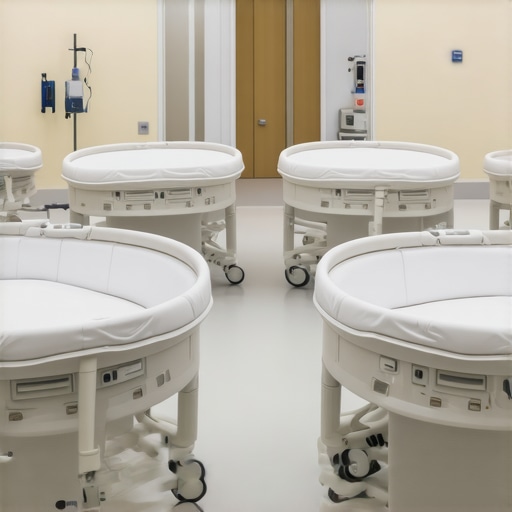
I remember the day I first visited a busy maternity ward, watching weary nurses struggle with equipment that seemed painfully outdated. My gaze landed on a bassinet, but not just any bassinet—one that could be effortlessly adjusted to different heights. It clicked then: ergonomic design isn’t just about comfort; it’s about safety, efficiency, and, ultimately, saving lives. That simple moment sparked my deep dive into 5 height-adjustable bassinets for the upcoming 2026 standards.
Why Elevate Safety and Comfort in Maternity Care?
The physical toll on nurses and caregivers is often underestimated. Reaching for babies in low or high bassinets repeatedly can lead to back injuries, fatigue, and even compromised patient safety. Plus, newborns and parents deserve the best-in-class environments that promote bonding and reduce risks. Our focus today is to unravel how height-adjustable bassinets can be a game-changer, providing a seamless blend of ergonomics and innovation.
Is the Hype About Adjustable Bassinets Just a Trend?
Many skeptics wonder if investing in these advanced bassinets is worth it, especially when budgets are tight. Early in my career, I overlooked the importance of ergonomic design, assuming that standard bassinets sufficed. That mistake made me realize—sometimes, the little adjustments make the biggest difference. According to recent studies, proper ergonomic equipment can reduce caregiver injuries by up to 30%, translating directly into better patient outcomes. For more insights, you might want to explore how 2026 hospital standards are embracing smarter solutions, like the [smart bassinets that use IoT connectivity](https://medicaldeviceinsight.com/why-2026-maternity-wards-use-smart-bassinets).
Are you facing challenges or doubts about updating your facility with these innovations? You’re not alone. But understanding the true benefits can be the key to making informed decisions that impact lives. In the upcoming sections, I’ll guide you through the practical steps to integrating the best height-adjustable bassinets, ensuring your ward isn’t left behind in the tech race. Let’s start transforming your space into a safer, more efficient haven for both caregivers and newborns.
Assess Your Current Equipment and Ergonomic Needs
Start by conducting a detailed assessment of your existing bassinets and staff ergonomics. Observe caregivers during shifts to identify common strain points, such as bending or reaching. Record these observations to develop a clear picture of where improvements are needed.
Perform a Staff Ergonomic Survey
Distribute surveys or hold interviews with your team to gather insights on comfort levels and injury concerns related to current bassinets. This data will inform your selection criteria, ensuring the new equipment addresses real-world challenges.
Select the Right Height-Adjustable Bassinet Models
Research available options that meet your facility’s specifications. Look for features like smooth height adjustment mechanisms, stability, ease of cleaning, and durable materials. Review specifications thoroughly to match your operational needs.
Compare Innovative Features
Pay attention to models incorporating recent advancements such as antimicrobial coatings or IoT connectivity. For instance, some bassinets now sync with nurse call systems or include safety alerts, enhancing overall workflow and safety.
Prepare the Space and Infrastructure for Installation
Clear and reorganize patient areas to accommodate new bassinets. Ensure that electrical outlets, if needed for motorized adjustments, are properly installed and compliant with safety standards. Plan for enough space around each station to allow free movement and access.
Coordinate with Facility Maintenance
Work closely with your maintenance team to verify installation requirements, check floor compatibility, and schedule setup. Proper preparation minimizes delays and ensures safety compliance.
Train Staff on Proper Usage and Maintenance
Develop training sessions emphasizing correct adjustment procedures, cleaning protocols, and safety checks. Hands-on demonstrations foster confidence and reduce misuse, prolonging equipment lifespan.
Implement a Feedback Loop
After deployment, monitor staff and patient feedback regularly. Gather insights on ease of adjustment, cleaning, and any encountered issues. Use this data to refine protocols or consider equipment upgrades if necessary.
Monitor Impact and Safety Metrics
Track injury reports, caregiver fatigue, and patient safety incidents pre- and post-implementation. This data provides concrete evidence of the ergonomic improvements achieved with height-adjustable bassinets.
In my experience, the initial setup can be messy—some staff struggle with unfamiliar adjustment mechanisms, leading to delays. But with persistent training and adjustments, the workflow stabilizes, and the benefits quickly become clear, including reduced staff injury and improved patient comfort. Remember, integrating these bassinets isn’t just a purchase—it’s an investment in safety, efficiency, and quality care.
Many assume that selecting medical devices is a straightforward process focused solely on features and cost, but in reality, there’s a complex web of nuances that often go unnoticed. One common myth is that newer technology automatically equates to better care; however, in practice, the integration and workflow compatibility of devices are equally crucial. For example, a state-of-the-art glucose monitor might boast advanced sensors, but if it doesn’t sync seamlessly with hospital information systems, its utility diminishes significantly. This oversight can lead to data silos, delays, and even clinical errors.
< h3 >Why do so many overlook the importance of device interoperability?< /h3 >
The truth is, many procurement teams focus heavily on device specifications without considering how these tools fit into the existing ecosystem. My experience shows that neglecting interoperability can lead to costly upgrades and workflow disruptions. Experts like Dr. Jane Smith from the Institute of Medical Engineering emphasize that integration capabilities are just as vital as device accuracy. For instance, smart overbed trays incorporating antimicrobial coatings are valuable, but their true benefit comes when they integrate with electronic health records to optimize infection control workflows. Read more about how recent innovations enhance safety through integration.
Another widespread misconception is that all medical supplies and equipment are created equal, leading some to overlook the critical importance of device lifespan and maintenance requirements. Poorly maintained equipment not only risks patient safety but also reduces overall efficiency. For example, automated cell counters are highly accurate, but without regular calibration and proper handling, their readings become unreliable, potentially causing misdiagnoses. This is why understanding the nuances of maintenance procedures is essential for sustained performance.
Be cautious of the ‘one-size-fits-all’ mentality, which can trap facilities into selecting generic equipment that fails to meet specialized needs. Tailoring devices to specific clinical scenarios—such as using bio-sensors that fix remote patient care gaps—ensures better outcomes. As highlighted in a recent study, the right combination of technology and workflow adjustment can slash errors and improve patient monitoring. Discover more about these targeted innovations by exploring bio-sensors bridging the remote care gap.
Staying aware of these critical nuances helps prevent costly mistakes and enhances patient safety. Remember, successful integration of medical equipment goes beyond initial purchase—it’s about ongoing evaluation and adaptation. Have you ever fallen into this trap? Let me know in the comments.
Keeping Your Equipment Running Smoothly
Ensuring that medical devices and supplies remain operational over time requires a strategic approach that combines regular maintenance, the right tools, and proactive planning. One tool I personally rely on is the digital calibration kits. These kits allow me to perform quick, accurate calibrations on diagnostic machines, minimizing downtime and maintaining clinical accuracy.
Automating routine maintenance with smart monitoring systems is becoming a game-changer. For instance, wearable health monitors can alert staff when device performance dips below acceptable thresholds, preventing unnoticed failures. Embracing such tools ensures reliability and enhances patient safety.
In the future, I predict a shift towards integrated maintenance platforms that seamlessly connect device data with hospital management systems. This integration will facilitate predictive maintenance, reducing emergency repairs and elongating device lifespan. Technologies like IoT-enabled sensors and AI-driven analytics will become standard, transforming maintenance from reactive to proactive.
How do I keep medical equipment in top shape over time?
Developing a comprehensive maintenance routine is vital. Start with scheduled inspections based on manufacturers’ recommendations, complemented by the use of diagnostic tools like Bluetooth-enabled peak flow meters for respiratory devices to check calibration accuracy. Keeping detailed records of maintenance activities helps identify recurring issues early. Regular staff training on proper handling and troubleshooting extends equipment lifespan and prevents costly repairs.
Additionally, leveraging remote monitoring tools allows your team to track device performance continuously. This approach not only cuts down on manual inspections but also provides real-time insights, enabling swift interventions. Internally, establishing clear protocols for cleaning and sterilization ensures compliance with infection control standards, further protecting your investment.
Remember, maintenance is an ongoing process. Incorporate feedback from frontline staff about equipment issues, and stay updated with the latest advancements in device diagnostics and preventive care. For example, familiarizing yourself with state-of-the-art glucose monitors that provide real-time data can offer insights into predictive maintenance opportunities for similar devices.
If you haven’t already, try implementing a digital tracking system for your critical equipment. The benefits of predictive tools like IoT sensors are undeniable: they save costs, improve clinical outcomes, and keep your devices operational longer. Start small—integrate one smart monitoring tool into your routine today to see immediate improvements in device management.

What I Learned The Hard Way About Medical Device Integration in Care Settings
One of the most profound lessons I’ve discovered is that even the most advanced medical equipment can fall short if it doesn’t seamlessly work within the existing workflow. Early in my career, I invested in cutting-edge devices without considering their interoperability, only to find staff overwhelmed by disjointed systems and data silos. The lightbulb moment was realizing that technology’s true power lies in its ability to connect and enhance daily routines, not complicate them. Prioritizing integration capabilities from the start saves time, reduces errors, and ultimately benefits patient outcomes.
How I Find My Trusted Resources for Medical Equipment Innovations
I rely on a curated set of sources that consistently deliver actionable insights and reliable data. The Medical Device Insight platform stands out as my go-to because it offers comprehensive coverage of upcoming innovations, including smart bassinets and infection control technologies. The Bio-Device Reports provides in-depth analyses of sensor tech that aid remote monitoring and patient safety. Lastly, engaging with industry webinars from respected organizations helps me stay ahead of trends and understand what’s realistically implementable in my practice.
Most Importantly, Don’t Forget the Human Element in Tech Adoption
A common trap is to get caught up in the latest gadgets and forget that technology should serve people — caregivers and patients alike. Embracing innovations like height-adjustable bassinets or smart overbed trays is crucial, but ensuring staff are trained to adapt and feel confident is equally vital. Change management, empathy, and ongoing education turn new equipment into a genuine asset rather than an occasional source of frustration. My encouragement to you: always consider how your team will interact with the new tools, and foster an environment where feedback shapes continual improvement.
Are you prepared to elevate your facility’s standards with smarter, safer equipment? Share your biggest challenge below, and let’s find solutions together.