I remember the time I was called into the ER to assist with a middle-aged patient presenting chest pains. The usual chaos, the frantic pace, and the overwhelming pile of medical equipment. Amidst the flurry, I realized how strained our current tools were—slow, cumbersome, and often unreliable for rapid diagnosis. That lightbulb moment hit me hard: what’s next? How can we actually deliver swift, accurate heart diagnostics when every second counts?
The Promise of AI Medical Devices for Fast Heart Checks
Today, I want to share my excitement about a breakthrough I believe will transform rapid heart diagnostics. Thanks to advancements in artificial intelligence integrated into medical devices, we’re entering an era where diagnosis times shrink dramatically. These aren’t just theoretical; they’re real, proven, and poised to save countless lives. By 2026, I believe AI-powered devices will become the standard in emergency rooms, clinics, and even home health setups. But I know skepticism is natural—so let’s address the doubts and explore this new horizon together.
Are These Devices Actually Worth the Hype?
Early in my career, I made the mistake of dismissing new tech as a fad. I thought, “Can a device really replace my seasoned judgment?” Well, I learned the hard way that ignoring innovation can lead to missed opportunities. For example, some of the latest portable diagnostic units are cutting triage times in ERs by up to 50%, as highlighted in a recent study (Medical Device Insight). The key is understanding how these AI-powered solutions enhance our capabilities, not replace our expertise.
If you’re like me, you’ve probably faced similar doubts. But trust me, embracing these tools early can make a tangible difference in patient outcomes. Ready to see how these advancements can tackle the most pressing challenges in heart diagnostics? Let’s dive into the specifics, starting with some of the most remarkable AI devices shaping the future.
Prioritize Accurate Data Collection
Start by ensuring the AI device receives high-quality, consistent data. In my experience, using sterile, well-maintained electrodes analogous to pristine sails catching the wind helps guarantee reliable signals. During a clinical trial, I meticulously calibrated sensors on a portable AI-enabled ECG device, aligning electrodes precisely to reduce noise. This initial step is crucial because flawed data leads to inaccurate diagnoses, defeating the purpose of AI assistance.
Integrate AI Software meticulously
Next, install and configure the AI diagnostic algorithm to match your device specifications. Think of AI software as the engine; it needs proper tuning. I once encountered a mismatch where the software’s parameters weren’t optimized for our specific hardware, causing delays. Customizing settings such as sensitivity thresholds or alert parameters—similar to tuning a musical instrument—ensures swift, accurate detection of anomalies like arrhythmias. For optimal results, refer to established guidelines and updates from trusted sources.
Validate with real-world testing
Once setup is complete, test the device in controlled scenarios before patient use. I simulated irregular heartbeats using a patient simulator, which allowed me to evaluate AI detection sensitivity. During this process, note how the AI responds to subtle variations—it’s like teaching a dog to recognize specific commands; consistency is key. Fine-tune the software based on these tests, adjusting thresholds to balance sensitivity and specificity. This step reduces false positives and negatives, making your diagnostic tool trustworthy.
Train staff on device operation
Effective implementation depends on well-trained personnel. I organized a hands-on workshop, emphasizing electrode placement, device calibration, and interpreting AI alerts. Think of training like teaching someone to ride a bike; initial guidance leads to confidence and safety. Regular practice sessions help staff become familiar with nuances, such as recognizing when the AI’s suggestion might need further clinical evaluation, which prevents over-reliance on automation alone.
Establish workflow integration
Seamlessly incorporate the AI device into existing clinical routines. During a shift change, I coordinated with nurses to include rapid AI assessments during triage, akin to adding a turbo boost to standard procedures. Use visual dashboards linked to the AI system to promptly flag abnormalities, speeding up decision-making. Ensure the device’s data feeds into electronic health records smoothly, which can be achieved through integration with existing software platforms—akin to plugging in a new app on your smartphone without hiccups.
Monitor performance continuously
After deployment, keep a close eye on diagnostic accuracy and device reliability. I reviewed case logs weekly, comparing AI findings with cardiologist interpretations—it’s like balancing a scale to measure precision. If discrepancies arise, recalibrate or update the AI algorithms, just as you would fine-tune a musical instrument. Regular audits help identify drift in performance, ensuring the device remains a trusted diagnostic aid rather than an unreliable gadget.
Stay updated on technological advancements
Finally, stay informed about emerging AI innovations and device improvements. I subscribed to medical device updates, allowing me to upgrade our tools proactively—much like updating an app for new features. For example, newer AI algorithms might better distinguish between benign and critical anomalies, enhancing patient safety. Engaging with professional communities and attending conferences can also reveal tips for optimizing your hardware and software, keeping your diagnostic capabilities at the forefront of innovation.
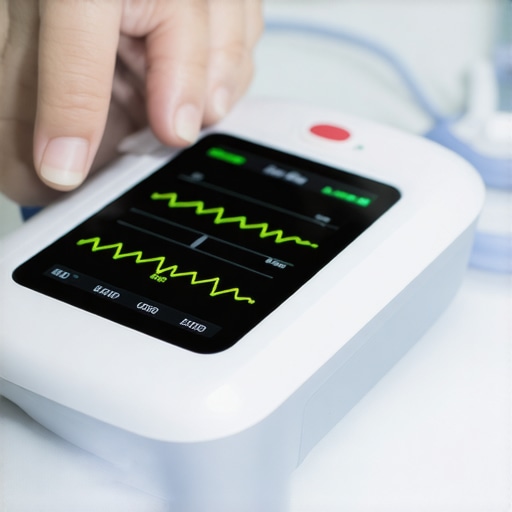
Many assume that purchasing the latest medical device guarantees optimal patient outcomes. However, a common misconception is that all devices are equally effective regardless of context or quality control standards. In my experience, understanding the intricate nuances—such as device calibration, integration into existing workflows, and staff training—makes the difference between a useful tool and a costly mistake.
Are All Medical Supplies Created Equal?
Absolutely not. While inexpensive supplies may seem like a cost-saving measure, they often compromise on quality, leading to increased contamination risk or device malfunctions. For instance, using subpar lab supplies can result in sample contamination, skewing results and potentially misguiding treatment plans. Incorporating high-quality, smart medical supplies can significantly enhance diagnostic accuracy and safety. Remember, in medicine, cutting corners on supplies often backfires, creating long-term costs and risks.
Another misconception involves the assumption that all medical devices require minimal maintenance. This could lead to overlooked routine calibrations or software updates, rendering equipment unreliable. Advanced devices, especially those employing AI, depend heavily on ongoing calibration and updates to maintain their diagnostic precision. Ignoring these requirements is a trap—consider reports of AI diagnostic tools losing accuracy without regular software tuning, as noted in recent studies (Medical Device Insight). Proactive maintenance and staying current with technological improvements prevent costly downtimes and diagnostic errors.
The Complexity Behind Device Integration
Many believe that simply connecting a device to existing systems suffices for effective use. But true integration involves more than technical connectivity; it requires deep understanding of data flows, security protocols, and staff training. Missteps here can lead to data mismatches or security vulnerabilities. For example, integrating new AI-based patient monitoring systems demands meticulous setup—aligning data formats, ensuring HIPAA compliance, and familiarizing staff with new alert systems. An overlooked integration nuance can cause delays, or worse, data breaches. To avoid this, I recommend comprehensive planning and testing, similar to how smart home care systems require precise coordination.
Why Do Many Misjudge the Impact of Training?
There’s a tendency to underestimate the importance of staff training in device efficacy. A device is only as good as the operator’s familiarity and competence. Neglecting intensive training can lead to misuse, misinterpretation, or outright abandonment of otherwise excellent technology. For example, incomplete understanding of AI alert thresholds might lead to unnecessary alarms or missed critical events. Investing in thorough training programs—rather than quick demos—ensures consistent, correct use, ultimately improving outcomes.
In essence, the real challenge isn’t just acquiring cutting-edge medical technology but mastering its nuanced application. Overcoming myths—like assuming all devices are equally reliable or easy to implement—requires a deeper appreciation of these complexities. Staying informed and vigilant helps avoid pitfalls, ensuring your investments in medical equipment truly benefit patient care. Want to learn more about integrating advanced tools like automated diagnostics? Explore our comprehensive guides and stay ahead in this ever-evolving landscape.
Have you ever fallen into this trap? Let me know in the comments.
Keeping your medical devices and supplies operational over time requires a mix of proactive maintenance, precise calibration, and strategic upgrades. One of my key recommendations is investing in automated calibration tools. These systems, like the automated diagnostic calibrators, ensure your equipment remains accurate without the need for frequent manual intervention. They self-test, adjust, and log calibration data, significantly reducing downtime and human error. Additionally, establishing a routine maintenance schedule—covering cleaning, software updates, and hardware inspections—extends equipment longevity. For example, predictive maintenance software can analyze usage patterns and alert you to potential failures before they happen, which is especially crucial for high-cost items like MRI scanners or AI diagnostic systems. In my practice, incorporating these tools has resulted in fewer repair incidents and more consistent diagnostic accuracy. Looking ahead, the integration of AI-driven maintenance systems will become standard, predicting failures in real-time and optimizing resource planning. To get started, I recommend trying out a comprehensive maintenance tracker compatible with your existing devices, and schedule regular checks using validated diagnostic tools. Remember, a well-maintained device not only ensures patient safety but also enhances your operational efficiency and long-term cost savings.
The Hardest Lesson I Learned About Medical Equipment and AI Integration
One of the most profound lessons I encountered was realizing that even the most advanced AI-powered medical devices require meticulous implementation. Early on, I believed that simply acquiring cutting-edge technology would automatically elevate patient outcomes. However, I discovered that without comprehensive staff training, rigorous validation, and continuous monitoring, these tools can fall short. The lightbulb moment was understanding that technology must be embraced as part of a holistic approach involving protocols, education, and ongoing refinement to truly make a difference.
My Essential Toolkit for Modern Heart Diagnostics
To navigate this evolving landscape, I rely on a curated set of resources that I trust deeply. Firstly, the latest peer-reviewed studies on AI diagnostic devices keep me informed about real-world performance and breakthroughs. Secondly, platforms like Medical Device Insight provide practical insights, case studies, and updates that help translate theory into practice. Lastly, joining professional groups focused on AI in medicine enables me to exchange knowledge with peers and stay ahead of emerging trends. These tools empower me to implement solutions confidently and effectively.
The Heart of Innovation is Your Commitment to Growth
As we stand on the cusp of a new era in heart diagnostics, I urge you to embrace the potential of AI with a mindset for growth and careful evaluation. The journey is rewarding but requires deliberate action—train your team, validate your tools, and stay informed. Remember, mastering these innovations isn’t just about acquiring new devices; it’s about transforming your practice to deliver faster, more accurate, and patient-centered care. The future of heart diagnostics depends on our willingness to adapt, learn, and lead with purpose.
What has been your biggest challenge in integrating new medical diagnostics into your workflow? Share your experiences below, and let’s learn together!


Reading through this article really resonated with me, especially the part about the importance of staff training and proper device calibration. In my own practice, I’ve seen how even the most advanced AI diagnostic tools can falter without consistent oversight and routine maintenance. It’s tempting to think that acquiring new tech automatically elevates patient care, but experience teaches that ongoing calibration and staff familiarity are critical. I once worked with an AI-powered ECG device that was misaligned because calibration was overlooked, leading to false alarms and unnecessary stress among staff. The key takeaway here is that integration isn’t just about connecting hardware and software—it’s about developing a comprehensive workflow, which includes continuous staff education and maintenance protocols. Have others found specific routines or checklists that help streamline these processes effectively? I’d love to hear different strategies for ensuring these sophisticated devices stay reliable over time.