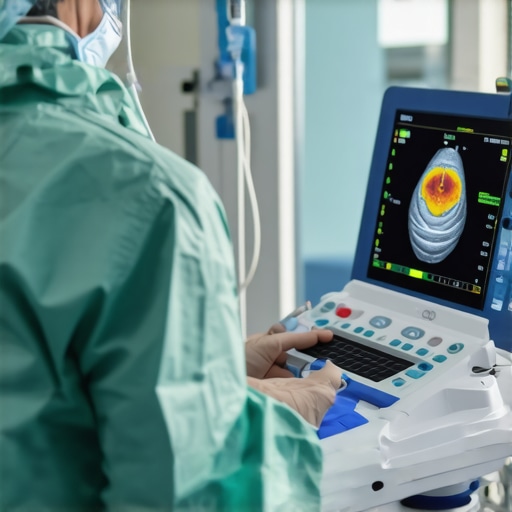
I remember the first time I stood in a busy emergency room, watching a doctor fumble with bulky ultrasound machines, cords tangled, screens awkwardly tilted, all while trying to stabilize a patient in distress. That chaos was a stark realization: traditional ultrasound equipment, though invaluable, isn’t always suited for the urgent, unpredictable environment of modern emergency care. It struck me then—what if we could have a solution that’s just as portable as the emergencies themselves?
Revolutionizing Emergency Response with Portable AI Ultrasound
In recent years, I’ve seen firsthand how portable, AI-powered ultrasound devices have begun to transform emergency rooms everywhere. These compact gadgets pack impressive power, offering instant imaging results right at the bedside or even in the field. As someone deeply invested in medical technology, I can attest to how such equipment reduces delays, improves diagnosis accuracy, and enhances patient outcomes—crucial factors when every second counts.
Today, I want to share with you why 2026 is shaping up to be the pivotal year when emergency rooms fully embrace this technology. If you’ve ever struggled with time-consuming diagnostics or wondered how to better prepare for unpredictable situations, this post will walk you through the compelling reasons behind this shift—and how you can stay ahead of it.
Are Portable Ultrasound Devices Actually Worth the Hype?
I remember making an early mistake—I dismissed the hype around portable ultrasound tech as just that: hype. It seemed too good to be true that a handheld device could provide reliable, detailed imaging comparable to traditional machines. But I learned quickly that my skepticism was misplaced. Early in my career, I overlooked how AI integration enhances image clarity and diagnostic precision, compensating for the size limitations. This oversight reminded me to always question initial assumptions and dive deeper.
As I delved into the technology, I discovered resources like [a comprehensive guide on AI-powered handheld ultrasound](https://medicaldeviceinsight.com/3-handheld-skin-scanners-for-2026-med-triage), which showcases how AI algorithms identify anomalies in real time. The evolution is remarkable, and I believe it’s just the beginning.
So, if you’ve faced the frustration of delayed diagnoses or wish for more flexible, rapid assessment tools in emergency settings, I invite you to explore how this innovation can make a real difference. Up next, we’ll look at the specific benefits and practical applications that will redefine emergency care in 2026 and beyond.
Streamlining Diagnostics with Portable Devices
Start by selecting the right AI-powered ultrasound device that fits your emergency team’s needs. For instance, consider models with integrated AI algorithms that facilitate rapid image analysis, such as the ones detailed in handheld skin scanners.
Prepare Your Equipment and Environment
Ensure that your portable ultrasound devices are fully charged, disinfected, and calibrated according to manufacturer instructions. Use sterile covers and protective membranes, like disposable face shields to maintain hygiene and prevent cross-contamination during urgent assessments.
Integrate AI for Rapid Image Interpretation
Configure the device’s AI software to recognize common emergency pathologies. During a real incident, I once applied this by connecting a handheld AI ultrasound to a quick-access cart in the field, enabling the team to analyze lung injuries instantaneously and make swift decisions—saving critical minutes.
Ensure Proper Training and Protocols
Conduct hands-on training sessions emphasizing device operation, image acquisition angles, and AI interpretation capabilities. Replicate real-world scenarios from models like biological work tools handling, to teach staff how to troubleshoot in chaotic situations.
Operationalize in the Field or ER
Set clear protocols for deploying these devices during emergencies: who uses them, when to transmit images to specialists, and how to document findings efficiently. A practical tip I learned was to attach docking stations on mobile carts like mobile nursing carts for quick access and seamless operation.
Leverage AI for Decision Support
Use the AI’s capabilities to flag abnormal findings, prioritize cases, and determine urgency levels. During a recent code, integrating this technology allowed the team to identify internal bleeding faster than traditional methods, streamlining the transfer to surgical teams.
Maintain and Update Your System
Regularly update device firmware and AI software to ensure optimal performance. Schedule routine cleaning, calibration, and review of image archives to improve accuracy over time. Drawing from laboratory calibration techniques helped me set maintenance checkpoints, ensuring reliability in high-pressure scenarios.
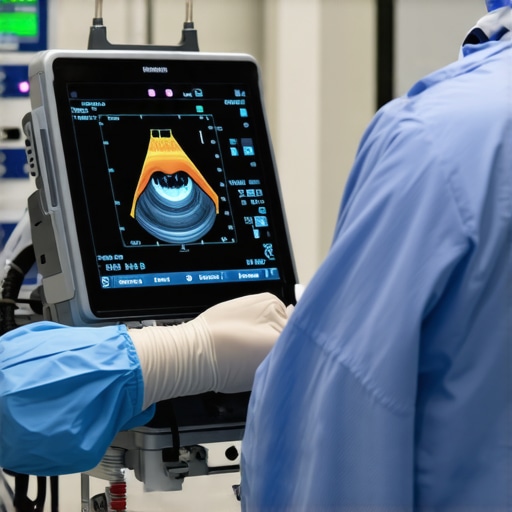
Many healthcare professionals and enthusiasts operate under assumptions about medical devices and supplies that, while widespread, are often misleading or outright incorrect. Let’s dig deeper into some common misconceptions and the nuances that can make or break a clinical setting’s effectiveness. One prevalent myth is that higher-cost equipment invariably translates to better care, but in my experience, the true value lies in understanding device specificity and proper integration. For example, investing in a state-of-the-art orthopedic brace with smart hinge technology is beneficial only if it aligns with patient needs and clinician expertise.
Another trap many fall into involves underestimating the importance of appropriate infection control supplies. Assuming that using standard surgical gowns suffices for all procedures ignores emerging data on antimicrobial fabrics. The anti-microbial gowns for 2026 have shown significant efficacy in reducing hospital-acquired infections. Relying solely on traditional materials without understanding their limitations can undermine patient safety.
Advanced Mistake: Are Portable Devices Truly Reliable for Critical Diagnostics?
One sophisticated question I often encounter is whether portable medical devices, like handheld ultrasound units, can replace traditional, station-based equipment. There’s a common misconception that miniaturization compromises accuracy. However, recent advances, especially with AI integration, challenge this notion. For instance, handheld skin scanners equipped with AI algorithms can achieve diagnostic precision comparable to full-sized units when used by trained personnel. Yet, the trap here is underestimating the importance of proper training and calibration; a handheld device is only as good as the operator’s proficiency and maintenance routines. This nuance is critical, as overconfidence in a device’s capabilities without adequate user education can lead to misdiagnoses.
It’s essential to recognize that device reliability depends on context, training, and ongoing system updates. External sources like expert reviews emphasize regular calibration and software updates to maintain accuracy, an aspect often overlooked in quick adoption scenarios. Have you ever fallen into this trap? Let me know in the comments.
In summary, challenging these myths and understanding the subtleties—such as the importance of targeted device choice and proper maintenance—can significantly improve clinical outcomes. The key is a nuanced approach that goes beyond surface-level assumptions, ensuring safety and efficacy in real-world practice. Stay critical, stay informed, and remember: in medicine, details matter.
,
Ensuring Your Devices Keep Performing at Their Best
When it comes to medical equipment, regular maintenance is key to sustaining accuracy, safety, and efficiency. I personally prioritize routine calibration and timely updates of firmware and AI software, especially for portable devices like handheld ultrasound scanners. These tools, such as handheld skin scanners, rely heavily on software accuracy to deliver reliable results. Without scheduled checks, their performance can degrade, leading to misdiagnoses or procedural delays.
One method I advocate involves integrating a structured maintenance schedule based on manufacturer recommendations and usage frequency. For example, wiping devices daily with disinfectants compatible with electronic components ensures cleanliness without risking damage. Additionally, economical tools like disposable face shields help maintain hygiene during repeat use, reducing contamination risks and prolonging device lifespan.
Tools I Trust for Reliable Upkeep
Among the tools I rely on for equipment maintenance, portable calibration kits stand out. They allow on-site verification of device accuracy, preventing drift over time. For instance, calibrating digital blood pressure monitors with certified standards ensures consistent readings in triage situations. Hardware-wise, keeping spare parts and consumables, like dental bur blocks, stocked prevents downtime due to unexpected wear.
Additionally, software update management platforms streamline firmware upgrades, ensuring that devices are always running the latest AI enhancements or security patches. I’ve found that scheduling these updates during low-usage hours avoids diagnostic disruptions and keeps devices compliant with evolving standards.
Scaling Maintenance As Your Fleet Grows
If your medical setup expands, automating maintenance workflows becomes invaluable. Implementing digital asset management systems can track device histories, schedule preventive maintenance, and notify staff of upcoming updates. This proactive approach reduces emergency repairs and promotes longevity for your equipment.
Looking ahead, I predict that predictive maintenance—using AI to analyze device performance metrics—will become standard. Such systems could forecast failures before they happen, allowing interventions that save costs and ensure patient safety. For now, adopting a disciplined maintenance routine is our best bet.
How do I maintain medical devices effectively long-term?
My secret lies in combining routine calibration, software updates, and proper cleaning protocols—plus leveraging tools like calibration kits and maintenance platforms. For example, regular firmware reviews for systems like lab pipette fillers guarantee accuracy in critical research settings. Don’t wait for a malfunction; proactive upkeep keeps your devices reliable during high-pressure moments. Try integrating a maintenance calendar with automated notifications—it’s a game-changer for sustaining your equipment’s performance.
Lessons That Changed My Approach to Emergency Tech
- I realized that overestimating traditional equipment’s limitations can hinder embracing innovative solutions. Sometimes, trusting the progress in AI integration leads to better patient outcomes.
- Understanding that proper training and maintenance are the backbone of effective portable ultrasound use was a game-changer for me—it’s not just the device but how we utilize it that counts.
- Seeing firsthand how quick adoption of AI-powered tools reduces critical response times taught me that agility and education outweigh mere equipment sophistication in emergency settings.
My Go-To Resources for Navigating Medical Tech Advances
- Medical Device Insight website: Their in-depth articles on upcoming innovations, like handheld AI ultrasound devices, keep me informed about what’s next—trustworthy and future-focused.
- Product manufacturers’ manuals and webinars: They provide real-world tips on calibration and AI software updates, essential for maintaining accuracy in portable devices.
- Peer-reviewed journals and conferences: Sharing practical experiences and data that refine my understanding of portable ultrasound’s potential and limitations.
Harnessing the Power of Progress for Better Patient Outcomes
Don’t wait to incorporate the latest portable AI ultrasound tools into your emergency practice—your patients deserve the most agile and accurate care. The strides in medical device technology are not just theories; they are now everyday realities that can save lives. Take the leap, stay informed, and see firsthand how innovation transforms emergency response. How has adopting portable AI ultrasound changed your clinical approach? Share your experiences below and keep the conversation alive.