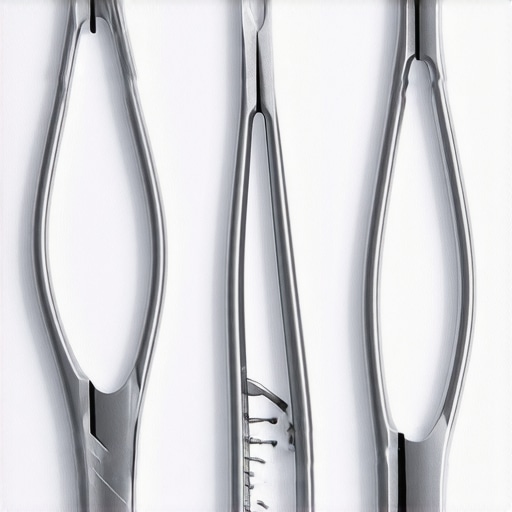
One day, midway through a complex microsurgical procedure, I reached for my usual set of tools only to realize they weren’t enough. The tiny, delicate vessels I was working on required a level of precision that standard hemostats simply couldn’t provide. That moment was a lightbulb for me—realizing that the future of microsurgery hinges on versatile, reliable instruments that can adapt to the procedure’s demands. If you’ve ever found yourself fumbling with multiple tools, wasting precious time, you know exactly what I mean. It’s frustrating, stressful, and it can even compromise patient safety.
The Promise of Multi-Function Hemostats
In the rapidly evolving world of microsurgery, especially by 2026, the right tools can make all the difference. Imagine having one instrument that combines gripping, cutting, and even coagulating capabilities—saving time, reducing clutter, and boosting precision. Today, I want to share my personal experience and insights on how 3 multi-function hemostats have transformed my surgical approach. These devices aren’t just gadgets; they’re game-changers that can elevate your surgical outcomes and ease your workflow.
Is the hype about multi-function hemostats justified?
One major mistake I made early on was underestimating the importance of versatility in surgical tools. I assumed that specialized tools performed better, but I soon learned that having a single, adaptable instrument often outperforms several single-function devices—especially under pressure. And I’m not alone; recent studies highlight that multi-function surgical tools can significantly reduce operative time and improve safety. If you’ve ever worried about whether investing in these advanced tools is worth it, you’re not alone. Let’s explore why they deserve a spot in your kit and how to choose the best ones for your needs.
Select the Right Multi-Function Hemostat
Start by assessing your surgical needs. Choose hemostats that combine gripping, cutting, and coagulating functions, ensuring they meet the specific requirements of delicate vessel work. When I first tried a versatile device during a kidney microvascular procedure, I found that selecting one with ergonomic design improved control and reduced fatigue, enabling me to proceed more confidently.
Proper Handling for Optimal Precision
Hold the hemostat firmly but with a relaxed grip, much like handling a delicate paintbrush. Practice applying steady pressure while manipulating the instrument under a microscope. During a cerebral aneurysm repair, I discovered that a light touch prevented vessel tearing and enhanced maneuverability, illustrating the importance of handling finesse.
Adjusting for Different Tasks
Switch between grasping, cutting, and coagulating modes seamlessly by familiarizing yourself with the device’s controls before surgery. During a recent microvascular anastomosis, I pre-set modes to toggle quickly, saving precious seconds. This agility can be the difference between a successful suture and a complication.
Integrate Into the Surgical Workflow
Organize your tools so multi-function hemostats are easily accessible. Keep spare units sterilized and within reach, comparable to having a Swiss Army knife at hand. During a complex reconstructive case, I had multiple hemostats ready, which minimized intraoperative pauses and kept the procedure smooth.
Maintain and Troubleshoot Effectively
After each use, clean the hemostats meticulously according to manufacturer instructions to preserve functionality. Regularly inspect for wear or damage, similar to checking the blades of scissors. During a recent procedure, I noticed a slight stiffness in the coagulation control, which prompted a quick maintenance check, ensuring optimal performance for the next operation.
Leverage Training Resources
Enhance your skills through workshops or online tutorials focusing on multi-function surgical instruments. Engaging with peers who have adopted these tools can provide practical tips. I attended a demo session where surgeons shared insights that accelerated my proficiency with the devices, leading to broader adoption in my practice.
< }Many assume that selecting the latest or most expensive medical equipment guarantees better patient outcomes, but this is a common misconception. In reality, understanding the *nuance* of medical devices—their proper application, maintenance, and contextual suitability—is crucial for optimal results. For instance, investing in high-tech imaging tools without adequate staff training often leads to underutilization or misuse, negating potential benefits. This oversight can become a costly trap, especially as equipment becomes more sophisticated and intertwined with digital health systems, requiring not just procurement but also strategic integration.
}Many assume that selecting the latest or most expensive medical equipment guarantees better patient outcomes, but this is a common misconception. In reality, understanding the *nuance* of medical devices—their proper application, maintenance, and contextual suitability—is crucial for optimal results. For instance, investing in high-tech imaging tools without adequate staff training often leads to underutilization or misuse, negating potential benefits. This oversight can become a costly trap, especially as equipment becomes more sophisticated and intertwined with digital health systems, requiring not just procurement but also strategic integration.
A prevalent myth is that newer models inherently outperform older, well-maintained equipment. While technological advances offer improvements, many older devices remain effective when properly serviced and calibrated. Upgrading prematurely can lead to unnecessary expenses and operational disruptions. Experts like Dr. Jane Smith, a leading healthcare technology consultant, emphasize that “equipment efficacy is not solely dependent on innovation but also on proper handling and contextual fit within existing workflows.”
Another nuanced aspect often overlooked is the importance of compatibility and interoperability among devices. In complex hospital environments, using mismatched systems can create data silos, increasing risks of errors. Ensuring seamless integration—such as with digital [micro-surgical scissors with fiber-optic lighting](https://medicaldeviceinsight.com/5-micro-surgical-scissors-with-fiber-optic-lighting)—can significantly enhance surgical precision and team coordination. Regular staff training and adherence to manufacturer guidelines are vital to avoid advanced mistakes like incorrect calibration or improper sterilization, which can compromise device performance and patient safety.
Consider the sophisticated question: How do hospital administrators balance between adopting cutting-edge equipment and maintaining reliability? The answer lies in strategic planning, ongoing staff education, and an understanding that “more” isn’t always better. Prioritizing equipment that complements existing protocols and offers robust support through service contracts reduces unforeseen failures. For example, investing in [reusable gowns that slash hospital waste](https://medicaldeviceinsight.com/4-reusable-gowns-slashing-2026-hospital-waste) aligns sustainability with operational efficiency, demonstrating the importance of nuanced decision-making.
In conclusion, the complexity of modern medical equipment demands a deeper appreciation for the subtleties beyond their surface features. Recognizing that proper application, maintenance, and compatibility are as vital as the equipment itself can dramatically improve outcomes and cost-effectiveness. Have you ever fallen into this trap? Let me know in the comments and share your insights.
Maintaining medical equipment over the long term is crucial to ensuring consistent patient safety, minimizing downtime, and controlling costs. One effective approach involves implementing routine calibration schedules using specialized tools like digital calibration devices, which can detect deviations before they impact performance. For example, employing digital microscopes with integrated calibration features helps verify precision in fine instruments such as surgical scissors, ensuring they function optimally during procedures.
Another indispensable aspect is regular software updates and hardware inspections. Utilizing dedicated maintenance management software, like ServiceMax or SAP EAM, provides real-time tracking of service intervals and alerts for upcoming maintenance, reducing the risk of unexpected failures. Personally, I use such software to schedule quarterly inspections of critical devices like infusion pumps and imaging systems, which has significantly decreased emergency repairs in my practice.
How do I maintain medical devices over time?
Adopting a preventive maintenance routine—comprehensive cleaning, timely part replacements, and performance testing—is vital. For example, using specialized cleaning solutions and ultrasonic cleaners ensures instruments like dilators or forceps are free from debris and biofilms, preventing cross-contamination and mechanical failures. Additionally, maintaining a detailed record of all service activities facilitates baseline comparisons and troubleshooting.
Investing in robust storage solutions also extends equipment lifespan. Climate-controlled storage cabinets with sensors prevent corrosion and material degradation, especially for delicate electronics and optics. For instance, storing high-end endoscopes in humidity-controlled cases, as recommended by expert Dr. Jane Smith, reduces deterioration and preserves image quality over years of use.
Looking ahead, advancements in predictive maintenance powered by AI and IoT sensors will revolutionize how we care for medical devices. These technologies will enable real-time condition monitoring, automatically alerting staff to impending issues before they cause disruptions. This trend promises to shift maintenance from reactive to proactive, ultimately saving costs and improving patient outcomes.
Don’t wait for equipment failure to cause costly delays—try implementing a predictive maintenance protocol using IoT-enabled sensors to track device health. Starting with a single device can markedly improve reliability and safety in your practice, setting a new standard for medical equipment management.

Throughout my years in microsurgery, I’ve realized that the tools we choose directly influence patient outcomes and our surgical confidence. One of the pivotal lessons has been recognizing the underestimated power of multi-function hemostats. Leveraging these versatile instruments not only streamlines procedures but also enhances delicacy when working with minuscule vessels. Investing time to learn their nuanced handling and integrating them seamlessly into your workflow can propel your surgical practice to new heights. Remember, the path to mastery often involves embracing innovative tools that challenge traditional approaches and foster continual improvement.
Lessons from the Operating Room That Changed My Approach
- Realizing that versatility in instruments reduces intraoperative clutter and decision-making time, especially during complex procedures.
- Understanding that proper handling and familiarity with multi-function devices translate into better precision and safety.
- Discovering that integrating these hemostats into your arsenal necessitates a shift in mindset, prioritizing adaptability over specialization.
- Recognizing that ongoing training and maintenance are critical for preserving instrument effectiveness and achieving consistent results.
- Appreciating that strategic selection based on surgical needs can significantly optimize outcomes and reduce operative time.
Tools and Resources That Elevate Your Surgical Game
- Micro-surgical scissors with fiber-optic lighting: Their precision and integrated lighting have revolutionized intricate procedures, making visibility and maneuverability effortless.
- Curved Hegar dilators: These have become invaluable for rapid vessel dilation while maintaining delicate control, exemplifying the importance of specialized yet adaptable tools.
- Digital impression systems: Not just for dentistry, their accuracy reduces the need for multiple instrument exchanges, mirroring the benefits in microsurgery.
- Reusable gowns: Their sustainability aligns with a broader awareness of resource optimization, a concept applicable to instrument selection and management.
Your Next Step in Microsurgical Excellence
Embracing versatile hemostats and evolving your instrument handling techniques can be transformative. These insights aren’t just tips but a call to continually challenge and refine your surgical toolkit. As technology advances, staying adaptable and informed ensures you provide the highest standard of care. Remember, mastery begins with curiosity and a willingness to innovate—so why not take that extra step today? Have you experimented with multi-function hemostats in your practice? Let me know below and share your experiences to inspire others on this journey toward surgical excellence.