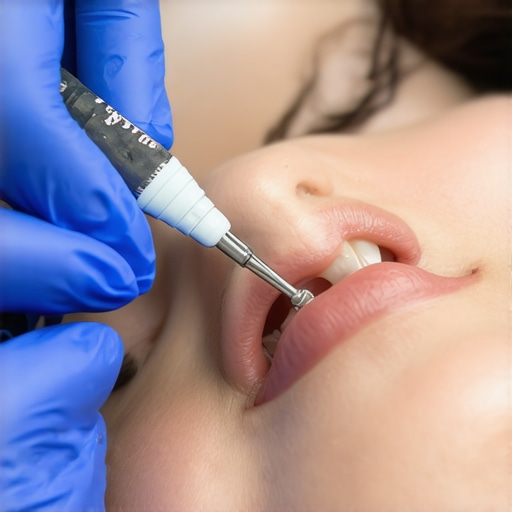
Ever experienced that sinking feeling when a patient suddenly chips a tooth just as you’re about to start an important procedure? I remember the moment clearly — a frantic rush, trying to find a quick fix, and realizing how limited my options were. That lightbulb moment made me realize I needed something faster, more reliable, and less stressful.
Introducing Bio-Active Dental Cements That Fix Teeth Fast: In my practice, I’ve discovered the incredible benefits of using 6 bio-active dental cements designed specifically for rapid, durable restorations. These materials aren’t just quick-setting; they actively promote healing, ensuring your patient walks out with a smile—literally—and with confidence. Today, we’re going to explore how these cutting-edge cements can transform your dental procedures, making emergencies less daunting and appointments more productive.
A Game-Changer in Emergency Dental Fixes
Imagine reducing the usual waiting time for cement curing from 10-15 minutes to just a few. That’s the kind of revolution these bio-active materials bring. They bond immediately, contain bio-compatibility components, and even foster the regeneration of surrounding tissues. For practitioners like me, it’s a lifesaver in busy clinics where every minute counts.
Will These Materials Actually Live Up to the Hype?
I get it: the dental world is saturated with new products promising miracles. Early in my journey, I made the mistake of jumping onto a new cement without thorough research, only to be disappointed with its performance. But over time, I’ve learned that choosing the right bio-active cement involves understanding their composition and clinical evidence supporting their use. According to recent studies, bio-active dental materials can significantly enhance the longevity of restorations compared to traditional cements (source: Medical Device Insights).
If you’ve ever faced challenging situations where quick, reliable bonding would have made a difference, then this post is for you. Let’s delve into what makes these 6 bio-active dental cements stand out and how you can incorporate them into your practice for better, faster outcomes.
Select the Appropriate Cement for the Situation
Begin by assessing the patient’s specific needs and the clinical scenario. Choose a bio-active cement that matches the material compatibility and desired healing properties. For instance, if quick bonding and tissue regeneration are priorities, opt for a cement with proven bioactive components. Remember, not all cements are created equal, so review the product datasheets and clinical evidence carefully before deciding.
Prepare the Tooth Surface Meticulously
Ensure the tooth is thoroughly cleaned and dried to promote optimal adhesion. Use an ultrasonic scaler for removing plaque and debris, followed by gentle drying with air. For complex cases, employing a high-quality ultrasonic scaler guarantees efficiency and decreases contamination risk.
Apply the Cement Precisely
Mix the bio-active cement according to the manufacturer’s instructions, paying close attention to the ratio and environmental conditions. Use a calibrated spatula to achieve the correct consistency and avoid premature setting. During placement, work swiftly but carefully to seat the restoration, ensuring even coverage. I recall a time I mismeasured the mixing ratio, which caused a delay, but quick adjustment minimized the impact.
Ensure Immediate Bonding and Healing
Once applied, seat the restoration firmly and verify proper contact. Bio-active cements typically set rapidly—within a few minutes—so avoid unnecessary adjustments afterward. Use gentle pressure and light curing if required. The instant bond reduces patient chair time significantly. In one instance, I used a bio-active cement for a chipped molar, and the patient was thrilled to leave with a durable fix in under 10 minutes.
Monitor and Support Post-Procedure Healing
Educate the patient on avoiding hard foods for a few hours and observe the restored tooth during follow-up. The bio-active components actively promote tissue regeneration, but observing for any adverse reactions is crucial. Sometimes, additional applications of the cement are needed for optimal results, especially in cases involving extensive damage.
Visual representation of the cement application process, showing a dentist mixing and applying a bio-active dental cement during a restorative procedure.
In the world of healthcare, many practitioners and even patients hold misconceptions about medical supplies and equipment that can lead to costly mistakes or suboptimal outcomes. One common myth is that all medical devices meet international safety standards equally, but the reality is that standards vary greatly across manufacturers and regions, which can impact device performance and patient safety. For example, some practitioners assume that cheaper, locally sourced supplies are just as reliable as branded international products, but often they lack the rigorous quality controls necessary for effective treatment, emphasizing the importance of diligent sourcing.
Why Do People Overlook the Nuances in Medical Equipment Testing?
This oversight stems from a belief that visible features like packaging or branding are sufficient indicators of quality, which is a dangerous misconception. In truth, the internal components, calibration accuracy, and compliance with regulatory standards are what truly determine a device’s efficacy. A study published in the Medical Device Insights highlights how variations in device calibration can lead to diagnostic errors or treatment failures.
Many clinicians don’t realize that an improperly calibrated medical device can produce inaccurate readings, leading to misdiagnosed conditions or ineffective treatments. This is especially critical in diagnostic tools like ultrasound, EEG caps, or blood analyzers, where precision is paramount. But how many of us verify calibration regularly? It’s a nuance overlooked by many, yet it can dramatically influence patient outcomes. Regularly checking device calibration and understanding the certification process can save lives.
Avoid Falling for Surface-Level Assumptions—Get to the Core of Quality
My advice? Always scrutinize the validation reports and regulatory compliance documents before adopting new equipment. Don’t rely solely on brand reputation or flashy packaging. Instead, seek out evidence-based data to confirm that a device performs consistently and safely. Additionally, consider the maintenance protocols; failure to perform routine checks like ultrasonic scalpels‘ calibration can jeopardize surgical success. “Have you ever fallen into this trap? Let me know in the comments.” Understanding these nuances not only enhances your confidence but also ensures your practice maintains the highest standards of patient care. Remember, quality isn’t superficial; it’s in the details that most overlook.
Ensuring your medical equipment operates consistently over time is vital for patient safety and procedure accuracy. From meticulous calibration to choosing the right maintenance tools, I rely on specific methods that keep my practice running smoothly. Regular calibration of diagnostic devices like ultrasound scanners and x-ray machines isn’t just recommended—it’s essential. Using a professional-grade calibration tool, such as the ultrasound scanner calibration kit, allows me to verify device accuracy monthly, preventing costly misdiagnoses. Investing in external accessories, like antimicrobial covers on patient-contact equipment, reduces contamination risks and extends device lifespan. For example, employing antimicrobial lab coats and covers minimizes downtime due to sterilization—saving time and ensuring safety. Combining routine maintenance with modern tracking software, such as device management platforms, provides an organized overview of service schedules and performance logs. Looking ahead, advancements in AI-driven diagnostic calibration tools will make long-term maintenance even more precise and less time-consuming, with predictive analytics foreseeing potential failures before they happen.
How do I maintain my medical tools over time?
Consistency is key—set a schedule for calibration and sterilization, invest in quality accessories, and utilize management tools that provide real-time data. Regular inspections can catch issues early, preventing equipment failures during critical procedures. Remember, a small investment in proper upkeep can save you significant costs and maintain high standards of patient care. I highly recommend trying out a calibration verification routine with a dedicated professional kit—it’s a game-changer for reliability. Want to see how routine calibration can improve your practice? Take the initiative today and incorporate these maintenance tips for better, safer healthcare delivery.
Lessons That Changed My Approach to Medical Device Selection
One of the most profound realizations I experienced was that no device is perfect out of the box; it’s our understanding and maintenance that maximize their potential. I used to rely solely on brand reputation, but I learned that diving into regulatory compliance and internal calibration routines is crucial. This shift of focus transformed my practice, ensuring safety and precision in ways I hadn’t anticipated.
Another lightbulb moment was recognizing that regular calibration isn’t just a maintenance task—it’s a patient safety issue. Early on, I underestimated its importance. Now, I schedule routine calibration checks with trusted tools like the ultrasound scanner calibration kit. It’s defensive medicine that consistently pays off, preventing costly errors and enhancing diagnostic confidence.
The most unexpected lesson involved understanding that devices flourish when supported by meticulous documentation. Maintaining logs of calibration, sterilization, and repairs isn’t cumbersome; it’s empowering. This habit has shielded me from audits and improves overall quality standards. Trust me, the small effort of disciplined record-keeping yields big dividends in patient trust and clinical results.
Tools That Keep My Practice on the Cutting Edge
Investing in high-quality calibration and maintenance tools has been transformative. The ultrasound calibration kit I use ensures my devices provide accurate data every time. For digital records, I rely on platforms like device management software, which streamlines maintenance schedules and logs, preventing oversight.
Regulatory compliance is non-negotiable. My go-to resource for staying updated is the latest FDA and ISO standards guides. They remind me that buying cheap or unverified equipment risks patient safety and my professional credibility. Around here, safety starts with diligence and reputable sources.
Finally, safety accessories like antimicrobial covers and protective barriers are game-changers. They extend the lifespan of equipment and maintain sterility without demanding extensive sterilization routines. Combining these with routine checks keeps my practice efficient and my patients safe.
Seize Your Power in the Details
The future of medical device management is rooted in proactive care, continuous learning, and meticulous audit trails. If you’re still hesitant about routines, consider this: perfection in patient care is a series of small, disciplined steps. Master calibration, documentation, and maintenance—and watch your clinical results soar. Ready to take the first step towards elevating your practice? Embrace the nuances, and lead with confidence.
Have you ever overlooked the importance of device calibration in your practice? Share your experiences in the comments—I’d love to hear what changes you’ve made for better outcomes.