Imagine a busy morning in your lab. You’re rushing to prepare for the day, but chaos reigns. Supplies are scattered, equipment is misplaced, and that crucial sample gets buried under a pile of outdated storage boxes. I’ve been there—frustrated, overwhelmed, and constantly battling the clutter. That lightbulb moment hit me hard: what if I could make my storage smarter, more efficient, and future-proof? Turns out, the solution was right within reach—4 Smart Lab Storage Cabinets for 2026 Labs could revolutionize how we manage our resources.
Why Settling for Old Storage Methods Just Doesn’t Cut It
Traditional cabinets are the backbone of most labs, but let’s be honest—are they really designed for the demands of modern research? When I started transitioning to smarter solutions, I realized how much time and effort I was wasting hunting down supplies or untangling misplaced equipment. This inefficiency affects productivity and can even compromise safety. The good news? The emergence of smart lab storage is changing the game, paving the way for faster, safer, and more organized labs.
Are Smart Cabinets Worth the Investment?
Many skeptics wonder if investing in these futuristic cabinets is justified—well, I’ve made my share of mistakes early on. I once purchased generic storage units, thinking they’d do the job, but quickly learned they lacked the connectivity and adaptability needed. The key is understanding that these smart cabinets aren’t just high-tech gadgets—they’re strategic assets that streamline workflows and reduce errors. Trust me, the initial investment pays off when you see how much smoother your operations become and how much time you save each day.
In the next sections, I’ll guide you through selecting the right smart storage solutions tailored for your lab’s specific needs, so you can avoid common pitfalls and truly harness the potential of this technology. Ready to make your lab smarter? Let’s dive deeper.
Select the Right Smart Cabinets for Your Space
Start by assessing your lab’s specific needs; consider the types of samples, equipment, and frequency of access. Think of it as choosing a toolbox: you need compartments for delicate reagents, bulky instruments, and quick-access drawers for frequently used items. When I upgraded my lab, I measured all storage areas and listed critical items to determine cabinet dimensions and features. Research smart lab solutions that offer modular designs and integrated inventory management, which made customization straightforward.
Install and Configure Your Cabinets Properly
Proper placement is crucial—for example, keeping frequently used supplies near workbenches minimizes movement. When installing, level the units carefully; an uneven cabinet is like a wobbly cart, risking spills and damage. I once fumbled through setup, but following manufacturer’s instructions and using a level tool created a stable base. Make sure to connect the cabinets to your network if they are IoT-enabled. Setting up automated alerts for low stock increases efficiency; I configured mine to notify me when reagent levels dropped below threshold, saving hours hunting for replacements.
Organize Supplies with Precision and Logic
Use logical groupings: store all PCR reagents together, separate biological samples from chemical supplies, and label everything clearly. Think of it as organizing jewelry by type—rings, necklaces, bracelets—so you can find items instantly. I adopted color-coded labels and categorized drawers, which dramatically reduced retrieval time. Integrate your inventory system with barcode scanning for real-time tracking; this helps prevent shortages and misplaced items. Check out smart inventory solutions that facilitate seamless stock management.
Leverage Data and Automation for Efficiency
Once setup is complete, utilize the data generated by your smart cabinets to optimize storage and ordering cycles. Set parameters for reorder points, analyze usage patterns, and adjust storage configurations accordingly. During my last overhaul, I noticed that certain buffers were rarely used; reallocating those spaces improved access to high-demand items. Some advanced cabinets can even predict consumption trends using AI, like AI-powered skin cancer scanners, enabling proactive stock replenishment. Automating these processes reduces manual oversight and minimizes human error, ensuring your supplies are always ready when needed and your lab runs smoothly.When it comes to medical supplies and equipment, a common misconception is that more advanced or expensive tools always lead to better patient care and operational efficiency. However, as an experienced professional in the field, I’ve observed that understanding the nuanced performance and limitations of these products is crucial for truly optimizing healthcare delivery. One widespread myth is that the latest technology automatically integrates seamlessly into existing workflows. In reality, many advanced devices, like AI-powered skin cancer scanners or smart lab incubators, require extensive staff training and infrastructure adjustments before realizing their full potential. Overlooking this can lead to underutilization and wasted investment.
A critical mistake I’ve seen is assuming that high-tech equals high reliability. For instance, some presume that the newest smart blood pressure kits or digital monitors are foolproof, but in practice, calibration issues, software bugs, or inaccurate data transmission can undermine their effectiveness. Regular maintenance, validation, and staff competency are often underestimated components that determine success.
Furthermore, the misconception that compatibility and standardization are secondary concerns can trap even seasoned professionals. Devices sourced from different providers might not align perfectly or could cause interoperability problems, hindering data integration and real-time monitoring. The hidden nuance here involves understanding the importance of choosing equipment that adheres to industry standards—something often overlooked during procurement but vital for long-term operational harmony.
For advanced users pondering the intricacies of equipment performance, it’s worth questioning: How do we accurately assess a device’s real-world reliability beyond marketing claims? Studies reveal that lifecycle testing and third-party validation are key indicators of durability, especially in demanding clinical environments. According to expert analyses, such as those published in the Journal of Medical Device Safety, rigorous validation protocols significantly reduce the risk of equipment failure and safety incidents.
Have you ever fallen into this trap of oversimplifying equipment capabilities? Let me know in the comments. Remember, mastering these hidden nuances ensures your healthcare facility maximizes investments, enhances safety, and improves patient outcomes—that’s the true bottom line.
How do I keep my medical devices running smoothly over time?
Ensuring the continual operation of medical equipment requires a combination of routine maintenance, strategic tool selection, and embracing automation where possible. Personally, I rely heavily on calibration tools like the Smart Blood Pressure Kits for daily checks, which allow me to verify device accuracy without the need for external calibration services every time. Consistent calibration prevents drift in readings, ensuring patient safety and compliance with regulatory standards—something a trusted calibration device is vital for.
Another vital aspect is software management. I recommend deploying remote monitoring platforms such as those integrated with smart lab incubators. These systems keep track of device performance, alerting you instantly if irregularities arise, akin to having a digital watchdog watching over your equipment 24/7. Regular software updates, validated through manufacturer protocols like those outlined by the FDA, are essential to patch vulnerabilities and incorporate improvements for long-term reliability.
Additionally, investing in durable power backup solutions like Uninterruptible Power Supplies (UPS) prevents equipment downtime during outages—something I personally cannot overlook. Pairing UPS systems with surge protectors prolongs device lifespan, reduces repair costs, and minimizes patient risk. For high-stakes equipment like MRI or CT scanners, redundancy plans that include spare units and preventive maintenance schedules—scheduled as per manufacturer recommendations—help avoid unexpected failures. According to the Journal of Clinical Chemistry, implementing predictive maintenance strategies backed by real-time data reduces downtime by up to 30%. Implementing these techniques may seem challenging initially, but they significantly pay off in operational efficiency and patient safety.
Looking ahead, I believe AI-driven predictive maintenance will become the norm, further reducing manual oversight and enhancing device longevity. For now, start by integrating a reliable calibration tool into your routine—it’s a game changer for healthcare providers aiming for excellence. Want to see real-world results? Try using a smart calibration device next week and notice how it simplifies your maintenance cycle.
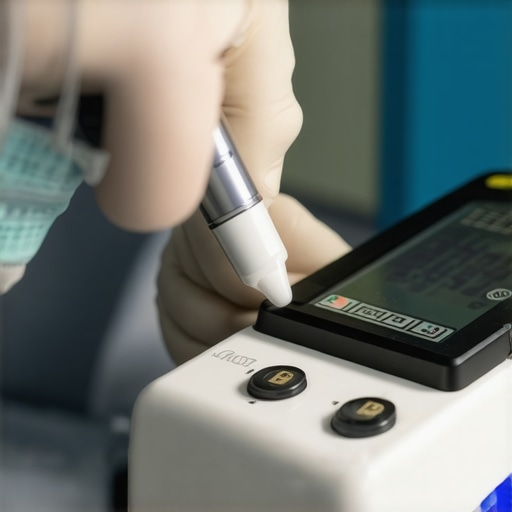
The Hardest Lessons I Learned About Medical Devices and Equipment
One of the most profound realizations I had was that investing in cutting-edge technology isn’t enough; understanding the operational nuances makes all the difference. I once introduced state-of-the-art smart incubators without proper staff training, leading to underutilization and wasted resources. The lesson? Training and ongoing education are just as crucial as the devices themselves.
Beware of Overconfidence in Device Reliability
I learned the hard way that no device is foolproof. Assuming that the newest smart blood pressure kits could operate flawlessly without regular calibration resulted in inaccurate readings and potential patient risks. Regular maintenance and validation are the unsung heroes behind dependable medical equipment—don’t neglect them.
Recognize Interoperability as a Hidden Key to Success
Choosing devices that adhere to industry standards can seem tedious but fundamentally impacts long-term functionality. I once faced interoperability issues with incompatible lab systems, causing data silos and workflow disruptions. Prioritizing standard-compliant equipment streamlines integration and saves headaches down the line.
Questions to Ponder When Upgrading Your Lab
Each new technology brings a set of unique challenges and benefits. Have you considered how a smart lab incubator could specifically optimize your workflows? Or whether integrating continuous data analysis might preempt equipment failures? Reflecting on these questions helps align your purchases with your lab’s real needs.
Curated Tools to Elevate Your Medical Equipment Strategy
For comprehensive device validation and maintenance, I recommend tools like smart blood pressure kits. They provide reliable data, simplifying calibration routines and enhancing accuracy. For staff training, platforms such as smart lab incubators come with intuitive interfaces, making staff onboarding seamless. Additionally, investing in standards-compliant equipment, as discussed in industry reviews, minimizes future compatibility issues, ensuring your lab stays ahead.
Your Next Move Starts Now
The landscape of medical supplies and equipment is evolving rapidly, and staying updated is essential for delivering top-notch care. Embracing smarter tools and understanding their intricacies empowers you to make informed decisions that benefit both your team and your patients. Remember, technology is only as good as the knowledge guiding its use.
What has been your biggest challenge when integrating new medical equipment? Share your experience below, and let’s learn from each other!
**

