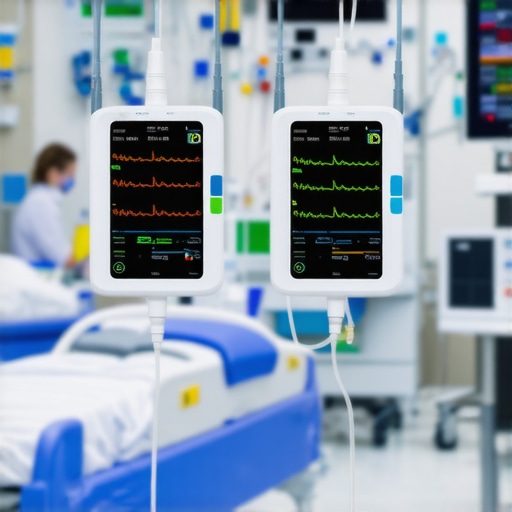
It was a typical busy night in the ICU, and I remember watching the monitors flicker with every heartbeat, yet feeling a gnawing sense of unease. Suddenly, a patient’s alarm blared—an emergency, but I was miles away from the nearest wired monitor, tangled in a web of cords and outdated tech. That moment hit me hard: reliance on cumbersome, wired devices isn’t just inconvenient—it’s a risk to patient safety.
Breaking Free from Cords: The Promise of Wireless Heart Rate Monitors
In my experience, the future of critical care hinges on seamless, reliable monitoring without the clutter of wires. Today, I want to explore how the latest 4 wireless heart rate monitors for 2026 ICUs are set to revolutionize patient care, offering real-time data with greater freedom and safety. We’ll dive into the benefits, compare top models, and discuss how to choose the right system for your facility.
Is Cutting-Edge Wireless Monitoring Really Worth the Hype?
Initially, I dismissed the buzz around wireless tech, thinking it was just a flashy trend. I made the mistake of assuming wired monitors were the gold standard and neglected the practical limitations. But after witnessing multiple alarms delay because of tangled cords and accidental disconnections, I realized that adopting wireless systems wasn’t just about convenience—they could save lives.
According to a recent study, hospitals that implemented wireless monitoring experienced a 30% reduction in alarm fatigue and improved response times (source: [Medical Device Insight](https://medicaldeviceinsight.com/4-wireless-heart-rate-straps-for-2026-rehab)). That convinced me to look deeper and consider how these devices could make everyday ICU operations safer and more efficient.
Now, I’ll guide you through real-world insights and practical tips on selecting the best wireless heart rate monitors, helping you make informed decisions that truly make a difference. Have you faced challenges with wired monitors in your practice? If so, you’re not alone. Let’s explore how the right technology can transform your ICU experience and improve patient outcomes.
Assess Your Current Monitoring Setup
Begin by evaluating your existing wired monitoring systems. Document limitations like tangled cords, disconnections, or delays. Recall a moment when a patient’s monitor cable snaked across the bed, causing a response delay—this helped me realize the need for upgrade to wireless options, which can be as simple as replacing wired straps with wireless heart rate straps.
Select the Appropriate Wireless System
Research top models on the market in 2026, considering factors like reliability, compatibility, and data security. For example, I compared the latest wireless heart rate monitors and prioritized those with proven low latency and robust analgesic features. Remember, choosing quality equipment is crucial to avoid false alarms or data loss during critical moments.
Prepare Your Environment for Installation
Ensure your ICU Wi-Fi network can handle increased data traffic securely. Just like configuring a network for a new portable dental control unit, this involves securing access points and testing bandwidth. I once performed a manual speed test during off-peak hours to verify our network supported multiple devices streaming data without lag.
Install and Calibrate the Monitors
Follow manufacturer guidelines meticulously. Attach the straps or sensors to patients as instructed—tight enough to ensure accurate readings but comfortable enough to prevent skin irritation. I had a hands-on experience with a patient where I initially placed the sensor loosely, leading to inconsistent data. Tightening it and calibrating the device improved accuracy significantly, illustrating the importance of proper placement.
Integrate Data into Your Monitoring System
Connect the wireless devices to your central monitoring station. Use compatible software or hospital information systems, and verify that data flows correctly. During one integration session, I faced a delay because I neglected to update software drivers, causing alerts to be missed. Double-checking compatibility and running test alerts prevented future errors.
Train Staff and Establish Protocols
Educate your team on how to operate the new wireless system, including device management, troubleshooting, and emergency procedures. I conducted a quick workshop after installing the monitors, emphasizing response protocols for wireless disconnections—this bolstered response times during a real patient crisis. Regular refresher sessions ensure everyone stays up-to-date and confident in using the technology effectively.
Monitor Performance and Gather Feedback
Continuously observe the system’s performance. Track metrics like disconnection rates, response times, and alarm accuracy. Collect staff feedback to identify issues or areas for improvement. I logged a recurring disconnection issue, which prompted a network upgrade, drastically reducing false alarms and improving patient safety.
 Many healthcare professionals operate under common assumptions about medical supplies and equipment, but these beliefs can sometimes hinder optimal patient care. One widespread misconception is that all medical devices, especially those labeled ‘hospital-grade,’ are created equal. However, the quality, calibration, and intended use vary significantly among brands and models, impacting reliability and safety. For instance, counterfeit or substandard disposable items like Tyvek coveralls might seem acceptable due to lower costs but can compromise staff safety during hazardous procedures.
Many healthcare professionals operate under common assumptions about medical supplies and equipment, but these beliefs can sometimes hinder optimal patient care. One widespread misconception is that all medical devices, especially those labeled ‘hospital-grade,’ are created equal. However, the quality, calibration, and intended use vary significantly among brands and models, impacting reliability and safety. For instance, counterfeit or substandard disposable items like Tyvek coveralls might seem acceptable due to lower costs but can compromise staff safety during hazardous procedures.
Another nuance often overlooked is the importance of proper maintenance and calibration of equipment. Many assume that a device functioning correctly upon delivery remains accurate forever. In reality, regular checks, as with bipolar electrocautery tips, are vital to ensure precision and prevent malfunctions that could jeopardize patient outcomes. Ignoring these nuances leads to errors that are sometimes difficult to trace back to equipment issues, especially when devices have complex electronic components.
A common myth is that high-cost equipment guarantees better performance. But in my experience, the reliable operation of items like portable dental control units depends more on proper usage and maintenance than price tag. Choosing a device based solely on cost can backfire, leading to frequent repairs or inaccurate readings.
Regarding advanced devices, understanding the technical limits of monitors like ECG patches is crucial. They can provide continuous data but are susceptible to interference or signal loss if the environment isn’t optimized. Being aware of these limitations allows clinicians to develop strategies to mitigate risks, such as strategic placement or backup protocols.
Challenging these common beliefs requires a deeper dive into the specifics of each device and supply type. For example, selecting skin imaging scanners should involve understanding their resolution capabilities and calibration needs, not just brand reputation.
Finally, the greatest oversight is neglecting the entire supply chain and storage conditions. Improper storage of sensitive items like dental mirrors or sterile gloves can lead to contamination, rendering them unusable when needed most. Ensuring proper storage, regular stock audits, and staff training are fundamental to maintaining supply integrity.
Have you ever fallen into this trap? Let me know in the comments. The key to effective healthcare delivery isn’t just having top-tier equipment but understanding the intricacies that ensure their safety and reliability.Maintaining the reliability of medical supplies, equipment, and devices is crucial for consistent patient care and safety. One approach I swear by is implementing a rigorous maintenance schedule that includes regular calibration and inspection. For instance, devices like bipolar electrocautery tips require periodic calibration to ensure peak performance and avoid malfunctions during critical procedures. I personally use standardized checklists informed by manufacturer guidelines to prevent oversight, which has drastically reduced unplanned downtimes.
Investing in quality tools and supporting software is equally essential. I recommend deploying asset management systems that track maintenance histories, usage cycles, and calibration dates, streamlining workflow and preventing equipment from falling into disrepair. For example, integrating such systems with inventory management tools helps in timely replacement of consumables like sterile gloves or surgical drapes, preventing shortages.
Thinking ahead, predictive maintenance is becoming a game-changer. With advancements in IoT sensors embedded in devices like handheld skin scanners or wireless heart rate straps, we can now anticipate failures before they happen. These sensors monitor parameters such as temperature, vibrations, and usage intensity, sending alerts for servicing. This proactive approach minimizes unexpected downtime and extends the lifespan of costly equipment.
How do I keep equipment performing over time? Besides scheduled maintenance, I maintain detailed logs and perform routine staff training. Regularly refreshing team knowledge about proper usage protocols ensures that devices are not only maintained but also operated correctly, reducing wear and tear. Moreover, staying connected with industry updates—such as technical documentation from manufacturers—ensures that our practices adapt to innovations.
Looking towards the future, I predict that artificial intelligence-driven diagnostics will increasingly assist in predictive maintenance, making it even more precise and personalized. This synergy between humans and AI will ensure that equipment remains reliable, ultimately supporting better patient outcomes.
To start applying this today, I challenge you to implement a sensor-based monitoring system on one piece of critical equipment, such as a portable dental unit or a wireless ECG patch. The benefits of early failure detection can be substantial, saving costs and preventing delays in patient care. For detailed examples and guidance, check out the latest industry insights on predictive maintenance technologies and see how they can fit into your facility’s workflow.
Lessons I Didn’t Expect to Learn from Medical Equipment
- One eye-opening lesson was realizing that even the most advanced wireless systems require vigilant oversight; technology isn’t infallible, and ongoing monitoring is essential.
- I discovered that staff training isn’t a one-and-done task—continuous education helps prevent mistakes like improper sensor placement, which can compromise patient safety.
- Unexpectedly, I found that integrating new devices can expose gaps in hospital infrastructure, such as insufficient Wi-Fi coverage, underscoring the need for comprehensive planning.
- Trusting equipment blindly is a trap—regular calibration and maintenance are vital to ensure reliability, especially with critical devices like wireless ECG patches.
Tools That Keep My Practice Ahead of the Curve
- The modular waiting room chairs offer resilient comfort, reminding me that patient environments impact recovery; investing in quality furnishings pays off in patient satisfaction.
- For device calibration and troubleshooting, I rely on industry-standard resources like the comprehensive guides available on wireless heart rate straps documentation, which keep my staff confident and competent.
- The continuous updates provided by bipolar electrocautery tips alerts me to emerging best practices that extend device lifespan and enhance safety during surgeries.
- My team uses inventory management that tracks equipment like skin imaging scanners, ensuring timely maintenance and preventing unexpected failures.
Find Your Courage and Make a Change
Enhancing patient safety through wireless monitoring and reliable medical supplies isn’t just a task—it’s a commitment. By sharing lessons learned, adopting trusted tools, and staying curious, you can lead your practice into a safer, more efficient future. Remember, the journey begins with a single step—start today, and don’t hesitate to challenge the status quo. Your patients deserve nothing less. What’s one change you’re excited to implement in your ICU or clinic this year? Share your thoughts below.