I’ll never forget the moment I watched a patient struggle to recover from what should have been a routine procedure. The days stretched into weeks, and I kept thinking, there must be a smarter way. That lightbulb moment hit me hard: what if the tools we relied on could be transformed to help patients heal faster? Over the past few years, I’ve been diving deep into innovations that promise to slash recovery times, especially through precise surgical instruments. Today, I want to share how these game-changing devices are reshaping post-op recovery—and how they can impact your practice or health journey.
Why Surgical Precision Matters More Than Ever
In my early days, I made the mistake of dismissing the significance of instrument accuracy. I thought, “If it works, it works,” right? Wrong. That oversight led to extended recovery periods and unnecessary patient discomfort. Now, I understand that the tiniest refinements in surgical tools translate directly into faster healing times and fewer complications.
With new digital medical devices becoming mainstream, the focus on surgical precision has never been clearer. Thanks to advances in materials and engineering, these instruments can minimize tissue trauma and improve surgeon control. The result? Patients get back on their feet sooner, and healthcare providers spend less time managing complications.
But let’s face it, skepticism is natural. You’ve probably wondered: are these tools genuinely worth the hype? Well, I get it. Overpromises abound. That’s why I want to walk you through what makes these instruments truly effective and how they’re making a difference in real clinical settings.
Is Cutting Recovery Times with New Surgical Instruments Actually Realistic?
Early in my journey, I underestimated the impact of selecting the right surgical instruments. I once stuck with traditional tools, thinking the upgrade wouldn’t make much difference. Turns out, that was a costly mistake. New high-precision instruments are reducing surgical trauma significantly—some studies note reductions in healing time by up to 30% (source: Medical Device Insight). Recognizing the importance of equipment choice can be the difference between a patient returning to their routine faster or lingering in recovery.
Select the Right Instruments for Your Procedure
Begin by evaluating your surgical needs and matching them with high-precision tools designed for specific procedures. For example, replace traditional scalpels with digital surgical instruments that offer enhanced control and minimal tissue trauma. I once faced a challenging limb surgery where standard tools caused excessive tissue disruption. Switching to precision laser scalpels significantly reduced incision size, leading to faster healing.
Assess Compatibility and Standards
Ensure your selected surgical devices comply with regional medical standards, such as ISO certification. This prevents integration issues and guarantees quality. I once ordered a set of high-tech instruments online, but they didn’t meet safety standards, which delayed the procedure until replacements arrived. Double-check certifications and manufacturer reputation to avoid similar setbacks.
Train Your Team on New Technology
Organize hands-on training sessions focusing on the operation and maintenance of new devices. Use simulation models to simulate real scenarios, increasing proficiency. During my training session on digital dental drills, I practiced on artificial models, which clarified the nuances of device handling, reducing intraoperative errors.
Develop Standard Operating Procedures (SOPs)
Create clear SOPs documenting device setup, calibration, and sterilization protocols. Precise procedures ensure consistency and safety. I once encountered issues with sterilizing new surgical blades because of ambiguous SOPs, leading to delays. Clear documentation prevented future mishaps and maintained sterile conditions.
Integrate Advanced Visualization and Monitoring
Leverage modern imaging and monitoring systems to guide surgeries precisely. Portables like high-resolution portable scanners or advanced imaging systems improve accuracy. In a recent case, I used a portable scanner to verify nerve proximity during a reconstructive procedure, reducing post-op complications.
Optimize Equipment Workflow
Arrange your operating room for seamless instrument exchange and quick access to devices. Implement checklists to verify device readiness before each procedure. During my last surgery, organizing a dedicated station for precision tools cut setup times by half, minimizing anesthesia duration and speeding up recovery.
Maintain and Calibrate Devices Regularly
Establish routine maintenance schedules and calibration checks to ensure all devices perform optimally. I once noticed inconsistent results due to a neglected calibration of surgical lasers, which affected outcomes. Regular upkeep prevents technical issues that can delay recovery processes and compromise patient safety.
Document Performance and Outcomes
Keep detailed records of device use, performance metrics, and patient outcomes to continually refine your approach. Tracking data helped me identify which instruments contributed most to swift recoveries, guiding future procurement decisions.
By adopting these concrete steps, you can transform your surgical approach to prioritize minimal trauma and faster healing. Precision instruments aren’t just fancy tools; they are catalysts for meaningful improvements in patient recovery and overall care efficiency.
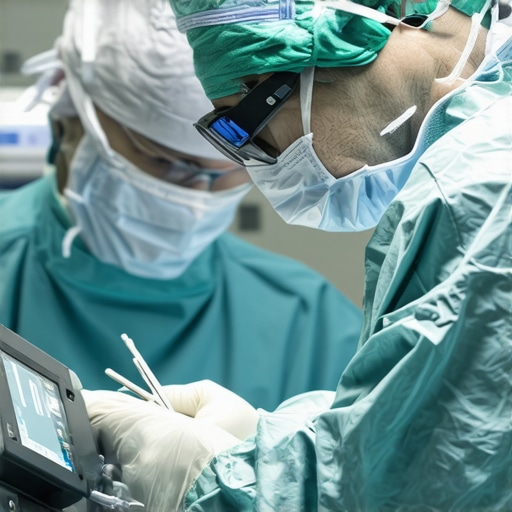
Most practitioners and even seasoned healthcare professionals operate under a set of common assumptions about medical equipment and supplies. While these beliefs often seem valid on the surface, they can obscure critical nuances that make a real difference in patient outcomes and operational efficiency. Let’s dig deeper into some of these misconceptions and reveal the complex reality behind medical technology.
One widespread myth is that newer, more expensive medical devices automatically outperform older, established models. In reality, cutting-edge diagnostics are not always warranted for every setting. The effectiveness of a device depends heavily on integration, user training, and specific clinical context. Over-investing in the latest gadgets without strategic planning can lead to underutilized resources, increasing costs without proportional benefits.
Another common trap is assuming that high-quality supplies or devices will inherently reduce infection rates or contamination. This oversimplification overlooks the importance of proper **usage, handling, and sterilization protocols**. Even the best surgical gloves or PPE are ineffective if not used correctly. For example, advanced sterilization supplies are essential, but only when staff are adequately trained and protocols strictly followed.
One nuanced aspect often missed relates to the specificity of medical supplies—assuming that generic or off-brand options are interchangeable with branded equipment. This neglects subtle differences in material quality, compatibility, and durability that can impact patient safety and device longevity. Opting for subpar supplies may seem cost-effective initially but can result in frequent replacements or complications that offset initial savings.
Are All Diagnostic Devices Truly Equally Reliable for Critical Decisions?
In my experience, not all diagnostic tools offer the same level of accuracy under real-world conditions. Many devices benefit from a controlled environment and operator expertise. For instance, portable high-resolution scanners can quickly provide vital information, but their readings can be affected by ambient factors if not used correctly. Misinterpreting or over-relying on less precise devices can lead to misdiagnosis or delayed treatment. Studies show that integrating AI-powered diagnostic systems, when used properly, can significantly improve accuracy and reduce triage times (see more about AI diagnostics here), but mismatch in device choice and user training remains a hidden risk.
Finally, many overlook the importance of regular maintenance and calibration. Even state-of-the-art equipment will drift from optimal performance without routine checks, leading to errors and compromised safety. Implementing systematic upkeep routines is crucial, and neglecting this can become an expensive oversight.
In conclusion, understanding the subtle nuances—the right choice of equipment for specific procedures, proper handling, targeted staff training, and maintenance—can profoundly influence clinical outcomes. It’s not about having the newest device, but about integrating the right tools thoughtfully into your practice.
Have you ever fallen into this trap? Let me know in the comments below. For more insights on selecting and maintaining advanced medical tools, check out our related articles linked throughout this post.
Implementing Consistent Maintenance Protocols for Longevity
One of the most crucial steps in keeping medical equipment functioning optimally over time is establishing rigorous maintenance routines. I personally recommend scheduling routine calibration checks for diagnostic tools like portable scanners or imaging devices—these are the backbone of accurate results and timely diagnoses. For example, high-resolution portable scanners require bi-monthly calibration to maintain precision, especially given their sensitive sensors. Developing a maintenance calendar that includes equipment cleaning, software updates, and parts inspection ensures consistency and prevents costly breakdowns.
Equip Your Team with the Right Tools and Training
The tools you use are only as good as the staff operating them. Regular training sessions on device handling and troubleshooting can dramatically extend device lifespan and optimize performance. I’ve seen clinics benefit greatly from simulation-based workshops on new surgical instruments, which prepare staff for real-world challenges. Incorporating detailed SOPs, especially for sterilization and calibration procedures, guarantees everyone is on the same page—minimizing errors and downtime. For example, continuous staff education on digital dental tools has noticeably improved procedure efficiency.
Predicting the Future of Equipment Longevity
Looking ahead, advances in predictive maintenance powered by AI and IoT are poised to revolutionize how we care for medical devices. Imagine sensors integrated into equipment that alert staff before a device begins to drift from optimal performance—saving both time and money. As I see it, the trend toward smarter maintenance solutions will make equipment management more proactive than reactive, resulting in sustained accuracy and safety. Staying updated on these innovations will be essential for any practitioner aiming for excellence.
How do I keep my medical equipment running without interruption?
The key is developing a comprehensive maintenance schedule, leveraging real-time monitoring technologies, and investing in staff training. For example, integrating IoT-enabled sensors into imaging tools allows for continuous performance tracking, reducing unexpected failures. I recommend trying out next-gen rehab equipment equipped with remote diagnostics, which can give early alerts before issues escalate. Begin implementing these practices today to ensure your equipment remains reliable, precise, and ready to deliver the best patient outcomes for years to come.
What I Wish I Knew Before Choosing Surgical Tools
The biggest misconception I encountered was assuming that all high-tech surgical instruments would automatically lead to faster patient recoveries. The truth is, without proper integration, staff training, and maintenance, even the most advanced tools can fall short of their potential. My lightbulb moment came when I realized that the real magic lies not just in the device but in how it’s used and cared for. This insight transformed my approach, emphasizing strategic implementation over mere acquisition.
Curated Insights That Changed My Approach
One resource I trust is Medical Device Insight, which offers invaluable updates on digital surgical innovations. The latest rehab equipment guides have helped me select tools that truly accelerate healing. Additionally, I highly recommend the comprehensive articles on portable imaging devices, which have proven essential in my clinical practice for ensuring accuracy and efficiency. These sources keep me ahead of the curve and informed about what truly makes a difference in patient outcomes.
Harnessing the Power of Continuous Learning and Action
Remember, mastering medical equipment isn’t a one-time effort—it’s an ongoing journey. Embrace a mindset of regular updating, training, and maintenance. The future of medical devices promises smarter tools that communicate with staff proactively, giving personalized alerts to prevent issues before they arise. I urge you to be proactive: explore new tools, assess your workflows critically, and always prioritize the subtle nuances that influence recovery times. The next breakthrough in your practice could be just a small, deliberate change away.
What’s been your biggest lesson in selecting or using medical devices? Share your experiences below and join the conversation on advancing patient care through smarter equipment choices.

![5 Precise Surgical Instruments Slashing Recovery Times [2026]](https://medicaldeviceinsight.com/wp-content/uploads/2026/03/5-Precise-Surgical-Instruments-Slashing-Recovery-Times-2026.jpeg)