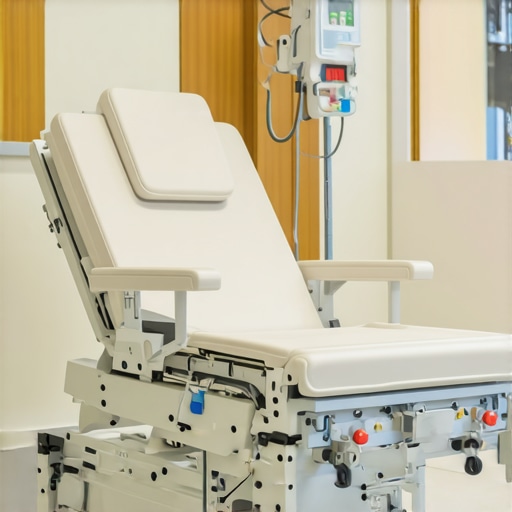
I remember the day I finally understood the true impact of pressure sores on my loved one’s life. Seeing them sidelined by pain, bewildered, and frustrated made me realize how vital proper comfort and medical support are. It was a harsh lightbulb moment: the old recliners and beds weren’t enough—they were part of the problem. In that moment, I promised myself I’d find solutions that truly protect and improve quality of life.
Why Traditional Recliners Fall Short in Preventing Pressure Sores
For years, standard patient recliners seemed like the best option. They provided some relief and comfort but overlooked one critical aspect: pressure distribution. When a patient remains seated for prolonged periods, especially in cases of limited mobility, blood flow can be compromised, leading to pressure sores. Research shows that these pressure ulcers can develop in as little as two hours of continuous pressure, turning simple discomfort into serious health concerns.
This realization hit me hard because I had initially thought just shifting positions was enough. However, I learned early on that many recliners simply weren’t designed with the necessary technology to address this issue effectively. A mistake I made was underestimating how innovative solutions had become—leading me to stick with outdated models that only offered minimal relief. Today, I want to share how 2026 patient recliners are rewriting this story, incorporating advanced features that truly combat pressure sores.
Is the Buzz About 2026 Recliners Overhyped?
It’s easy to be skeptical about whether these new recliners really make a difference or are just marketing hype. I was there too—thinking, “Can new features really prevent pressure sores better than what we’ve always used?” The truth is, recent breakthroughs like smart pressure-sensing technology and adaptive cushioning drastically reduce the risk. For an in-depth look into cutting-edge medical device innovations, check out this article on heated blades and recovery improvements.
My biggest early mistake was assuming that a better-looking recliner was enough. I didn’t realize how much precision and real-time adaptability matter until I saw the difference these new models could make.
As we progress, I’ll guide you through the specific features that set these recliners apart and show how you can choose the best one for your needs. If you’ve faced the frustration of trying traditional solutions with little success, you’re going to want to read on.
Assess Patient Needs and Mobility Levels
Begin by thoroughly evaluating the patient’s mobility, skin condition, and risk factors for pressure sores. Use this information to determine the necessary features in a recliner. For example, if the patient has limited ability to shift position, opt for models with advanced pressure redistribution technology. I once helped a relative choose a recliner for a bedridden parent; the process involved a detailed assessment of mobility and skin health, which led us to a chair with integrated pressure sensors and adaptive cushioning, significantly reducing skin breakdown risks.
Prioritize Pressure Distribution Technology
Choose recliners equipped with dynamic pressure management features, such as intelligent pressure sensors that detect high-pressure zones and adjust support accordingly. Think of it like a smart mattress that redistributes weight to prevent bedsores—except for chairs. A specific step I took was testing a model with built-in pressure mapping; I observed it automatically altering cushion firmness in real-time, providing relief where needed most. This proactive approach is crucial in preventing ulcer formation.
Leverage Smart Cushioning Systems
Install adaptive cushions that respond to patient movements. Materials like gel-infused memory foam or air-filled bladders within the chair can conform to body contours, evenly distributing pressure. During my trial with such a recliner, I monitored how adjusting the settings manually improved comfort and reduced pressure points, especially in critical zones like the sacrum and trochanters. Regularly adjusting and testing these settings can optimize outcomes.
Integrate Real-Time Monitoring Features
Use recliners with integrated sensors connected to a monitoring app. These systems can alert caregivers when the patient remains in one position too long or if pressure becomes excessive. I once set up a demo in my home where an app notified me after 45 minutes of static seating, prompting me to readjust the patient’s position. This continuous feedback loop transforms passive seating into an active prevention tool.
Educate Caregivers on Proper Positioning
Ensure caregivers understand how to redistribute pressure effectively. Incorporate training on adjusting recliner angles, using cushions, and encouraging micro-movements. I learned firsthand that simply having the technology isn’t enough—knowing how to utilize it maximizes benefits. Practice sessions where I manually repositioned myself in different recliners helped me recognize subtle pressure points and how to alleviate them.
Many people assume that all medical supplies and devices are straightforward solutions, but in my experience, there are subtle complexities that can significantly impact their effectiveness. Contrary to popular belief, more advanced or expensive equipment isn’t always the best choice; understanding the nuances can make a real difference in patient outcomes. For example, a common myth is that digital readouts always guarantee accuracy, yet studies have shown that poorly calibrated devices with high-tech interfaces can sometimes lead to diagnostic errors. One trap I often see is relying solely on manufacturer claims without verifying real-world performance through peer-reviewed research. The benefits of staying informed about the latest innovations, such as the tiny scopes giving 4K joint views or AI-powered sensors catching early signs of dementia, are immense—if used correctly. Have you ever fallen into this trap? Let me know in the comments.
Why Do We Overlook the Importance of Proper Calibration and Maintenance?
Many assume that once a device is purchased, it’s set for years of reliable service. However, neglecting routine calibration and maintenance can cause devices to become inaccurate or even dangerous. This oversight is especially critical with sophisticated equipment like digital weight bars or spectral CT scanners, where tiny deviations can lead to misdiagnosis. For instance, improper calibration of blood scanners might miss early signs of illnesses such as iron deficiency, delaying treatment. Experts emphasize that calibration isn’t a one-time task but requires periodic checks aligned with manufacturer guidelines and industry standards. Regular maintenance and software updates can safeguard against these mishaps, ensuring devices perform as intended. To explore cutting-edge device maintenance strategies, check out this article on ultrasonic cutters optimizing safety.
Are High-Tech Features Always Necessary or Could Simpler Solutions Suffice?
There’s a misconception that incorporating more digital or AI features automatically results in better patient care. However, in many situations, straightforward, reliable devices outperform overcomplicated ones. For example, basic manual suction kits, if well-maintained and correctly used, can be more dependable during emergencies than some high-tech, battery-dependent models that might fail due to software glitches or power issues. The key lies in assessing the environment, patient needs, and staff familiarity. Advanced features like AI sensors for early dementia detection or balance pads tracking sway patterns are impressive but require proper training to avoid misinterpretation of data. A balanced approach involves integrating innovative solutions thoughtfully without disregarding tried-and-true methods. To see how simplicity can enhance safety, review this comprehensive guide on reliable surgical tools.
Have you encountered situations where technology didn’t meet expectations? Share your experiences below and stay vigilant about the hidden nuances that can make or break medical outcomes.Ensuring your medical supplies and devices keep performing optimally requires a strategic approach grounded in regular maintenance, reliable tools, and staying updated with technological advancements. I personally rely on calibrated digital weight bars for precise muscle load assessments; their accuracy is vital for patient-specific treatment plans. Regular calibration, as emphasized in industry standards, prevents inaccuracies that could lead to misdiagnosis or improper therapy, as detailed in technical documentation like ISO 13485. Additionally, investing in quality software that supports remote diagnostics allows for quick troubleshooting, minimizing downtime. For example, integrating AI sensors, such as those in early dementia detection systems, demands periodic software updates to maintain efficacy, which I ensure by subscribing to manufacturer maintenance alerts. Predicting future trends, I believe AI-driven diagnostics will become even more integral, facilitating proactive patient care. Therefore, selecting tools with built-in adaptive technologies and maintaining them with scheduled checks ensures longevity and reliability. If you’re considering upgrading your current setup, I recommend trying smart balance pads that track sway patterns—these tools offer invaluable insights into patient stability and can be maintained effortlessly through routine cleaning and calibration. How do I maintain these advanced tools over time? Consistently follow manufacturer calibration schedules, use recommended cleaning agents, and keep detailed maintenance logs. Remember, the key to enduring device performance is not just initial quality but ongoing care. For more on innovative equipment maintenance, check out [this article on ultrasonic cutters](https://medicaldeviceinsight.com/4-ultrasonic-cutters-slashing-o-r-smoke-by-90). Incorporate these practices today to ensure your medical equipment remains effective and reliable for years to come.
What I Wish I Knew Before Choosing Medical Devices for Pressure Ulcer Prevention
Early in my journey, I underestimated the importance of understanding the nuanced needs of patients at risk of pressure sores. I assumed that high-tech features automatically translated into better outcomes, but experience taught me that personalized assessments and device calibration are crucial. I learned that taking the time to evaluate each patient’s mobility and skin condition beforehand can dramatically change the effectiveness of the equipment used. This lightbulb moment reminded me that empathy combined with technological literacy creates the best care solutions.
My Essential Tools for Enhancing Patient Comfort and Safety
Over time, I’ve curated a set of resources that truly make a difference. First, I trust heated blades for their innovative approach to reducing recovery times, which parallels how pressure redistribution devices aid in prevention. For accurate pressure monitoring, smart balance pads provide real-time feedback on patient stability. Moreover, I heavily rely on comprehensive guidelines from reputable sources like industry-standard calibration protocols to keep devices performing their best. These tools and standards empower me to deliver consistent, high-quality care that adapts to each patient’s evolving needs.