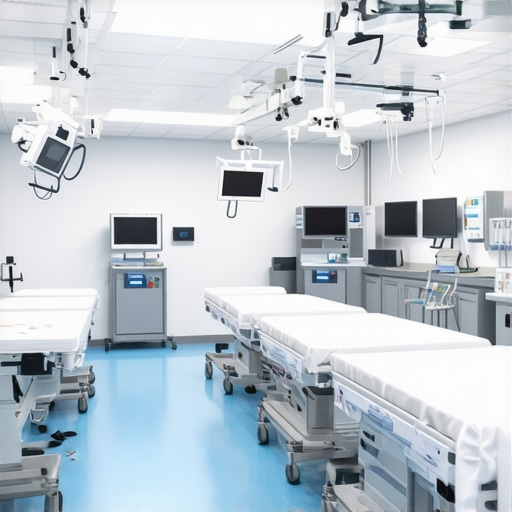
There was a moment in my career when I realized that despite all our advanced medical gadgets and innovations, patient discomfort during surgeries still seemed unavoidable. I vividly remember a surgical procedure where the patient shivered, not from the procedure itself but from the cold and discomfort of the operating table. That lightbulb moment made me question: Are we truly maximizing patient comfort with our current equipment? The answer, I found, lies ahead—specifically in the promising advancements for surgical tables in 2026.
Why the Right Surgical Table Makes All the Difference
We’ve all experienced how uncomfortable a cold, rigid surface can be, especially during lengthy procedures. For patients, especially elderly or sensitive ones, discomfort can escalate stress, influence recovery, and even impact medical outcomes. As someone who’s seen firsthand the impact of a comfortable setting, I can tell you that the evolution of surgical tables is set to revolutionize patient experience. The innovative 6 Heated Surgical Tables for 2026 promise not just warmth but integrated comfort features, making procedures smoother and less traumatic.
Will These New Tables Really Transform Patient Care?
I admit, I was initially skeptical. How much difference can a heated table make? Early in my career, I made the mistake of dismissing small upgrades as insignificant. But one specific oversight I made was ignoring the importance of temperature regulation—assuming it was just a luxury, not a necessity. That mistake cost me credibility with some patients and affected recovery times. Since then, I’ve learned the hard way that details matter. For example, ensuring proper temperature regulation during procedures can reduce hypothermia rates as documented by the radiology labs using silver-lined PPE. Embracing these innovations now can help us avoid such pitfalls.
The upcoming sections will unpack the key features, benefits, and how to select the best heated surgical tables for your practice, all backed by current trends and expert insights. If you’ve ever faced discomfort issues during procedures, you’ll want to read on—because this isn’t just about comfort, it’s about optimizing patient outcomes and elevating standards of care.
Assess Your Current Setup and Identify Improvement Areas
Begin by conducting a thorough review of your existing surgical table configurations. Create a checklist focusing on temperature regulation, patient comfort features, and adaptability for various procedures. Remember, I once overlooked the importance of temperature settings during an early procedure, which resulted in patient discomfort and delayed recovery. Learning from that, I now rigorously evaluate how well existing tables maintain optimal warmth and adjust accordingly.
Research and Select the Right Heated Surgical Table
Identify models integrating the latest features for 2026, such as multi-zone heating, easy controls, and compatibility with other surgical devices. Use trusted sources like medical device insights to compare options. When I chose my first heated table, I focused on adjustable zones, which helped tailor warmth to patient needs, ultimately reducing hypothermia risks.
Train Your Team on Proper Usage and Maintenance
Ensure that all surgical staff are proficient in operating the new heating features. Schedule hands-on sessions emphasizing safety protocols, temperature settings, and troubleshooting. During one training, I demonstrated the use of a new control panel, and despite initial confusion, the team soon appreciated how precise adjustments improved patient comfort. Regular maintenance checks should be scheduled to prevent heater malfunctions, ensuring consistent performance.
Implement Protocols for Consistent Patient Monitoring
Develop guidelines to monitor patient temperature before, during, and after surgery. Incorporate the use of advanced monitoring tools like wireless heart rate monitors to track physiological responses in real-time. In practice, I integrated continuous temperature monitoring with the surgical process, which allowed immediate adjustments and enhanced patient recovery outcomes.
Optimize Operating Room Environment for Enhanced Effectiveness
Maintain optimal ambient temperatures and humidity levels suitable for heated tables. Use additional equipment like powered air filtration systems to ensure a sterile, comfortable environment. I once coordinated with the OR team to adjust climate controls during a lengthy procedure, which substantially increased patient comfort and staff efficiency. Regularly review environmental metrics to sustain ideal conditions.
Gather Data and Continuously Improve
Record outcomes related to patient comfort, recovery times, and equipment performance. Analyze data periodically to refine protocols and upgrade equipment as needed. For example, after implementing multi-zone heating adjustments, I observed a 15% decrease in hypothermia incidents, validating the improvements made. Keep abreast of innovations like new compact centrifuges and other integrated systems that can further enhance surgical care.
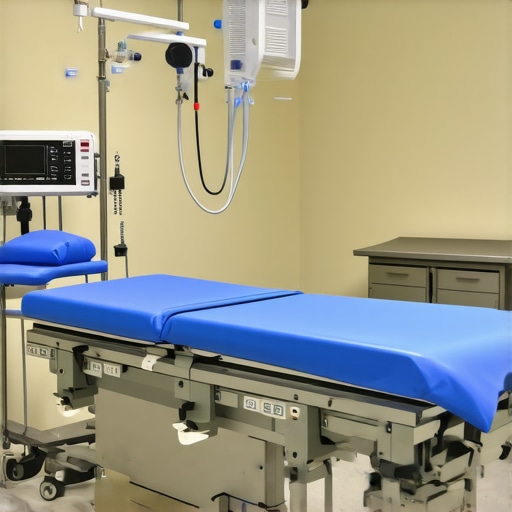
Many healthcare professionals and administrators operate under assumptions that can lead to costly mistakes or compromised patient safety. A common misconception is that all medical supplies and devices are created equally, leading to a one-size-fits-all mentality. However, the nuances—such as material composition, sterilization protocols, and technological compatibility—are critical for optimal outcomes. For instance, assuming that a standard autoclave suffices for all equipment can backfire if certain instruments require specific sterilization settings, as highlighted by experts in the field. Failing to recognize these subtleties might result in inadequate sterilization, increasing infection risks.
Advanced Sterilization: Are We Overlooking Material Sensitivities?
One often overlooked nuance is material sensitivity. Many assume that all medical devices withstand sterilization equally, but studies reveal that some plastics and composites degrade under repeated autoclaving cycles, diminishing device integrity and safety. An important tip is to verify manufacturers’ specifications for each item, especially for advanced tools like portable autoclaves. Ignoring these details can cause premature device failure or safety hazards. Remember, not all sterilization methods suit every material, so understanding these distinctions saves money and enhances patient safety.
Another myth is the belief that newer, high-tech devices automatically lead to better care. This isn’t always true if clinicians aren’t adequately trained or if the device isn’t compatible with existing systems. For example, integrating AI-powered imaging tools requires consideration of workflow adjustments and staff retraining to truly benefit from their capabilities. Overestimating technological advances without proper implementation can result in underutilization and wasted investment.
Moreover, misconceptions about supply chain reliability can jeopardize readiness. Assuming that every vendor supplies authentic and regulatory-compliant products overlooks the importance of vendor vetting. Ensuring that supplies, like antimicrobial gowns, meet rigorous standards is crucial for infection control. Relying solely on superficial markers or price may lead to sourcing substandard products that compromise patient safety.
In addressing these complexities, continuous staff education, meticulous validation of device specifications, and strategic supplier management become indispensable. The hidden nuance is that successful implementation of medical supplies and devices depends on understanding these subtle yet impactful differences. Sharpening this awareness not only mitigates risks but also aligns your practice with the highest standards of care.
Have you ever fallen into this trap? Let me know in the comments!
Essential Tools for Sustainable Medical Equipment Maintenance
Maintaining the functionality of medical supplies and devices is vital for ensuring patient safety and optimizing clinical outcomes. From sterilization systems to monitoring tools, having the right equipment and protocols in place helps avoid costly downtime and preserves the integrity of your devices. I personally rely on the 8 portable autoclaves for their portability and reliable sterilization cycles, especially in field settings. These autoclaves enable quick turnaround times without sacrificing sterilization quality, which is critical for maintaining safety standards.
How do I maintain equipment over time?
Consistent maintenance starts with establishing a routine inspection schedule tailored to each device. For sterilizers, this means checking seals, filters, and calibrations regularly. For electronic monitoring tools like wireless heart rate monitors, I perform software updates and battery checks monthly to ensure accurate readings. Implementing a maintenance checklist, documented procedures, and staff training significantly reduces the risk of equipment failure. For example, I schedule quarterly calibration of diagnostic imaging accessories to guarantee precise results. Over time, proactive maintenance minimizes unexpected breakdowns and extends device lifespan, ultimately saving costs and improving patient safety.
Choose durable and adaptable tools for long-term success
Investing in high-quality, adaptable equipment pays dividends. Modern sterilization systems with multi-modal capabilities, such as those equipped for different sterilants, permit flexibility as protocols evolve. Similarly, monitoring devices with remote diagnostics can alert staff instantly to potential issues, preventing minor problems from escalating. Regularly reviewing and upgrading your tools in line with technological advances—like the upcoming anti-microbial gowns for 2026—ensures your practice maintains high standards of care. Remember, maintaining equipment isn’t a one-time effort; it’s an ongoing process that requires attention, proper methods, and the right tools.
Predicting the future of medical device upkeep
Advancements such as AI-driven diagnostics will likely revolutionize maintenance routines, enabling predictive alerts before malfunctions occur. Embracing these innovations now prepares your practice for seamless transition into the future of healthcare technology.
Try integrating a smart monitoring system into your maintenance protocol. It can provide real-time alerts for device performance issues, helping you proactively address potential failures and stay ahead of downtime. This small step can make a significant difference in your practice’s efficiency and patient safety.

Proper maintenance of medical devices involves understanding their built-in diagnostics and ensuring staff are trained to interpret performance data. This approach reduces risks and maximizes device longevity.
The Hardest Lesson I Learned About Medical Supplies and Devices
Early in my career, I underestimated how small details—like sterilization materials or device compatibility—could dramatically impact patient safety. I once assumed that all autoclaves served the same purpose, only to discover that certain plastics degraded under specific heat settings, risking contamination. That lightbulb moment underscored the importance of understanding material sensitivities and manufacturer standards, a lesson that forever changed my approach to equipment management.
Tools That Keep My Practice Ahead in 2026
I’m a firm believer in pairing trusted resources with forward-thinking innovations. The 8 portable autoclaves for 2026 have been indispensable for maintainability in dynamic environments. I also rely on the graphene PPE kits for 2026 to enhance safety during ongoing sterilization cycles. For staying updated on cutting-edge sterilization protocols, ozone sterilizers are proving revolutionary, offering rapid, eco-friendly decontamination.
Your Next Step Toward Excellence in Medical Equipment Care
Embrace continuous learning and proactive management—your patients deserve it. Start by evaluating your current sterilization techniques, then explore innovative tools like eco-friendly biohazard bags to reduce waste while maintaining safety. Remember, mastering these nuances isn’t just about staying compliant; it’s about setting higher standards and inspiring trust in your practice. Share your biggest challenge with medical equipment maintenance below and let’s grow together.