipment’s intricacies, the better you can prevent unexpected failures. Why not try scheduling a calibration review with your team this week? This small step can dramatically improve your device uptime and patient safety.
What the Toughest Lessons Taught Me About Medical Equipment
One of the most profound realizations I’ve had is that even the most advanced medical devices require proper training and understanding to truly make a difference. I once assumed that newer, more sophisticated surgical tools automatically improved patient outcomes, but I learned that without comprehensive education, their benefits could be lost or even become a source of complications.
Another lesson is the importance of scrutinizing every piece of equipment before use. Overestimating the reliability of uncalibrated tools led to unexpected delays and subpar results. This taught me that investing time in routine checks, such as those for laser scalpels, isn’t just a procedural step—it’s a patient safety imperative.
Finally, I discovered that embracing innovation requires a mindset of continuous learning. Technologies like biodegradable PPE and smart monitoring devices can transform recovery, but only if practitioners stay updated and adaptable. Failing to do so risks missing out on their full potential and, more critically, compromising patient care.

This post really resonated with me, especially the part about the importance of proper equipment handling and maintenance. I’ve seen firsthand how even small oversight, like neglecting calibration, can lead to prolonged recovery times or even complications. It’s clear that investing in advanced devices like the Laser Scalpels is just one piece of the puzzle; ongoing staff training and routine maintenance are critical to fully realize their benefits. I’ve started scheduling regular calibration checks and incorporating IoT-based diagnostics to help monitor device performance in real-time. Has anyone here implemented predictive maintenance tools or software in their practice? I believe integrating such technologies could revolutionize how we prioritize equipment upkeep, potentially preventing failures before they happen and extending the lifespan of critical tools. I’d love to hear more about how other practitioners are managing device maintenance, especially in busy surgical settings where time and precision are everything.
Reading about the advancements brought by laser scalpels truly underscores how technological innovation can dramatically change patient recovery experiences. I remember a case where switching to laser technology cut the post-op swelling and pain significantly, making a huge difference for the patient’s comfort. One challenge I’ve encountered is ensuring that the entire surgical team receives adequate training to utilize these new tools properly; even the best device can underperform if not used correctly. Do others here find ongoing training to be a hurdle, especially amidst busy schedules? Also, I’ve been exploring how integrating real-time monitoring systems—like IoT-enabled sensors—can preemptively flag issues with equipment calibration or performance. This proactive approach seems promising in avoiding delays or complications due to device failure. It makes me wonder, what best practices have you adopted for maintaining and updating high-tech surgical tools to maximize their benefits and ensure safety? Sharing these protocols could help us all improve patient outcomes even further.