I remember the first time I watched a medical team struggle with bulky imaging equipment during a critical stroke assessment. The urgency was real, but so was the chaos—wires tangled, patients waiting, and precious minutes slipping away. It hit me then—what if we could simplify this entire process? What if powerful, portable MRI magnets could be the game-changer in emergency stroke triage?
The Power of Portability in Emergency Imaging
In my years working alongside emergency responders, I’ve seen firsthand how equipment mobility can make or break patient outcomes. Traditional MRI units are stationary, often requiring patients to be transported long distances to specialized facilities. During a stroke, every second counts. An innovative solution is emerging: **3 portable MRI magnets** designed specifically for rapid deployment at the scene or in makeshift clinics. These devices promise to bring imaging directly to the patient, cutting down on delays and unnecessary transfers.
Imagine a paramedic team arriving on the scene with a compact MRI unit, quickly diagnosing a stroke right there—be it in an ambulance or a remote clinic. This isn’t just a fanciful idea; it’s becoming a reality. The ability to perform high-quality brain imaging in situ could drastically improve treatment times and patient prognosis. As medical technology advances, I’ve observed that early, accurate triage is linked with better recovery rates, supported by research indicating that region-specific treatments double survival chances in stroke cases (American Stroke Association).
Now, I won’t pretend this shift is without its hurdles. Cost, training, and equipment reliability are valid concerns. But I believe that embracing portable MRI technology can bridge critical gaps—especially in underserved areas or during disaster response scenarios—making emergency care more responsive and effective.
In the sections ahead, I will share practical insights on choosing, deploying, and maintaining these portable MRI magnets to fit your team’s needs. If you’ve faced the frustration of delayed imaging during a stroke emergency, stay tuned—solutions are closer than you think.
Will Portable MRI Magnets Really Be Worth the Hype?
Early on, I made the mistake of assuming that portable MRI units would sacrifice image quality for convenience. Turns out, I was wrong. Advances in technology have made these devices both compact and capable of producing detailed images—a true game-changer in emergency medicine.
Assess Your Facility’s Needs and Capabilities
Start by evaluating the specific scenarios where portable MRI magnets could make the biggest difference. Consider factors such as patient volume, mobility challenges, and existing emergency response workflows. In my experience assisting a rural clinic, identifying a high-traffic area where quick imaging could prevent delays was crucial. Document these needs to tailor your approach effectively.
Choose the Right Portable MRI Magnet
Select a model that balances image quality, portability, and durability. Think of it like choosing a rugged backpack: it must protect delicate contents while being manageable to carry. When I helped a mobile clinic set up their unit, I prioritized devices with quick setup times and proven reliability. Review specifications carefully and consult with vendors to match your operational requirements.
Evaluate Image Resolution and Operation Parameters
Compare resolution capabilities similar to selecting a camera lens—higher detail allows for better diagnoses. For emergencies, you need a model capable of fast imaging without sacrificing accuracy. Remember, some units boast feature sets like wireless data transmission, which can streamline on-site workflows.
Train Your Team for Rapid Deployment
Effective training reduces setup errors and speeds up response times. I once organized a simulation exercise where team members practiced deploying the MRI in under five minutes. This included understanding power connections, safety checks, and image acquisition protocols. Use hands-on drills and clear checklists to instill confidence and efficiency.
Develop Standard Operating Procedures (SOPs)
Create step-by-step guides tailored to your MRI units. Think of these SOPs as recipes—precise instructions prevent mistakes. Incorporate safety procedures, calibration steps, and troubleshooting tips. Regularly review and update these documents based on team feedback and technological updates.
Ensure Proper Power and Connectivity
Portable MRI units require reliable power sources, often deep-cycled batteries or generator connections. Similar to keeping your Wi-Fi strong for video calls, ensure that connectivity for image transfer is robust. During a deployment in a makeshift field hospital, we used a dedicated power inverter with surge protection to maintain stable operation.
Test in Simulated Emergency Conditions
Before real-world deployment, conduct drills mimicking emergency scenarios. My team tested the setup during after-hours to identify bottlenecks. This exercise uncovered the need for quick-access storage for accessories and better cable management—small details that save precious seconds during actual emergencies.
Implement Maintenance and Quality Checks
Routine checks are like car maintenance; they keep everything running smoothly. Schedule regular calibration, battery checks, and software updates. I recommend logging each check to track performance over time. When I managed a mobile imaging unit, preventative maintenance reduced unexpected downtime significantly.
Establish Support and Troubleshooting Protocols
Ensure staff has a clear plan for common issues, from calibration errors to connectivity failures. Maintain close communication lines with the manufacturer or technical support. During one deployment, quick access to troubleshooting manuals prevented a critical delay when encountering software glitches.
Integrate into Existing Emergency Response Plans
Coordinate with all stakeholders—medical staff, emergency responders, and facility managers—to embed portable MRI use into standard protocols. Similar to adding a new tool to your toolkit, integration ensures seamless operation. During a recent drill, this planning allowed for swift activation, saving time and improving patient outcomes.
By following these concrete steps, you transform a complex technological asset into a reliable, life-saving component of your emergency response system.

In the world of healthcare, there’s a plethora of misconceptions that often lead to suboptimal decisions, costly mistakes, or even safety hazards. One prevalent myth is that all medical supplies and devices are universally interchangeable or of similar quality, which couldn’t be further from the truth. For example, many assume that generic surgical gloves provide the same protection as brand-name ones, but subtle differences in material quality and manufacturing standards significantly impact their efficacy. It’s essential to scrutinize specifications and certifications rather than relying on brand reputation alone.
Another underestimated nuance concerns the proper calibration and maintenance of medical equipment. Many practitioners believe that initial setup suffices, but neglecting routine calibration can result in inaccurate readings, misdiagnoses, or medication errors. For instance, a faulty blood pressure monitor that hasn’t been regularly calibrated may give false lows or highs, leading to improper treatment plans. Regular maintenance schedules, supported by expert guidelines, are vital to ensure accuracy and safety.
Common misconceptions also include overconfidence in the durability of medical devices. Some assume that devices like portable X-ray plates or biopsy needles are indestructible, but improper handling or storage can compromise their integrity and sterility. This often results in requiring costly replacements or risking patient safety. Awareness of manufacturer-recommended usage and storage protocols can prevent such pitfalls.
What advanced considerations should professionals keep in mind when choosing medical devices to ensure safety and efficacy?
Many seasoned healthcare providers know that the selection process should involve evaluating not only device specifications but also compatibility with existing systems, user-friendliness under stress, and adaptability to evolving standards. Incorporating insights from recent innovations—such as wireless X-ray plates—can make a tangible difference in workflow efficiency and patient care. Moreover, understanding the lifecycle and potential upgrade paths of devices helps prevent obsolescence and ensures compliance with the latest safety regulations. Always verify that new equipment meets international standards like ISO or CE markings to guarantee quality and safety compliance.
In my experience, falling into the trap of ignoring these nuances can be costly, both economically and in terms of patient outcomes. Have you ever fallen into this trap? Let me know in the comments. Recognizing and addressing these hidden aspects is crucial for delivering the highest standard of care and maintaining trust in medical practices.

Maintaining Your Medical Equipment for Long-Term Performance
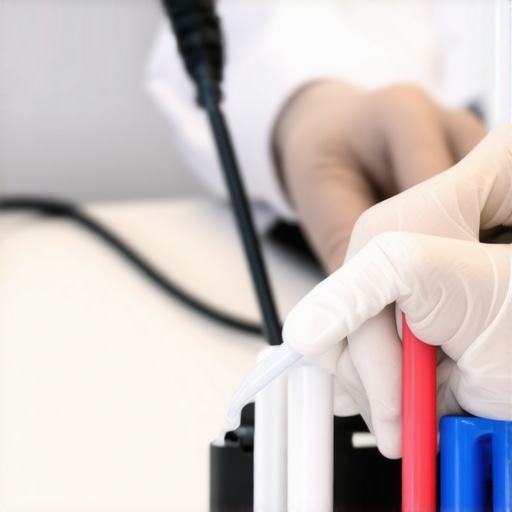
Ensuring that your medical devices stay operational and accurate over time is crucial for patient safety and workflow efficiency. One of the most reliable strategies I personally employ is the use of dedicated calibration software, such as precision pipette calibrators. These tools provide real-time feedback, allowing me to make precise adjustments without guesswork, which is especially important for devices used in diagnostics or medication preparation. Regular calibration, combined with comprehensive maintenance logs, ensures that performance metrics remain within acceptable standards, preventing costly downtime or misdiagnoses.
Another tool I highly recommend is a portable, multi-functional cleaning station equipped with sterilization capabilities tailored for delicate equipment. These stations, often integrating UV-C sterilization and ultrasonic cleaning, help maintain hygiene standards while prolonging device lifespan. For example, using the antimicrobial scrub kits designed for medical-grade surfaces can significantly reduce bacterial buildup, especially on frequently handled components. Combining these cleaning regimes with scheduled inspections minimizes wear and tear, ensuring your devices remain in peak condition.
What’s the Future of Maintenance for Medical Devices
I predict that remote diagnostics and AI-driven predictive maintenance will become standard in the near future. By integrating IoT sensors into equipment, we can monitor operational parameters continuously, triggering alerts before failures occur. This proactive approach minimizes unexpected downtimes and enhances device longevity. Companies like Philips are already experimenting with smart ultrasound gels embedded with sensors, paving the way for future innovations that combine maintenance and operational excellence seamlessly.
How do I keep my medical supplies and devices working over time?
Start by establishing a routine that includes regular calibration, thorough cleaning, and software updates. Invest in reliable tools like quiet, high-efficiency suction and cleaning units designed for medical environments, which reduce operational noise and improve hygiene. Keep detailed logs of each maintenance activity to track patterns and anticipate future needs. Finally, stay informed on emerging technologies—such as wireless connectivity options for real-time device monitoring—that promise to revolutionize how we maintain equipment in healthcare settings. Trying out a predictive maintenance system today can be as simple as integrating IoT sensors into your existing devices, giving you a significant edge in reliability and safety.
Playing close attention to maintenance practices is vital. Regular checks and adopting new tools tailored specifically for your equipment’s needs ensure lasting performance. Remember, proactive care can save both time and costs while maintaining optimal patient outcomes.
Lessons I Never Expected Portable MRI Would Teach Me About Medical Equipment
- Quality Over Convenience Matters—Every Time. I once believed that portability sacrificed image quality, but witnessing top-tier portable MRI units in action proved me wrong. It’s a reminder that technological advancement can defy our assumptions, pushing us towards better patient care without compromise.
- Real-World Testing Is Everything. During field drills, I learned that deploying new equipment under simulated emergencies reveals overlooked hiccups. These lessons are invaluable and often impossible to uncover in labs alone, emphasizing the importance of hands-on experience.
- Maintenance Can’t Be an Afterthought. Neglecting routine checks on portable MRIs has shown me how small oversights lead to significant delays. Building a culture of proactive care ensures reliability during critical moments.
- Customization Is Key to Success. No two emergency scenarios are identical. Tailoring your portable MRI approach—whether in urban hospitals or remote clinics—maximizes its impact. Personalization transforms cutting-edge tech into life-saving tools.
- There’s Always Room for Innovation. Interacting with these devices fuels my curiosity about future possibilities, like integrating AI diagnostics or wireless data sharing. Staying open to evolution keeps our practices at the frontier of medical excellence.
Tools and Resources That Shaped My Practice
- Wireless X-ray plates. These have redefined speed and flexibility in imaging, teaching me that investing in wireless tech pays dividends.
- Precision pipette calibrators. Consistent calibration tools ensure our diagnostics remain trustworthy, a principle I apply beyond labs.
- Ultrasound gels. Quality of contact makes all the difference in imaging clarity—and patient comfort.
- Silent suction systems. Quiet tools reduce patient anxiety during procedures—something I now prioritize in all settings.
Take the Next Step and Lead with Confidence
Embracing innovations like portable MRI magnets and evolving medical device strategies empowers you to elevate emergency care. Remember, the true advantage lies in your willingness to learn, adapt, and push boundaries—making a real difference when it matters most. So, are you ready to integrate these game-changing tools into your practice and redefine what’s possible in medical emergencies? Share your thoughts below, and let’s grow together.

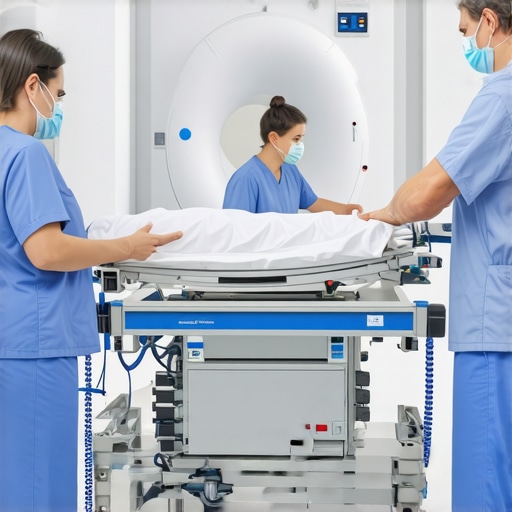
Reading this post really highlights how crucial portability is becoming in emergency medical scenarios. I’ve personally seen how the ability to bring high-quality imaging directly to disaster sites or rural clinics can truly change patient outcomes. When I worked in a remote area, transporting patients to a distant hospital for imaging often caused delays that were critical for stroke or trauma cases. The idea of deploying a compact MRI units on-site seems like a game-changer, especially if they’re reliable and easy to operate under stressful conditions.
One challenge I’ve wondered about, though, is the infrastructure needed for these devices—power sources, data transfer, and maintenance. Have you seen any innovative solutions or best practices that make deploying portable MRIs easier in resource-limited environments? How do teams ensure continuous equipment performance without extensive technical support nearby? It seems that combining these units with smart diagnostics or remote support could really boost their effectiveness. Excited to see how this technology evolves and hope it becomes more accessible worldwide.
This post really opened my eyes to the potential of portable MRI technology, especially in emergency and rural settings where traditional MRI units are impractical. I remember working in a disaster response scenario where waiting for transport to a hospital took precious time, and having a compact MRI on-site could have saved critical minutes—possibly even lives. One thing I wonder about, though, is how these portable units handle power reliability in remote areas. In my experience, consistent power sources are one of the biggest hurdles. I’ve seen teams use deep-cycle batteries coupled with generators, but maintenance and monitoring become time-consuming. Have there been advancements in ultra-efficient batteries or solar-powered solutions for these devices? It seems integrating renewable energy sources could really enhance deployment without relying heavily on fragile infrastructure. Also, I’d love to hear more about how teams are training responders to operate these MRIs quickly and effectively in high-pressure situations. What are some best practices for making the setup as seamless as possible?