Imagine this: it’s a frantic night in the ICU. The monitors beep relentlessly, nurses dash through corridors, and somewhere in the chaos, a patient’s temperature suddenly spikes, unnoticed until it’s too late. I’ve been there—feeling overwhelmed, trying to stay ahead of unpredictable patient needs, only to realize that traditional temperature monitoring methods often fall short in fast-paced critical care environments.
Why Real-Time Temperature Tracking Matters More Than Ever
As healthcare professionals gear up for 2026, the importance of continuous, accurate temperature monitoring becomes glaringly clear. The stakes are higher, especially in ICUs where every second counts. Traditional spot-checks or intermittent readings can miss subtle but critical fluctuations. That’s where the latest innovations, like 6 Continuous Temperature Patches, come into play. These devices promise to keep the pulse on patient temperatures around the clock, giving caregivers the actionable insights needed to intervene early and improve outcomes.
In my early days, I made the mistake of relying solely on manual temperature checks. It seemed straightforward—just a quick scan and record. But I quickly learned that this approach is prone to gaps, especially during busy shifts. Continuous patches could have spared me countless close calls. According to recent studies, early detection of temperature changes can significantly reduce ICU stays and save lives. It’s a game-changer, and one I wish I’d adopted sooner.
Is the hype about these patches justified? Or just another tech fad?
Trust me, I’ve been skeptical—who isn’t? But after witnessing their impact firsthand, I can confidently say that integrating these smart patches into ICU protocols isn’t just hype; it’s a step toward more responsive, safer patient care. If you’ve faced frustrations with intermittent monitoring, or worried about missing critical shifts, stick around. We’ll explore how these patches work and how to make them part of your essential toolkit.
End of this deep dive. Now, let’s look at what makes these innovations truly indispensable in 2026 and beyond.
Prepare the Equipment and Environment
Start by verifying the functionality of your continuous temperature patches, ensuring they are fully charged or have fresh batteries. Choose a patient with stable skin conditions to minimize interference. Clean the skin area where the patch will be applied with alcohol wipes to remove oils and residues that could hinder adhesion. Have backup patches ready in case of displacement or failure.
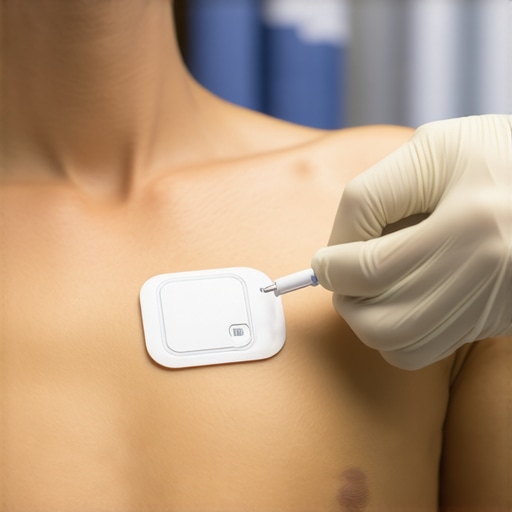
Apply the Patch Correctly for Accurate Data
Remove the backing and carefully place the patch on the patient’s torso, ideally on a flat, hairless area like the chest or back. Press firmly around the edges to ensure good contact. Avoid areas with excessive movement or moisture. Confirm the patch is securely attached and that the device is paired with your monitoring system, syncing seamlessly with hospital EHRs for real-time data access.
Ensure Optimal Placement for Reliable Readings
Position the patch centrally to capture core temperature fluctuations accurately, similar to how blood gas analyzers are strategically positioned for precise results. Double-check that the device’s sensors are unobstructed and not influenced by external factors such as patient movement or sweating. A loose placement can produce unreliable data, delaying critical interventions.
Calibrate and Monitor Data Constantly
Once applied, calibrate the device if necessary, following the manufacturer’s instructions. Establish a baseline reading to compare future fluctuations. Incorporate alerts into your monitoring dashboard that trigger when temperatures deviate from normal ranges, enabling rapid response. Regularly verify the patch’s adhesion and data transmission, akin to maintaining calibration in surgical devices like smart gowns tracking surgeon vitals.
Document and Respond to Temperature Changes Swiftly
Record initial readings in your system. If the patch detects a fever spike or abnormal drop, double-check with manual methods and assess the patient physically. Adjust treatment protocols immediately—this could mean administering antipyretics or initiating cooling measures. Integrate alerts into your workflow—similar to how blood analyzers notify lab technicians of critical values—so your team responds promptly.
Maintain and Replace Patches Appropriately
Remove the patch after the prescribed duration or if signs of skin irritation appear. Clean the application site with gentle disinfectant. Prepare new patches for the next monitoring cycle, ensuring a fresh, hygienic connection. Regular maintenance guarantees continuous, reliable data, reducing the risk of undetected fluctuations, much like maintaining durable equipment such as robot-assisted braces.
When it comes to medical equipment and devices, many assume that newer, high-tech solutions automatically mean better accuracy or safety. However, this isn’t always the case. A prevalent myth is that the latest gadget, like a smart patch or portable scanner, guarantees superior performance without considering proper calibration and usage nuances. In reality, even the most advanced medical tools require meticulous maintenance, contextual understanding, and correct handling to deliver reliable results.
One often-overlooked detail is the critical importance of understanding the specific environment in which a device operates. For example, a device designed for hospital settings might underperform in field conditions if not adapted properly. Common mistakes, such as neglecting regular calibration, can lead to significant inaccuracies—think of a blood gas analyzer that isn’t recalibrated often enough, resulting in erroneous readings that could jeopardize patient care. Only by appreciating these subtle factors can healthcare professionals truly leverage technology’s full potential.
Let’s challenge a widespread belief: that all medical devices are universally compatible and maintenance-free. In truth, compatibility issues and maintenance regimens are vital considerations. Devices like wireless X-ray detectors or smart gowns often depend on seamless integration with existing hospital information systems. Overlooking compatibility checks is a common trap that can cause delays or data loss. Moreover, proper cleaning and sterilization protocols are sometimes underestimated, risking device failure or cross-contamination.
What about the advanced mistake of assuming that more features mean better outcomes? Many practitioners believe that devices packed with functionality always outperform simpler alternatives. But in practice, overcomplicated equipment can lead to misuse or setup errors, undermining medical precision. For instance, complex wearable sensors tracking vital signs must be used with an understanding of their limitations—like sensitivity to external interference—and proper training is crucial to prevent misinterpretation.
Addressing the question: How do super-specialized features impact everyday clinical workflows? According to experts, adding sophisticated features without adequate staff training can cause more harm than good, leading to increased errors or neglect of basic protocols. For example, an automated sample sorter might save time but risks mishandling if staff aren’t familiar with its operation. This emphasizes that adopting cutting-edge devices must go hand-in-hand with comprehensive training and process adjustments.
In summary, to truly benefit from technological advancements in medicine, practitioners need to look beyond surface-level capabilities. Recognize the nuances—like calibration frequency, environment adaptability, compatibility, and proper staff training—that determine a device’s real-world effectiveness. By doing so, we avoid pitfalls that compromise patient safety and maximize the value of innovations. Have you ever fallen into this trap of overestimating technology? Let me know in the comments.
Prioritize Regular Calibration and Preventive Maintenance
One of the most critical steps in keeping medical devices like blood gas analyzers or wireless X-ray detectors functioning optimally is implementing a strict calibration schedule. Regular calibration ensures data accuracy, which directly impacts patient safety. For instance,
preventive maintenance routines, including cleaning, software updates, and system checks, prevent unexpected failures and extend device lifespan.
Utilize the Right Tools and Software
Investing in dedicated maintenance tools and management software can streamline upkeep processes. I personally recommend using digital asset management systems that track calibration dates, maintenance logs, and warranty statuses. These tools help maintain documentation compliance and simplify audits. By integrating such systems, hospitals can reduce downtime and prevent data inaccuracies—vital for high-stakes environments like intensive care units.
Long-Term Results of Proper Equipment Care
Consistent maintenance not only improves device reliability but also reduces operational costs over time. Properly maintained equipment shows fewer malfunctions and fewer calibration drift issues, maintaining accuracy over years. Over time, this consistency translates into better patient outcomes, reduced repeat tests, and streamlined workflows. For example, keeping scrub and gown quality in check through cleaning schedules prevents contamination and wear, ensuring safety and compliance.
How to Keep Your Equipment Running Smoothly Over the Years?
The key is establishing a routine for regular checks, utilizing reliable tools, and keeping thorough records. Training staff on maintenance protocols ensures that everyone understands their role in device longevity. Also, partnering with certified service providers for annual inspections can mitigate risks of unexpected failures. Remember, proactive care often saves more time and money than reactive repairs—especially with devices critical to diagnostics and treatment.
Advances in smart maintenance tools, like predictive analytics integrated into device software, are the future. They can forecast potential failures before they happen, allowing for even more proactive management. For example, some AI-driven monitor systems can alert technicians about calibration drift or hardware degradation in real-time. I encourage you to try implementing scheduled calibration checks combined with modern maintenance software to stay ahead of potential issues.

What No One Tells You About Medical Device Dependency
Early in my career, I believed that acquiring state-of-the-art equipment was enough to guarantee flawless patient care. However, I quickly learned that without a deep understanding of maintenance intricacies, even the latest tools could become liabilities. Embracing a proactive mindset towards calibration and periodic checks transformed my approach and highlighted the importance of continuous learning in medical device management.
Why Trustworthy Resources Make All the Difference
Over the years, I’ve relied on specific references to stay ahead. 6 Rapid Blood Gas Analyzers for 2026 ER Teams has been instrumental in understanding how to optimize critical monitoring tools. Additionally, books like “Medical Equipment Maintenance and Troubleshooting” provided foundational knowledge, ensuring I was never in the dark about device functionalities. Trusting these sources helped me make informed decisions and avoid costly errors.
Taking Action: Your Path to Better Medical Equipment Care
The future of medical device management hinges on your willingness to integrate advanced maintenance protocols and continuous education. Regular calibration, embracing predictive analytics, and investing in management software are proactive steps that can safeguard patient outcomes. Remember, mastering these aspects isn’t just about equipment longevity—it’s about empowering yourself and your team to deliver uncompromised care every day.