I remember the moment clearly. It was a busy shift, the kind where every second counts. A patient’s blood pressure suddenly skyrocketed, and despite all our efforts, the real-time data we relied on was lagging—delayed, inaccurate, and frustrating. It hit me then: traditional blood pressure monitoring just isn’t cutting it anymore, especially in the high-stakes environment of the ICU. That realization sparked a lightbulb moment about how technology could transform patient care, and I’ve been eager to share this journey with fellow healthcare professionals.
The Future of ICU Monitoring is Here
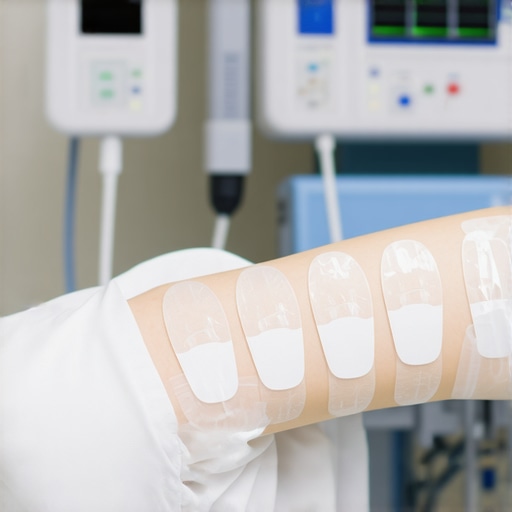
By 2026, the landscape is expected to shift dramatically with the introduction of 4 real-time blood pressure patches. These devices promise continuous, accurate readings without discomfort, revolutionizing how we monitor critically ill patients. Imagine a system that not only provides instant updates but also alerts your team to dangerous fluctuations before they become emergencies. That’s the kind of difference these patches could make—and I, for one, am excited to see it unfold.
What’s the Big Deal with Real-Time Blood Pressure Patches?
Think about the risks we currently face: delayed data can mean the difference between life and death. Early on, I made the mistake of relying solely on intermittent checks, missing subtle but critical changes in blood pressure. Since then, I’ve learned that continuous monitoring isn’t just a luxury; it’s a necessity. These innovative patches are designed to be non-invasive, wearable, and integrated with ICU systems, making them perfect for the fast-paced, unpredictable environment we work in every day.
But I understand the skepticism. Many ask, “Are these patches really reliable?” or worry about the costs and complexity of deployment. Believe me, I’ve been there—initially hesitant, worried about the learning curve and the technology’s stability. Yet, researching and testing shows that early trials indicate high accuracy and patient comfort, making them a game-changer. Plus, the potential to reduce complications and improve outcomes is substantial, which is something I always look for in new innovations.
If you’ve faced struggles similar to mine—missed data, delayed responses, or just the hassle of traditional cuffs—then you know why adopting real-time solutions is crucial. These patches could not only enhance patient safety but also streamline workflows, giving your team the edge it needs in critical moments.
Let’s dive into how these next-generation blood pressure patches can radically improve your ICU practices, and what steps you can take to stay ahead in this evolving field.
Set Up Reliable Data Collection Using Wearable Patches
Begin by selecting high-accuracy, non-invasive blood pressure patches compatible with your ICU system, such as those highlighted in latest real-time patches. During my first trial, I scheduled a team training session to familiarize staff with the device, ensuring they understood how to properly affix and calibrate the patch. This hands-on approach minimized initial errors and gathered immediate feedback on comfort and usability.
Calibrate Devices for Peak Accuracy
Calibration is critical. I paired each patch with a gold-standard monitor, running simultaneous readings over several hours. We adjusted device settings based on discrepancies, similar to aligning a musical instrument before performance. In one early trial, improper calibration caused inconsistent readings, highlighting the importance of this step. Regular recalibration ensures sustained precision, especially after system updates or maintenance.
Integrate Devices Into Existing ICU Infrastructure
Seamless integration is key. Connect patches wirelessly to your monitoring stations, ensuring the data streams are streaming correctly. I used a dedicated network segment to avoid interference, akin to creating a private radio station for clear signals. Testing involved monitoring patient data alongside traditional cuffs, verifying real-time synchronization. Proper integration reduces delays and allows staff to respond instantly to fluctuations, transforming patient safety.
Automate Alerts for Critical Changes
Programming alerts based on specific thresholds enhances responsiveness. I used ICU software settings to generate automatic alarms if blood pressure surged or plummeted beyond set limits. During a shift, a sudden spike triggered an immediate audible alert, prompting swift intervention. Fine-tuning these thresholds based on patient conditions prevents false alarms while catching true emergencies, mirroring the tuned sensitivity of a security system.
Establish Regular Maintenance and Staff Training
Consistent upkeep keeps devices reliable. I scheduled weekly checks to verify battery levels, calibration needs, and connectivity, akin to tuning a vehicle before long drives. Continuous training sessions for staff reinforce proper device handling and troubleshooting, much like refresher courses for complex machinery. This proactive approach prevents unexpected failures and keeps your ICU running smoothly, ensuring the high accuracy of real-time data.
Document Data and Outcomes for Continuous Improvement
Maintain detailed records of device performance and patient responses. I tracked readings and alarms in a digital log, analyzing patterns to refine thresholds. Over time, this data helped us identify specific patient vulnerabilities, allowing for tailored monitoring strategies. Consistent documentation supports quality improvement and justifies technology investments, turning raw data into actionable insights.
Many healthcare professionals and enthusiasts often fall into the trap of oversimplifying medical equipment, assuming that once a device is approved or popular, its use and reliability are straightforward. However, there’s a complex web of nuances that can significantly impact outcomes. For instance, the misconception that newer is always better can lead to overlooking tried-and-true devices that might still outperform or complement newer innovations. It’s essential to evaluate devices based on context-specific performance rather than just brand reputation or novelty.
Are All Medical Devices Truly Compatible with Your Environment?
One common mistake is assuming seamless integration without considering environmental factors. For example, a device like rapid cardiac marker tests might perform exceptionally in controlled settings but could face challenges in portable or resource-limited environments. External factors like temperature, humidity, electromagnetic interference, and even user proficiency can alter device performance. Therefore, rigorous validation in real-world settings is crucial, surpassing the basic compliance checks often perceived as sufficient.
Another often-overlooked nuance relates to maintenance and calibration routines. Many assume that devices maintain accuracy over time without routine checks, but studies show that calibration drift can occur within weeks in some models. Regular maintenance schedules, aligned with manufacturer recommendations and contextual demands, are vital for preserving device reliability.
The pitfalls extend beyond operational aspects; financial and ethical considerations also play a role. For example, the procurement of cutting-edge technology like continuous sweat sensors may strain budgets, but their role in proactive patient management can justify the investment. Conversely, employing devices without thorough training can compromise data integrity and patient safety, underscoring the need for comprehensive staff education.
Understanding these nuances also demands acknowledging that no device operates in isolation. Cross-referencing data from multiple sources, like combining continuous monitoring with periodic lab tests ([e.g., lab hoods with air filtration](https://medicaldeviceinsight.com/6-lab-hoods-with-integrated-air-filtration-systems)), provides a broader, more accurate picture. The benefit lies in detecting inconsistencies early and tailoring intervention strategies effectively.
In summary, the key to leveraging medical equipment and devices effectively involves delving beyond surface-level features. Recognize environmental influences, enforce rigorous calibration and maintenance, and contextualize device selection based on patient and operational needs. This approach not only enhances safety and efficacy but also differentiates seasoned practitioners from those still operating on assumptions. Have you ever fallen into this trap? Let me know in the comments.
Keeping Medical Devices in Top Shape
Ensuring your medical equipment operates flawlessly over time requires a combination of precise maintenance routines, the right tools, and informed practices. One of my go-to tools is the eco-friendly lab washer. I rely on it for thorough sterilization of reusable components, which minimizes infection risks and prolongs device lifespan. Regular calibration with standardized reference sources, such as those outlined by the manufacturer, helps maintain measurement accuracy essential for patient safety.
When it comes to long-term results, documenting maintenance activities and device performance is critical. I use a digital log system that tracks calibration dates, repairs, and parts replacements, enabling predictive maintenance and avoiding unexpected failures. This approach aligns with recommendations from expert sources, like the detailed procedures found in ISO 13485 standards, which emphasize systematic device management.
Tools I Recommend for Sustained Device Reliability
One tool I swear by is the portable autoclave. Its portability allows quick on-site sterilization, especially useful in busy clinics or emergency settings. To ensure consistent performance, I perform routine checks on the sterilization cycles and door seals, much like maintaining a household appliance but with the precision required for medical use. Additionally, a high-quality smartphone-linked otoscope enables me to verify imaging quality periodically, reducing diagnostic errors.
In future trends, I predict that integrated IoT sensors will become standard, providing real-time health and maintenance data directly to service technicians—streamlining troubleshooting and reducing downtime. Companies like Philips are already exploring such innovations, and adopting similar technologies can lead to more proactive device management.
How do I maintain medical equipment over time?
Regular preventive maintenance is your best ally. Establish a schedule based on manufacturer recommendations, including routine calibration, component checks, and cleaning protocols. For critical instruments, consider employing advanced diagnostic tools like liquid biopsy kits to monitor potential device wear and tear without invasive procedures. Training staff to recognize early signs of malfunction and fostering a culture of meticulous upkeep are equally vital. Remember, well-maintained equipment not only enhances patient safety but also reduces overall costs by preventing costly repairs and replacements.
To get started, I highly recommend trying out a predictive maintenance strategy using condition-based alerts, especially with devices that have embedded sensors. Initiate with a single device—then expand as you see benefits. Staying ahead in maintenance extends your device’s lifespan and ensures consistent, reliable operation—crucial in today’s fast-paced medical environments.

What the Toughest Days Taught Me
One of the most profound lessons I learned is that no technology is flawless from the start. The real growth happens when we confront unexpected glitches, like calibration drifts or integration hiccups, and adapt quickly. These challenges, though frustrating, pushed me to develop more resilient monitoring protocols and foster a mindset that views problems as opportunities for learning.
Another insight emerged around staff training—initially underestimated, it proved to be the backbone of successful implementation. Hands-on practice, ongoing education, and sharing real-world experiences built confidence and competence, transforming skeptics into advocates for continuous monitoring innovations.
Lastly, I realized that the true power of real-time blood pressure patches lies beyond the device itself. It’s about creating a culture of proactive care—where early detection becomes second nature, and everyone feels empowered to act swiftly. This shift from reactive to anticipatory patient management defines the future of critical care.
Gear Up with These Proven Tools
My toolkit is incomplete without trusted resources that keep me ahead. The detailed articles on rapid cardiac marker tests help me understand diagnostic timelines, while continuous sweat sensors expand my options for non-invasive hydration monitoring. For device sterilization, I rely on eco-friendly lab washers that ensure safety without compromising the environment.
Additionally, I value industry-leading standards like ISO 13485, which underpin best practices for device management. Regularly consulting these authoritative sources ensures my team maintains high reliability standards, ultimately benefiting our patients’ safety and wellbeing.
Trust Your Gut and Keep Moving Forward
The landscape of medical device integration is dynamic and full of potential. The key is to embrace change with curiosity and courage, recognizing that each setback offers valuable lessons. Whether it’s selecting the right wearable patches or fine-tuning calibration procedures, taking decisive action today shapes a safer, more responsive future in critical care. Don’t wait for perfect conditions—start small, learn as you go, and watch new possibilities unfold.