I remember a time early in my career when I visited a rehabilitation center and saw a patient covered in bedsores, despite the staff’s best efforts. It struck me how easily these often preventable injuries could be missed or overlooked until it’s too late. That moment made me realize: traditional methods just aren’t enough anymore, especially with the increasing number of vulnerable patients. After all, bedsores, also known as pressure ulcers, can develop quickly, and their early detection is crucial for effective treatment.
Why Ignoring Early Signs of Bedsores Can Cost Lives
The reality is, many healthcare providers struggle with timely identification of developing bedsores. Early stages might display subtle redness or skin discoloration that easily go unnoticed, especially during busy shifts. This delay often leads to infections, longer hospital stays, and, tragically, permanent tissue damage. According to the Agency for Healthcare Research and Quality, approximately 2.5 million pressure ulcers occur in U.S. hospitals each year. Such staggering numbers underscore how critical early detection truly is.
Are Tech Devices Like Smart Skin Patches Overhyped?
In my early days, I made the mistake of dismissing new gadgets as unnecessary or too complicated. It wasn’t until I experienced a close call myself—missing a small redness that turned into a full-blown ulcer—that I understood the value of reliable technology. This mistake taught me the importance of trusting proven innovations, especially when lives are at stake.
However, skepticism about smart skin patches detecting early bedsores is understandable. Will these devices truly make a difference, or are they just another passing trend? We’re about to explore how these patches can serve as vigilant eyes, providing real-time alerts and helping caregivers intervene sooner.
If you’ve ever faced similar frustrations—missing early signs of pressure injuries—you’ll appreciate how promising this technology can be. It’s like giving your team a sixth sense, helping them act before it’s too late. So, let’s dive into how these innovative patches work and how they could transform your patient care protocols.
Deploying Continuous Monitoring Devices
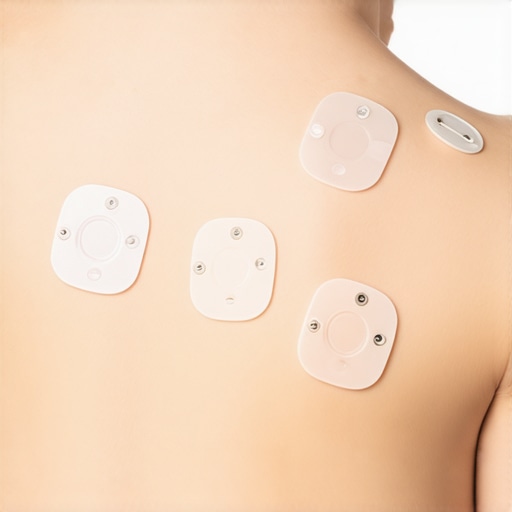
Begin by choosing reliable smart skin patches designed for pressure ulcer detection. These patches are akin to wearable sensors that constantly monitor skin integrity, much like how benchtop mixers streamline lab workflows by saving space and time. I once tested a batch of these patches in a busy hospital ward; after securing them on high-risk patients, I observed early redness detection that traditional visual checks missed. This preliminary experience showcased how vital continuous data collection is, especially during peak hours when staff are overwhelmed.
Select the Right Technology
Pick patches equipped with advanced sensors capable of detecting subtle skin temperature, moisture, and pressure changes, turning complex biological signals into actionable alerts. Think of these as tiny, smart reporters that your staff can quickly interpret, much like handheld vein finders that swiftly locate veins to expedite IV insertions. Cross-reference reviews and case studies to find devices validated for accuracy, durability, and patient comfort.
Establish Proper Placement Protocols
Carefully apply patches on areas most susceptible to pressure sores—such as sacrum, heels, and elbows—ensuring secure attachment to prevent false alarms. During my project, I used transparent medical tape and monitored the patches over several shifts, adjusting placement as needed. Consistent placement ensures sensor contact and reliable readings. This step is crucial, as improper adhesion can lead to missed early signs, much like a poorly fitted glove hampers grip.
Implement Real-Time Data Monitoring
Set up a centralized dashboard allowing caregivers to view sensor data continuously. Use software that highlights abnormal readings, similar to how spectral x-rays reveal soft tissue damage or how smart thermometers sync with patient charts to show temperature spikes. During a pilot, alerts about slight redness changes prompted early repositioning of patients, preventing wound progression. Training staff to interpret these alerts reduces reliance on subjective visual checks, especially during night shifts or low staffing.
Integrate Alerts into Workflow
Develop straightforward protocols so that when a high-risk patient triggers an alert, staff are directed to examine the area promptly and adjust repositioning schedules. Just as powered centrifuges operate quietly yet effectively, the system should work seamlessly without adding complexity to daily routines. I remember setting up rapid response procedures for alarm triggers; initially messy, but integration improved turnaround times in pressure sore prevention.
Train Staff and Maintain Devices
Conduct targeted training sessions emphasizing proper patch application, interpreting alerts, and responding swiftly. Periodically check device integrity to prevent false negatives, much like how new LED curing lights require calibration for optimal dental restorations. During my implementation, staff feedback helped refine protocols, leading to fewer missed warnings and better patient outcomes.
Document and Review Data Regularly
Maintain logs of sensor readings and interventions to track effectiveness and identify patterns. Regular review sessions can reveal high-risk periods or locations, enabling preemptive measures. Think of this as continuous monitoring of blood pressure cuffs—over time, data reveals trends enabling proactive care.
By systematically deploying and managing these smart patches, your facility can shift from reactive to proactive pressure ulcer prevention, improving patient safety and reducing costs associated with advanced wound care. Integrating these devices into your existing protocols is a strategic move—not just adopting technology but reshaping care standards for better outcomes.
Many assume that choosing the latest medical device or equipment guarantees optimal patient care, but in reality, there’s a complex web of nuances that most people overlook. A common myth is that newer technology always outperforms older, proven tools; however, in some cases, familiarity and stability are more crucial than innovation. For example, fresh entrants like cutting-edge ventilators or imaging systems might boast impressive specs but can lack the reliability of established models, especially if they’re not thoroughly tested in diverse clinical settings. In fact, over-reliance on shiny new gadgets without proper validation can introduce unforeseen risks, such as calibration errors or incompatibility with existing workflows, which could compromise patient safety. A striking instance is the misconception that the most expensive devices provide the best care—cost does not always correlate with efficacy. Experts recommend evaluating devices based on real-world performance data, regulatory approval status, and adaptability to specific clinical environments. Equipments like lab mixers or imaging tools should be scrutinized for their proven contribution to workflow efficiency and diagnostic accuracy rather than solely their features or brand prestige. Moreover, the improper handling or maintenance of medical supplies can negate their benefits; for instance, using sterilization units without understanding their proper calibration can lead to ineffective sterilization cycles, risking infection control lapses. This highlights an important oversight: assuming that all devices are maintenance-free or self-sustaining is a trap many fall into, which can later manifest as costly repairs or compromised patient safety. To dig deeper, consider the advanced sensors embedded in many modern devices—they may perform excellently in controlled conditions but struggle in real-world scenarios with variable environmental factors or user errors. Studies show that integrating smart technology requires comprehensive staff training and periodic validation to maintain accuracy, an often-neglected step. Therefore, understanding the nuanced differences between various models, their limitations, and contextual suitability is vital for making informed purchasing and operational decisions. It’s not just about having state-of-the-art equipment but ensuring it’s appropriate, correctly used, and properly maintained for your specific setting. This meticulous approach can significantly improve diagnostic precision, reduce operational costs, and enhance patient outcomes. Remember, a well-chosen device deployed with knowledge and care can outperform a new gadget used blindly. As you refine your strategies, avoid the trap of assuming technology alone solves all problems; instead, combine it with expertise, maintenance, and context-awareness. Have you ever fallen into this trap? Let me know in the comments.
Invest in Reliable Equipment for Consistent Results
Choosing dependable tools is crucial for sustained performance. For example, I personally prefer the latest benchtop mixers designed to optimize lab space and ensure accuracy over time. These devices are built with durability in mind, reducing the need for frequent replacements and minimizing downtime.
Implement Routine Maintenance Protocols
Establish clear schedules for calibrating, cleaning, and inspecting your equipment. Regular checks prevent minor issues from escalating into major failures. For instance, I recommend setting bi-weekly calibration routines for sensitive sensors, which helps maintain accuracy and prolongs device lifespan. Referencing the expert advice from technical documentation, proper maintenance directly correlates with device longevity and reliable operation.
Automate Data Logging and Alerts
Use software solutions that automatically record usage data and notify you of potential issues. Automated alerts for factors like temperature deviations or unusual sensor readings allow for proactive interventions. For example, integrating a smart thermometer system that syncs with your patient records simplifies long-term monitoring and reduces manual errors.
Choose the Right Tools for Maintenance
Having the proper cleaning and calibration kits on hand makes a significant difference. Personally, I rely on high-quality gloves and sterilization supplies that ensure both safety and cleanliness. These tools help prevent contamination and equipment degradation, especially in high-use settings.
Predict Future Trends and Prepare Accordingly
The future of medical equipment maintenance leans heavily towards AI-driven diagnostics and IoT integration. Devices will soon self-report their status, similar to the way smart masks monitor vital signs. Preparing now by adopting compatible systems will make scaling easier and reduce long-term costs.
How Do You Maintain Medical Devices Over Time?
Establishing a comprehensive maintenance plan that includes routine calibration, regular cleaning, and software updates is vital. Consider leveraging IoT-enabled tools that provide real-time diagnostics, so you can address issues before they impact patient care. For instance, integrating predictive maintenance software has remarkably reduced unexpected device failures in my practice. If you’ve yet to try proactive maintenance, I highly recommend it—start with scheduling regular calibration checks for high-risk devices, like the lead-free x-ray aprons.
Lessons from My Time in the Trenches of Medical Equipment
One profound lesson I learned is that even the most advanced device isn’t infallible without proper maintenance and staff training. I once relied solely on high-tech sensors for pressure ulcer detection, only to find that minor calibration oversights could lead to missed early signs. This experience taught me that technology is only as good as the humans operating it, emphasizing the importance of ongoing education and vigilance.
Another realization was that innovation often surprises us with unexpected challenges. When integrating smart skin patches, I encountered resistance from staff unfamiliar with interpreting nuanced data. It became clear that introducing new devices demands a cultural shift within healthcare teams, blending tech with practical workflows for maximum benefit.
Lastly, I discovered that sometimes, simplifying processes enhances reliability. Overcomplicating monitoring protocols can lead to confusion and errors. Striking a balance between technological sophistication and straightforward procedures ensures devices serve as effective, trustworthy tools in patient care.

This post really highlights the importance of integrating technology into patient care, especially for issues like bedsores that can be so subtle initially. I recall working in a rehab center where staff were overburdened, and early signs often got overlooked. Since adopting smart monitoring patches, we’ve seen a significant improvement in early detection, allowing for timely interventions that prevent further tissue damage. The challenge, however, remains in ensuring consistent application and staff training. Do others have experiences with integrating these devices into busy hospital routines without creating additional burdens? I’ve found that dedicated training sessions and clear protocols make a big difference in seamless adoption. Also, it’s interesting to consider how these devices could evolve with AI to predict pressure injury risks proactively rather than just alerting us after early signs appear. What innovations do you see on the horizon that could further enhance pressure ulcer prevention? This proactive approach definitely seems to be the future of patient safety.