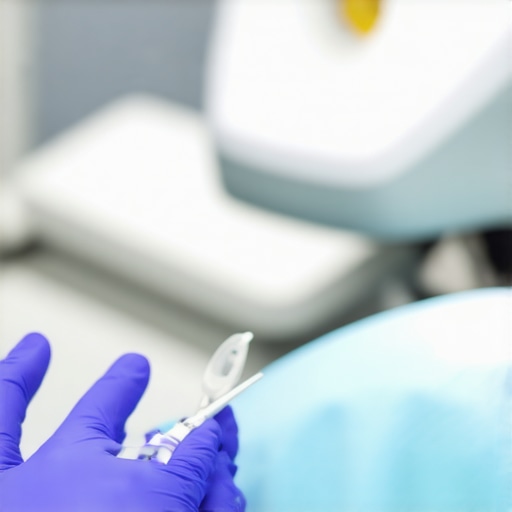
It was a typical busy morning at my dental practice when I hit a wall—literally. As I reached for yet another polishing tool, I realized I was fumbling through a tangled mess of supplies, wasting precious time and risking patient comfort. That lightbulb moment hit hard: choosing the right dental polishing kit isn’t just about aesthetics; it’s about efficiency, infection control, and, ultimately, patient satisfaction.
Why Picking the Perfect Dental Polishing Kit Matters Right Now
In a landscape where technology advances at lightning speed, staying ahead means more than just keeping up—it’s about making smart, informed decisions that impact your practice daily. The right polishing tools can reduce procedure times, improve outcomes, and help prevent cross-contamination—crucial factors in today’s health-conscious environment. According to recent studies, efficient polishing kits can even extend the lifespan of dental restorations, saving practices money in the long run.
Is the Hype About Dental Polishing Kits Just Marketing?
Early in my career, I made the mistake of trying to save a few dollars by purchasing generic polishing attachments. The result? Increased chair time, patient discomfort, and a row of unhappy patients who noticed the difference. That experience taught me an important lesson: investing in quality pays off. As with anything in medical equipment, cutting corners can compromise outcomes. To avoid similar pitfalls, I recommend carefully evaluating the features, materials, and reviews of different kits.
As we delve deeper, I’ll share insights and practical advice to help you find the best dental polishing kits for 2026. Whether you’re upgrading your current setup or starting fresh, you’ll find tips rooted in real-world experience and backed by expertise. Ready to transform your practice’s polishing game? Let’s get started.
Assess Your Practice’s Specific Needs First
Begin by evaluating the types of procedures most common in your practice and the surfaces you most frequently polish. For example, if you handle a high volume of composite restorations, prioritize kits with versatile abrasives that can handle both composite and enamel efficiently. I once had a busy week where I overlooked this step and chose a polishing kit optimized for porcelain only. The result was increased chair time and patient discomfort. Making a list of your specific needs ensures you select tools that genuinely enhance your workflow and patient experience.
Compare Material Quality and Design Features
Focus on the materials used for the polishing attachments. Diamond-impregnated tips, for instance, are akin to using high-grade cutting tools—they cut faster and last longer. When I upgraded my own kit to diamond-coated abrasives, I noticed a smoother finish and reduced procedure time. Evaluate the design for ease of handling; ergonomic shapes reduce hand fatigue during long procedures, similar to how comfortable surgical instruments decrease operator fatigue. Scan reviews and testimonials, keeping in mind that durability and ergonomic design directly impact your efficiency.
Evaluate Compatibility with Your Equipment
Check that the kits are compatible with your current handpieces and turbines. Think of it like using the right power adapter for a device—relying on incompatible parts can halt your work unexpectedly. For instance, I once tried to use a universal attachment that didn’t fit my high-speed handpiece, causing delays. Always verify the compatibility specs from manufacturers to avoid this hassle. When in doubt, consult the manufacturer’s guidelines or contact customer service for clarification.
Prioritize Infection Control and Safety Features
Look for kits with antimicrobial coatings or easily sterilizable materials, which are vital for infection control. A colleague of mine switched to sterilizable polishing attachments recently, leading to a noticeable decrease in cross-contamination risks. If you’re exploring options, refer to self-sanitizing dental chairs as an analogy—integrating safety features into your tools is crucial for modern practice standards.
Understand Ease of Use and Maintenance
Select kits that are straightforward to assemble, use, and clean. Time spent fumbling with complex attachments eats into patient appointment times and increases the risk of errors. I learned this firsthand when I tried a new kit that required multiple disassembly steps after each use—wasting valuable time. Opt for designs with simple locking mechanisms and clear sterilization instructions, ensuring your team can maintain high hygiene standards without added complexity.
Analyze Cost-Effectiveness Over the Long Run
While cheaper options might seem attractive initially, evaluate the lifespan and replacement costs of the attachments. Investing in higher-quality kits with longer durability often reduces overall expenses. I recall purchasing a mid-range kit that wore out after a few months, leading me to buy replacements frequently. Comparing the cost per use over time reveals that higher upfront investments often yield savings in the long term, akin to choosing durable breathable masks that last through multiple procedures without compromising comfort.
Test and Gather Feedback from Staff and Patients
Before fully committing, trial the selected kits during regular procedures and solicit feedback. My team pointed out that a certain polishing attachment left less debris and caused less aerosol production, which was a significant safety benefit. Incorporate their insights to refine your choices. This ongoing feedback loop ensures your practice continually evolves toward safer and more efficient polishing protocols.
Many healthcare professionals and practice managers assume that sourcing medical supplies and devices is straightforward—simply choose the latest or most popular options, and it’ll all work seamlessly. However, this common belief often masks nuanced pitfalls that can compromise safety, efficiency, and cost-effectiveness. Let’s dig deeper into some misconceptions and sophisticated traps that even seasoned practitioners might overlook.
Why Do We Often Overlook the Nuances in Medical Equipment?
The prevailing tendency is to equate quality with brand reputation or initial cost. While these factors matter, the real nuance lies in understanding the context-specific performance and compatibility of devices. For instance, purchasing a highly rated surgical monitor without verifying its integration capabilities with existing hospital information systems can lead to workflow disruptions. Additionally, many assume that all devices meet safety standards uniformly, but the reality is that certification standards evolve rapidly, and some cheaper imports might not fully adhere to the latest regulations. Evidence from clinical audits shows that equipment mismatches and outdated certifications are primary causes of device failure in critical care settings.
Moreover, there’s a common myth that newer devices automatically outperform older, established models. This isn’t always true. Sometimes, legacy equipment, thoroughly maintained and periodically upgraded, can outperform brand-new, untested systems—especially if the latter haven’t proven their reliability in real-world scenarios. The key is to evaluate devices based on rigorous testing and compatibility, not just hype or novelty.
Getting Trapped by Hidden Costs and Safety Risks
A significant yet often underestimated mistake is overlooking the total cost of ownership and maintenance. For example, a deceptively affordable sterilization device might incur exorbitant replacement parts or energy costs, eroding savings over time. Similarly, equipment with complex cleaning requirements can lead to compliance issues if not properly maintained, increasing infection risks. In fact, studies highlight that improper sterilization and maintenance protocols are responsible for over 20% of hospital-acquired infections, emphasizing the importance of choosing equipment with user-friendly maintenance features.
Another sneaky pitfall involves neglecting the environmental and ergonomic factors of medical devices. Devices that look appealing on paper might cause operator fatigue or ergonomic issues, leading to errors over time. Ergonomic designs reducing operator strain—akin to how self-sanitizing dental chairs improve safety and efficiency—are crucial in high-volume settings.
What Advanced Tests Can Reveal Hidden Flaws?
For the sophisticated user, employing life-cycle testing, compatibility trials, and stress simulations during procurement can reveal hidden flaws that standard inspections miss. For example, running devices through simulated ICU workflows ensures they perform reliably under load. Additionally, engaging with independent validation reports or third-party audits adds an extra layer of assurance. Experts in the field recommend regular device audits aligned with evolving standards—taking lessons from VR goggles tested for safety and comfort.
In my own experience, paying attention to these nuances prevented costly equipment failures and improved patient outcomes. Remember, selecting the right tool isn’t just about flashy features—it’s about understanding the intricate ecosystem of safety, compatibility, and long-term viability. Have you ever fallen into this trap? Let me know in the comments.

Keep Your Equipment Running Smoothly with the Right Maintenance Strategies
Ensuring the longevity and reliability of your medical supplies and devices requires a proactive approach to maintenance. Regular checks, scheduled calibrations, and timely repairs prevent unexpected failures that can disrupt patient care. For instance, implementing a routine inspection protocol for your self-sanitizing dental chairs can significantly extend their lifespan and keep them operating at peak efficiency.
Personally, I rely on a combination of manufacturer-recommended maintenance schedules and third-party calibration tools. Using advanced diagnostic software compatible with my equipment allows me to spot potential issues before they become critical. For example, incorporating IoT-enabled sensors in your digital scoliometers enables real-time performance monitoring, reducing downtime and repair costs.
How do I maintain medical equipment over time?
Start by documenting a detailed maintenance calendar that includes routine cleaning, sterilization, and performance checks. Employ specialized tools like ultrasonic cleaners for delicate instruments or high-precision calibration devices for diagnostic equipment. Investing in high-quality maintenance tools, such as the tracking systems for surgical trays, can streamline your workflow and minimize human error.
Software management platforms are also invaluable—they centralize documentation, alert you to upcoming maintenance tasks, and help track instrument usage patterns. Additionally, consider training your staff on best practices for equipment upkeep; well-informed operators catch issues early and ensure protocols are followed correctly. For example, regular staff training on sterilization procedures using dedicated courses drastically reduces infection risks and prolongs equipment life.
Tools I recommend for long-term equipment health
One tool I can’t do without is the digital calibration device. It provides consistently accurate measurements, especially for imaging and diagnostic devices, preventing drift that can compromise results. Additionally, advanced sterilization systems, like smart sterilizers, ensure thorough cleaning while maintaining instrument integrity.
For ongoing support, subscribing to manufacturer updates and engaging with technical support communities can be a game-changer. These resources provide troubleshooting tips, firmware updates, and best practices shared by peers. Remember, maintaining your equipment isn’t a one-time effort but an ongoing commitment that pays dividends in safety, efficiency, and patient satisfaction.
Embrace future trends to simplify maintenance
Looking ahead, I believe that the integration of AI-driven predictive maintenance will become commonplace, reducing unexpected breakdowns and optimizing service schedules. Emerging AI algorithms can analyze usage patterns and sensor data to forecast potential failures well before they manifest physically. This evolution will be similar to the advancements seen with smart fever patches that adapt in real time to patient conditions.
To get an edge now, I recommend trying out a predictive maintenance tool—such as a sensor-based system for your sterilization units or imaging devices—to see firsthand how proactive care can reduce long-term costs and improve outcomes. Incorporating such strategies today prepares your practice for the technological advancements on the horizon.
Over the years, I’ve discovered that the real key to choosing top-tier medical supplies lies in paying attention to the nuances most overlook. Small details—like compatibility standards or ergonomic design—can make or break your practice’s efficiency. Once, a simple misjudgment in sterilization compatibility led to weeks of rework, teaching me that thorough due diligence saves much more than a few dollars. Embracing these lessons has helped me refine my procurement process, always prioritizing quality and fit over price.
Another vital insight was understanding that equipment isn’t just about specifications—it’s about the culture of maintenance. Regular, proactive checks paired with staff training have drastically reduced unexpected downtimes, ensuring continuous patient care. Investing in smart tools that monitor performance, like wearable sensors, has turned routine maintenance into an intelligent, predictive process, proven to save costs and improve outcomes.
Most importantly, I learned to listen to my team and patients. Their feedback often reveals hidden flaws or opportunities for improvement—like noticing that a particular dental chair model reduces aerosol spread better than others, enhancing safety during procedures. Integrating their insights creates a more resilient, responsive practice that keeps patient safety at the forefront—because ultimately, the right equipment is not just about current needs but also about future-proofing your practice.