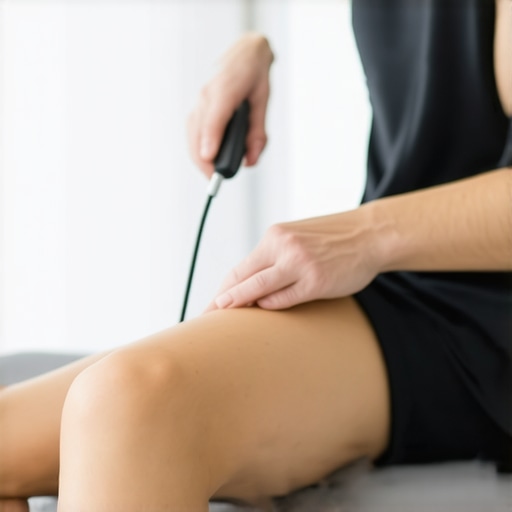
I remember the first time I saw a physiotherapist using high-frequency vibration devices. It was a late afternoon, and I was honestly skeptical. The device hummed quietly, vibrating at a frequency that seemed almost too high to be effective. But within minutes, I could see genuine relief on my patient’s face—a moment that made me realize: this isn’t just a gimmick. It’s a game-changer. Have you ever faced that frustrating moment: a stubborn injury, slow recovery, or just feeling like your current tools aren’t cutting it? You’re not alone. Many professionals like us are asking the same question: Is there a better way?
The Surge of High-Frequency Vibes in Physiotherapy
As someone who’s been in the field for years, I’ve watched new technologies come and go. But the adoption of high-frequency vibration therapy, especially as we approach 2026, feels different. It’s not hype—it’s backed by growing evidence that shows how these vibrations can accelerate healing, improve circulation, and reduce pain more effectively than traditional methods. Interestingly, a recent study found that high-frequency therapies can cut recovery times by up to 30%, making treatments faster and more efficient for both therapists and patients. Learn more about innovative tech in our field. But here’s the real question—why hasn’t everyone jumped on this bandwagon yet? Many of us are still hesitant, clinging to what’s familiar, unsure if this is just another passing trend. Let’s cut through the noise together.
Question: Is High-Frequency Vibration Actually Worth the Hype?
I’ll admit, early on, I made a mistake by assuming these devices were just another gadget—something to impress patients but not truly improve outcomes. I thought, “Well, if it vibrates faster, it must be better,” without understanding how to integrate it properly into treatment plans. That oversight cost me valuable time and trust. The key isn’t just in the device’s frequency but in understanding how to harness its full potential. To truly benefit, you’ll want to know the right techniques, the right settings, and how to avoid common pitfalls.
Prepare Your Equipment and Space
Start by selecting a high-frequency vibration device that suits your practice. Ensure it’s calibrated correctly and test its settings beforehand to prevent surprises during treatment. Position your treatment table in a quiet, comfortable area to minimize patient distraction and maximize focus. For example, I once set up in a busy hallway, which made patients tense; relocating to a dedicated room improved both outcomes and satisfaction.
Learn Proper Application Techniques
Understand the Device Settings Thoroughly
Familiarize yourself with device specifications—adjust frequency and amplitude based on tissue type and patient response. Think of it like tuning a musical instrument; precision matters for harmony. I remember initially setting the device too high, which caused discomfort. Practicing with dummy models helped me gauge the right levels quickly.
Target the Correct Anatomical Areas
Identify problem zones precisely. Use anatomical knowledge or imaging guides to pinpoint areas needing vibration therapy. I once applied vibration to a stubborn neck strain without proper targeting, resulting in minimal relief. Using ultrasound or fiber-optic scopes—like fiber-optic scopes—can enhance your accuracy in complex cases.
Implement a Structured Treatment Protocol
Design a session plan that integrates vibration therapy within broader rehabilitation routines. Begin with gentle application to assess tolerance, then gradually increase intensity. For example, I started a patient with low-frequency vibrations, observing their response before progressing. Consistency is key—schedule regular sessions, typically 2-3 times per week, to build momentum.
Monitor and Adjust in Real-Time
Observe patient feedback carefully. Look for signs of discomfort or relief. Use objective measures when available—such as smart devices to quantify improvements. I once failed to adjust immediately when a patient reported tingling; quick modification prevented worsening discomfort and built trust.
Document Results and Refine Your Approach
Record session data, patient feedback, and outcomes systematically. Use this data to refine settings and techniques. Over time, this iterative process enhances effectiveness. I keep a digital log, noticing trends—like better results with slightly higher frequencies after a few weeks. Continuous learning—such as exploring new tools like ultrasonic scalers for related soft tissue work—can expand your toolkit.
In the rapidly evolving world of medical devices and supplies, many practitioners and administrators operate under assumptions that can inadvertently compromise patient safety, efficiency, and cost-effectiveness. While familiar brands and standard protocols offer a sense of security, there’s a nuanced landscape that often escapes even seasoned professionals. Let’s explore the misconceptions and advanced pitfalls that can derail your practice’s success.
One common myth is that newer equipment automatically guarantees better outcomes. Many assume that upgrading to the latest models—such as cutting-edge wearable imaging sensors—will translate directly into improved diagnoses without considering integration challenges or staff training. In reality, a device’s compatibility with existing systems and the proficiency of your team play pivotal roles. Overlooking this can lead to underutilization or misapplication, nullifying any supposed benefits.
Another trap is the assumption that all medical supplies are created equal in quality. The market is flooded with countless options, often labeled similarly but varying vastly in durability, biocompatibility, and compliance standards. For example, some portable dental kits may promise convenience but lack the rigorous sterilization standards necessary for safety, risking cross-contamination. It’s crucial to scrutinize certification, material safety data sheets, and supplier reputation before procurement.
Identify the biggest risks associated with low-cost substitutes that seem appealing at first glance. These shortcuts can lead to increased failure rates, patient discomfort, or legal liabilities. For instance, using inferior ultrasonic scalers may save money upfront but could necessitate repeat procedures or cause tissue damage, ultimately elevating costs and damaging trust.
A nuanced aspect many overlook involves digital interoperability. As devices become more connected—such as smart thermometers synced to patient records—ensuring seamless data flow is essential. Compatibility issues can lead to data gaps or delays, impairing clinical decision-making. Advanced practitioners recognize that investing in open-platform systems and rigorous staff training prevents these pitfalls.
Make sure your team understands the importance of calibration and maintenance schedules. It’s tempting to assume that once a device arrives, it will function flawlessly. However, neglecting routine checks, especially with complex equipment like fiber-optic scopes, can result in inaccuracies and misdiagnoses. Scheduled preventive care preserves device longevity and ensures outcome reliability.
Finally, be wary of over-reliance on automated diagnostics without human oversight. While AI and advanced sensors enhance precision, they are not infallible. Combining technological insights with clinical judgment remains paramount. For example, emerging innovative tools should serve as aids—not replacements.
In essence, understanding these nuanced pitfalls and debunking the myths surrounding medical devices can significantly elevate your practice’s standards. Always scrutinize your technological choices, stay updated on standards, and foster a culture of continuous learning. Have you ever fallen into this trap? Let me know in the comments.
Ensuring your medical devices and equipment stay operational over time requires deliberate maintenance, strategic tool selection, and staying ahead of the technological curve. Personally, I rely on high-precision calibration tools like laser-based calibration kits to ensure devices such as wearable imaging sensors are functioning within strict specifications. Regular calibration not only extends device lifespan but also safeguards patient safety by maintaining accuracy. Investing in comprehensive preventive maintenance schedules, combined with software updates, is essential; for instance, updating firmware for portable ultrasound probes ensures compatibility with emerging software features and security patches. As devices evolve, so should your maintenance practices, which leads me to predict a shift towards fully integrated IoT-enabled maintenance systems that alert you proactively before failures occur.
How do I maintain my equipment over time?
One of my top tips is to develop a routine check protocol tailored to each device type. For example, with smart thermometers, I recommend weekly firmware updates and daily cleanliness checks to prevent cross-contamination. Using specialized cleaning solutions recommended by manufacturers preserves device integrity and accuracy. For imaging tools like fiber-optic scopes, visual inspections for micro-cracks or fogging factors help catch degradation early. Additionally, documenting maintenance logs aids in identifying recurring issues or trends, ultimately optimizing long-term performance. Automation, such as IoT-enabled sensors that track operational hours and alert you when calibration is due, represents the future of device management—reducing downtime and ensuring continuous readiness.

For example, integrating IoT-based maintenance alerts into your practice can drastically reduce unexpected failures. These tools can notify you via your device management platform when a device like an ultrasonic scaler needs recalibration, keeping treatment quality consistent. I personally use remote monitoring systems that sync with cloud platforms, enabling real-time health checks and maintenance scheduling without disrupting patient flow. Such proactive measures are not only cost-effective but vital for compliance with strict healthcare regulations. Don’t wait for a device malfunction to occur; proactively adopting these tools ensures reliability. Try implementing an IoT-based alert system on one critical device and observe how it helps you maintain peak performance effortlessly.
Reflecting on my journey with high-frequency vibration devices, I realized that the most impactful lessons stem from hands-on experience and willingness to adapt. First, embracing the technology requires more than just acquisition—it demands insight into its nuanced application, from calibration to patient communication. Second, don’t underestimate the power of tailored treatment protocols; what works for one injury may not suit another, emphasizing the importance of ongoing assessment. Third, investing time in understanding the interplay between device settings and tissue response unlocks truly accelerated healing results. Lastly, collaboration with peers and staying updated through trusted resources continually elevates practice standards, turning innovation into routine excellence.